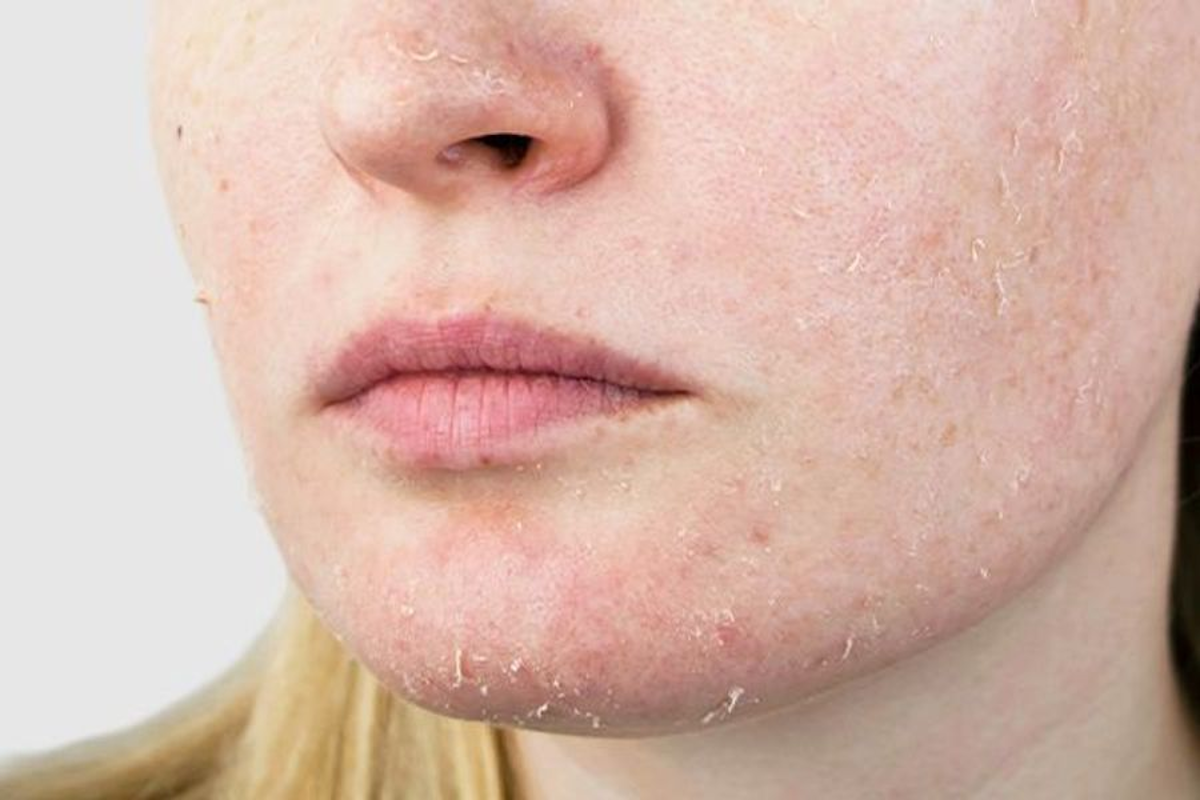
How to Moisturize and Cleanse Your Skin to Prevent Rough Skin: Causes and Skincare Tips
Table of Contents
- Introduction: The Hidden Epidemic of Rough, Dry Skin
- Understanding Your Skin’s Moisture Barrier
- What Causes Rough Skin: Environmental, Lifestyle, and Medical Factors
- Proper Cleansing Methods That Don’t Strip Your Skin
- The Science of Effective Moisturizing for Rough Skin
- Lifestyle Changes to Prevent Dry, Rough Skin
- Treatment Options: From Drugstore to Dermatologist
- Daily Skincare Routines for Different Rough Skin Severities
- Conclusion: Building Your Personalized Rough Skin Prevention Plan
- Frequently Asked Questions
Introduction: The Hidden Epidemic of Rough, Dry Skin
Standing in the pharmacy aisle at eleven o’clock on a Wednesday night, frantically reading moisturizer labels while my hands bled from tiny fissures at each knuckle, I realized that rough, dry skin had escalated from an aesthetic annoyance to a genuine health crisis I could no longer ignore. The cracks hurt with every movement—typing emails sent sharp pains through my fingers, washing dishes became torture despite rubber gloves, and shaking hands during professional meetings left traces of blood on colleagues’ palms that I tried desperately to explain away as “just a little dryness.” This breaking point came after eighteen months of progressively worsening skin roughness that I’d dismissed as temporary winter weather effects, unaware that my daily habits were systematically destroying my skin’s protective moisture barrier faster than it could repair itself. The dermatologist I finally consulted three days later explained that I’d developed xerosis cutis severe enough to require prescription treatment, a condition that affects approximately seventy-five million Americans yet remains dramatically undertreated because most people, like me, assume dry skin is merely cosmetic rather than recognizing it as a medical condition with serious implications for skin barrier integrity and infection risk.
Before delving into the article, watch the following video for some tips on treating severely dry skin:
The statistics surrounding rough, dry skin reveal a problem far more prevalent than most people realize, affecting demographics that extend well beyond the stereotypical elderly population. Research published in 2025 indicates that forty-two percent of adults under age forty now experience chronic dry skin conditions, up from just twenty-eight percent a decade earlier—a dramatic increase dermatologists attribute to lifestyle factors including excessive screen time in climate-controlled environments, over-cleansing driven by pandemic hygiene concerns, and aggressive skincare routines inspired by social media influencers who promote daily exfoliation and active ingredients without adequate moisturizing protocols. The American Academy of Dermatology reports that by age sixty, virtually everyone experiences some degree of skin dryness as sebaceous gland activity declines and cellular turnover slows, but younger individuals increasingly develop rough skin from preventable environmental and behavioral factors rather than inevitable aging. This shift matters because rough, compromised skin doesn’t just feel uncomfortable—it fundamentally weakens your body’s first line of defense against pathogens, allergens, and irritants, creating vulnerability to infections, eczema flares, and chronic inflammatory conditions that extend far beyond surface-level cosmetic concerns.
What makes rough skin particularly insidious is how gradually it develops and how easily people adapt to progressive deterioration without recognizing they’re experiencing an abnormal condition. Your skin should feel soft, pliable, and comfortable throughout the day, maintaining what dermatologists describe as a minimum water content of ten percent and ideally twenty to thirty-five percent in the stratum corneum, the outermost layer that serves as your moisture barrier. When this percentage drops, skin begins feeling tight immediately after cleansing, develops visible flaking that resists makeup application, shows visible cracks or fissures especially around joints and pressure points, appears dull or grayish rather than luminous, and most tellingly, itches persistently despite attempts to scratch or soothe it. These symptoms represent your skin’s distress signals indicating that the protective lipid barrier has become compromised and can no longer effectively prevent transepidermal water loss, the technical term for moisture escaping from deeper skin layers through the damaged surface. Most people experiencing these symptoms assume they simply need to apply hand cream more frequently, not realizing that without addressing the root causes of barrier disruption, topical moisturizers provide only temporary relief rather than lasting repair.
The economic and quality-of-life costs of rough, dry skin extend surprisingly far beyond the price of moisturizers and dermatology appointments. Americans spend approximately two billion dollars annually on over-the-counter dry skin treatments, a figure that doesn’t account for prescription medications, lost productivity from skin conditions causing discomfort and distraction, or the psychological impact of visible skin problems in a culture that places tremendous value on smooth, youthful appearance. Studies tracking patient-reported outcomes reveal that individuals with chronic rough skin experience sleep disruption from nighttime itching, social anxiety about shaking hands or wearing certain clothing that exposes affected areas, and genuine physical pain from deep fissures that interfere with daily activities ranging from typing to exercising to playing with children without wincing. More concerning, severely dry skin creates entry points for bacteria and viruses that healthy skin would normally repel, increasing infection risk particularly among healthcare workers, food handlers, and others who frequently wash hands as part of occupational safety protocols—creating a cruel paradox where necessary hygiene practices destroy the very barrier meant to protect against pathogens.
The National Institute on Aging provides comprehensive guidance on skin changes accompanying the aging process and evidence-based management strategies. Their research demonstrates how skin care and aging intersect, showing that age-related modifications in sebaceous gland activity, cellular turnover rates, and collagen production create unavoidable challenges requiring increasingly proactive moisturizing approaches as individuals progress through their sixties, seventies, and beyond.
This comprehensive guide emerged from extensive research into peer-reviewed dermatological studies, interviews with board-certified dermatologists specializing in barrier repair disorders, and analysis of the latest 2026 treatment protocols that reflect our evolving understanding of skin hydration mechanisms. I’ll explore the precise biological mechanisms that create rough skin, examining how environmental factors, cleansing practices, product choices, and underlying health conditions disrupt your moisture barrier. We’ll investigate evidence-based moisturizing techniques that go far beyond simply slathering on cream, including the optimal timing for application, the correct product selection based on specific skin needs, and the layering sequences that maximize hydration. You’ll learn which common skincare habits unknowingly worsen dry skin despite good intentions, how to identify whether your rough skin stems from external factors you can control or internal conditions requiring medical intervention, and most importantly, how to build a sustainable daily routine that prevents rough skin from developing rather than merely treating it after damage occurs. The goal isn’t just temporary symptom relief but lasting transformation that restores your skin’s natural ability to hydrate itself—because healthy skin shouldn’t require constant intervention to maintain basic comfort and function.
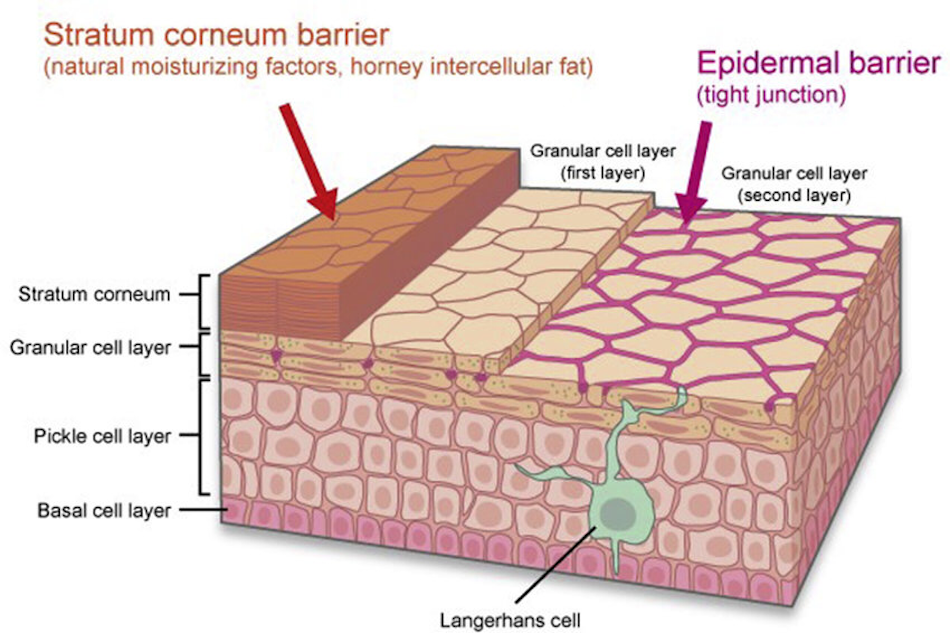
Understanding Your Skin’s Moisture Barrier
The stratum corneum, your skin’s outermost protective layer measuring approximately fifteen to twenty cell layers thick, functions like a brick wall where dead skin cells represent bricks and lipids serve as mortar—a structure dermatologists call the “brick and mortar model” that elegantly explains how healthy skin retains moisture while preventing harmful substances from penetrating. This seemingly simple arrangement performs remarkably complex functions that become apparent only when the system fails, as happens with rough, dry skin. The corneocytes, those dead skin cells that most people incorrectly assume serve no purpose, actually contain natural moisturizing factors including amino acids, lactic acid, urea, and pyrrolidone carboxylic acid that attract and bind water molecules in a process called humectancy. Meanwhile, the intercellular lipids composed of ceramides, cholesterol, and free fatty acids create a water-impermeable seal that prevents the moisture held within corneocytes from evaporating into the surrounding environment—a delicate balance that environmental insults, harsh cleansers, and aging progressively disrupt.
Understanding transepidermal water loss provides the key to comprehending why rough skin develops and, more importantly, how to prevent it. Your skin naturally loses approximately three hundred to four hundred milliliters of water daily through this invisible evaporation process, which serves important thermoregulation and metabolic waste elimination functions under normal circumstances. However, when the lipid barrier becomes compromised through excessive cleansing, environmental exposure, or underlying skin conditions, transepidermal water loss can increase two to ten-fold, overwhelming your body’s ability to replenish moisture from deeper dermal layers. This excessive water loss manifests first as tightness and mild roughness, but if unaddressed, progresses to visible flaking as corneocytes lose their water-binding capacity and literally curl away from the skin surface, then to painful fissures when the brittle, dehydrated cells crack under normal mechanical stress like joint movement or facial expressions. The progression follows a predictable pattern, meaning early intervention during the tightness stage prevents the more serious complications that develop when barrier damage becomes severe.
The natural moisturizing factor composition within your stratum corneum deserves particular attention because it represents your skin’s innate hydration system that topical products attempt to replicate and support. These water-soluble compounds including approximately forty percent amino acids, twelve percent pyrrolidone carboxylic acid, twelve percent lactate, seven percent urea, and smaller percentages of various minerals and sugars work synergistically to maintain optimal hydration levels in healthy skin. When you over-cleanse with harsh soaps or spend extended time in low-humidity environments, you literally wash away or evaporate these natural moisturizing factors faster than your skin can regenerate them, creating a hydration deficit that no amount of water drinking can correct because the problem exists at the skin surface rather than systemically. This explains why some people can drink eight glasses of water daily yet still suffer chronically dry skin—internal hydration supports but cannot substitute for external barrier protection and topical moisture retention.
Sebum production from sebaceous glands scattered throughout your skin except on palms and soles provides another critical component of the moisture retention system that diminishes with age and can be disrupted by skincare practices. Sebum, often vilified in discussions about oily skin and acne, actually serves essential protective functions including creating a lipid film over the stratum corneum that slows transepidermal water loss, delivering vitamin E and other antioxidants to the skin surface, and maintaining the slightly acidic pH around 5.5 that inhibits pathogenic bacterial growth. Sebaceous gland activity peaks during adolescence under hormonal influence, then gradually declines throughout adulthood, with most people experiencing approximately twenty-three percent reduction in sebum production per decade after age twenty. This natural decrease explains why skin that felt balanced or even oily during your twenties often becomes progressively drier through your thirties, forties, and beyond—not necessarily because environmental factors changed but because your internal oil production declined while cleansing habits remained constant or even intensified.
The pH of your skin surface influences moisture retention more significantly than most people realize, with disruption of the normal acidic mantle contributing to rough skin development. Healthy skin maintains a surface pH between 4.5 and 5.5, creating an “acid mantle” that supports beneficial bacterial flora while inhibiting pathogenic organisms and optimizing the enzymatic processes that build and maintain the lipid barrier. Alkaline soaps with pH levels of 9 to 11 temporarily elevate skin pH, requiring approximately ninety minutes for the surface to return to its natural acidic state—and during that window, the compromised barrier allows increased transepidermal water loss. Using highly alkaline cleansers twice daily means your skin spends significant portions of each twenty-four hour period with suboptimal pH and increased vulnerability to moisture loss, creating cumulative damage that manifests as progressive roughness. Modern gentle cleansers and pH-balanced soap-free formulations avoid this problem by maintaining pH close to skin’s natural level, cleaning effectively without creating the alkaline disruption that traditional soaps produce.
Skin thickness variations across different body areas explain why some regions develop roughness more readily than others, requiring adjusted skincare approaches for different zones. Facial skin measures approximately zero-point-twelve millimeters thick on average, while skin on your back can reach four millimeters—a thirty-fold difference that creates dramatically different vulnerability to moisture loss and environmental damage. Delicate areas like eyelids and lips have minimal sebaceous gland density and extremely thin stratum corneum layers, explaining why these regions often show the first signs of dryness even when the rest of your face feels adequately hydrated. Conversely, palms and soles have exceptionally thick stratum corneum lacking sebaceous glands entirely, meaning they depend completely on external moisture sources and develop severe roughness when exposed to frequent wetting and drying cycles or harsh chemicals. Understanding these anatomical differences helps you target skincare efforts appropriately rather than applying a one-size-fits-all approach that over-moisturizes some areas while under-treating others.
The age-related changes in skin barrier function create unavoidable challenges that require increasingly proactive moisturizing strategies as you grow older. Beyond the sebaceous gland activity decline mentioned earlier, cellular turnover rates slow from approximately twenty-eight days in your twenties to forty-five or even sixty days by your sixties, meaning dead surface cells accumulate longer before shedding, creating a thicker but less functional stratum corneum. The natural moisturizing factor production similarly decreases, and the lipid composition of the barrier layer shifts with relatively more cholesterol and less ceramides compared to youthful skin—changes that collectively reduce moisture-binding capacity and increase transepidermal water loss. These inevitable alterations don’t doom you to perpetually rough skin, but they do mean that skincare routines adequate during your twenties require adjustment in subsequent decades, with richer moisturizers, more frequent application, and gentler cleansing becoming necessary to maintain the same level of comfort and barrier integrity that previously required minimal effort.
What Causes Rough Skin: Environmental, Lifestyle, and Medical Factors
Environmental humidity levels profoundly influence skin moisture retention, with winter months presenting the perfect storm of dryness-inducing conditions that dermatologists call “winter xerosis.” Cold outdoor air holds significantly less moisture than warm air—air at twenty degrees Fahrenheit contains roughly sixty percent less water vapor than air at seventy degrees Fahrenheit—creating exceptionally low relative humidity that pulls moisture from your skin’s surface through osmosis. Indoor heating systems compound this problem by warming that already-dry winter air without adding humidity, often reducing indoor relative humidity to ten to twenty percent, comparable to desert climates and far below the forty to sixty percent range considered optimal for skin health. This dual assault from outdoor cold and indoor heating explains why rough skin problems typically peak between December and March in temperate climates, affecting even people whose skin feels comfortable during summer months. Geographic location matters tremendously—residents of humid southeastern states experience far lower rates of winter xerosis than those in dry southwestern deserts or cold northern regions where heating systems run constantly for months.
Excessive bathing and showering represent the single most common behavioral cause of rough, dry skin that dermatologists encounter in their practices, yet patients consistently underestimate how dramatically water exposure affects skin barrier integrity. Each bath or shower, regardless of temperature, temporarily hydrates the stratum corneum as water molecules penetrate between corneocytes—which initially feels pleasant and seems beneficial. However, as that absorbed water evaporates over the subsequent thirty minutes, it carries away natural moisturizing factors and disrupts the lipid barrier, leaving skin drier than before the bath unless you intervene with topical moisturizers. Hot water accelerates this process by dissolving the sebum layer more effectively than lukewarm water, essentially degreasing your skin the same way hot water cuts through oily dishes. Showering for ten to fifteen minutes daily, a common practice among health-conscious individuals who exercise regularly, subjects your skin to approximately seventy to one hundred five minutes of weekly water exposure that systematically strips away natural protection—and if you shower twice daily, you double that assault. Dermatologists treating rough skin typically recommend limiting showers to five to seven minutes every other day when possible, using lukewarm rather than hot water, and immediately applying moisturizer to damp skin within three to five minutes after bathing to trap the temporarily elevated water content before evaporation occurs.
Soap and cleanser chemistry creates another major source of barrier disruption that even people using “gentle” or “moisturizing” products often fail to appreciate. Traditional bar soaps achieve their cleaning action through surfactants with high pH levels around 9 to 11 that emulsify oils, allowing water to wash away both dirt and your protective sebum indiscriminately. Even brief contact with these alkaline cleansers temporarily elevates skin pH from its normal acidic 4.5 to 5.5 range, requiring sixty to ninety minutes for your skin to restore its acid mantle through complex buffering mechanisms. During that recovery period, enzyme systems that build and maintain the lipid barrier function suboptimally, and increased transepidermal water loss occurs—damage that accumulates with each washing if you’re cleansing multiple times daily. Modern syndets, synthetic detergent cleansers designed to match skin’s natural pH, avoid this alkaline disruption while still cleaning effectively, representing a significant improvement over traditional soaps for people prone to dry skin. Medical research on effective dry skin management published in dermatology journals demonstrates that successful treatment requires understanding the skin care routine for dry skin must incorporate barrier-supportive ingredients throughout every step. Prevention Magazine’s dermatologist-consulted guide emphasizes how combining gentle cleansers with strategic moisturizer layering and appropriate active ingredient selection creates comprehensive hydration rather than relying on any single miracle product. Additionally, many supposedly “moisturizing” soaps contain humectants like glycerin but still have alkaline pH and harsh surfactants that strip away far more moisture than the added humectants can replace, making the moisturizing claim technically true but practically misleading.
Occupational factors create rough skin vulnerability for millions of workers whose job requirements systematically damage their skin barriers day after day. Healthcare workers washing hands twenty to forty times per shift to prevent infection transmission experience dramatically elevated rates of hand dermatitis and severe xerosis, with studies showing up to seventy-two percent of nurses report chronic hand dryness and twenty-three percent develop contact dermatitis. Food service employees face similar challenges from frequent handwashing plus exposure to hot water, harsh detergents, and food acids that further compromise skin integrity. Hair stylists contend with chemical exposure from hair dyes, bleaches, and straightening treatments combined with constant water contact, while mechanics and industrial workers deal with petroleum-based solvents and degreasing agents that utterly demolish the lipid barrier. For these occupations, simply moisturizing more frequently provides insufficient protection—effective prevention requires barrier protection through gloves when feasible, immediate moisturizer application after each washing using products specifically formulated for occupational dermatitis prevention, and sometimes preemptive barrier creams applied before work shifts to provide additional protection against chemical and water exposure.
Underlying medical conditions frequently manifest as rough, dry skin before other symptoms become apparent, making persistent xerosis despite appropriate skincare a potential red flag warranting medical evaluation. Hypothyroidism slows cellular metabolism including keratinocyte turnover and sebaceous gland activity, creating characteristic dry, coarse skin particularly prominent on lower legs and arms that many patients notice before classic hypothyroid symptoms like fatigue and weight gain. Diabetes disrupts microvascular circulation and peripheral nerve function, reducing sweat gland activity and creating severely dry feet and lower legs prone to cracking and infection—complications that can be prevented through early diagnosis and glycemic control. Atopic dermatitis, commonly called eczema, stems from genetic mutations affecting filaggrin protein production essential for normal barrier function, leaving affected individuals with chronically dry, sensitive skin requiring lifelong management. Kidney disease reduces vitamin D activation and disrupts calcium and phosphate metabolism, sometimes producing severe itching and dryness called uremic pruritus that affects up to ninety percent of dialysis patients. Recognizing these medical causes matters because while moisturizers provide symptomatic relief, they cannot address the underlying pathology requiring specific medical treatment to truly resolve the skin manifestations.
Medication side effects represent an often-overlooked cause of rough skin that affects millions of people taking commonly prescribed drugs for various health conditions. Diuretics prescribed for hypertension and heart failure promote fluid loss that can manifest as skin dryness, particularly in elderly patients already vulnerable to xerosis from age-related sebaceous gland decline. Retinoids, vitamin A derivatives used for acne and anti-aging, deliberately increase cell turnover and decrease sebum production, creating dose-dependent dryness that requires aggressive compensatory moisturizing to manage. Statins for cholesterol management, antihistamines for allergies, and certain blood pressure medications can all produce dry skin as recognized side effects, though the mechanisms remain incompletely understood. Chemotherapy drugs targeting rapidly dividing cells unfortunately affect skin cells along with cancer cells, producing severe dryness, sensitivity, and increased infection risk during treatment. If your rough skin developed or dramatically worsened after starting a new medication, discuss this timeline with your prescribing physician—sometimes formulation changes, dosage adjustments, or alternative drugs can reduce dermatologic side effects without compromising therapeutic benefits for your primary condition.
Shop on AliExpress via link: wholesale-skincare-moisturizer
Nutritional deficiencies, though less common in developed countries than historical eras, still contribute to rough skin in vulnerable populations and individuals following highly restrictive diets. Essential fatty acid deficiency from extremely low-fat diets impairs cell membrane integrity and barrier lipid production, creating dry, flaky skin along with other health consequences. Vitamin A deficiency reduces sebum production and disrupts normal keratinization, producing characteristic rough, bumpy skin particularly on arms and thighs called follicular hyperkeratosis or “chicken skin.” Vitamin C deficiency interferes with collagen synthesis needed for skin structure and wound healing, creating fragility and roughness. Zinc deficiency produces a constellation of skin symptoms including dryness, delayed wound healing, and increased susceptibility to infections. While frank nutritional deficiencies severe enough to cause clinical symptoms remain rare except among people with malabsorption disorders or extremely limited diets, subclinical insufficiencies may contribute to rough skin in individuals consuming marginally adequate nutrients—making balanced nutrition an important component of comprehensive skin health even though dietary improvements alone rarely resolve established xerosis without concurrent topical treatment.
Genetic predisposition explains why some individuals develop rough skin despite excellent skincare practices while others maintain soft skin with minimal effort. Variations in filaggrin gene expression affect natural moisturizing factor production and barrier integrity, with certain mutations dramatically increasing atopic dermatitis and dry skin risk—conditions that run strongly in families. Sebaceous gland density and activity levels vary substantially between individuals based on genetic factors independent of age or hormone levels, meaning some people naturally produce less protective sebum than others from young adulthood onward. Skin thickness, another genetically determined characteristic, influences vulnerability to environmental damage with thinner skin experiencing greater transepidermal water loss under identical conditions compared to thicker skin. While you cannot change your genetic inheritance, understanding that you have inherent susceptibility to dry skin helps you recognize the need for more proactive prevention rather than waiting for problems to develop before implementing protective measures. Family history of eczema, psoriasis, or severe dry skin should prompt earlier and more aggressive moisturizing protocols, gentler cleansing practices, and heightened attention to environmental humidity control compared to individuals without such genetic loading.
Proper Cleansing Methods That Don’t Strip Your Skin
Cleanser selection represents the foundational decision that determines whether your cleansing routine supports or sabotages skin barrier health, yet most people choose products based on packaging claims rather than understanding ingredient chemistry. Creamy, lotion-based cleansers contain emollients and humectants that deposit moisturizing ingredients while removing dirt and light makeup, making them ideal for dry skin types who need cleaning without degreasing. Gel cleansers with higher surfactant concentrations remove oil more aggressively, serving oily and acne-prone skin better than dry complexions that cannot afford to lose natural sebum. Micellar water uses tiny micelle structures to gently lift away impurities without harsh surfactants or foaming agents, providing excellent option for sensitive dry skin though it may not remove heavy makeup or sunscreen adequately. Cleansing oils follow the “oil dissolves oil” principle, effectively removing makeup and excess sebum while paradoxically leaving skin feeling hydrated rather than stripped—a seemingly counterintuitive result that works remarkably well for dry skin when followed by a gentle secondary cleanse to remove oil residue. Understanding these distinctions helps you match cleanser type to your specific skin needs rather than choosing random products that may work against your hydration goals.
The pH level of cleansers deserves primary consideration for anyone battling rough skin, though most product labels frustratingly omit this crucial specification. As discussed earlier, skin’s natural pH hovers between 4.5 and 5.5, creating the acid mantle that supports barrier function and beneficial bacterial flora. Cleansers with pH above 7 temporarily alkalinize skin surface, disrupting enzyme systems that build the lipid barrier and increasing transepidermal water loss during the recovery period. Traditional bar soaps typically measure pH 9 to 11, while many liquid body washes and facial cleansers range from 6 to 8—both higher than optimal for dry skin. Truly pH-balanced cleansers matching skin’s natural acidity clean effectively without creating alkaline disruption, preserving barrier integrity during cleansing rather than creating damage that subsequent moisturizers must repair. Some specialized “syndet” cleansers explicitly advertise pH 5.5 formulation, but for products lacking pH disclosure, you can purchase inexpensive pH testing strips to measure your current cleansers and make informed decisions about whether they support or undermine your skin barrier health.
Cleansing frequency requires honest assessment of actual dirt and oil accumulation rather than reflexive twice-daily washing that many people perform out of habit regardless of skin condition or lifestyle. Unless you work in environments with significant particulate exposure, exercise vigorously enough to produce copious sweat, or wear heavy makeup daily, you may not need to cleanse both morning and evening—particularly if you have dry skin prone to roughness. Evening cleansing removes accumulated dirt, pollution particles, sunscreen, and makeup that shouldn’t remain on skin overnight, making this session non-negotiable for most people. Morning cleansing often serves more psychological than dermatological purposes, creating a fresh feeling that helps you wake up but potentially stripping away overnight sebum production that would otherwise protect your skin throughout the day. For dry skin types, consider simply rinsing with lukewarm water in the morning or using an extremely gentle micellar water, reserving actual cleanser application for evening when you genuinely need to remove accumulated substances. This frequency reduction alone often produces noticeable improvement in skin roughness within one to two weeks as your barrier has more opportunity to recover between cleansing sessions.
Water temperature during cleansing directly impacts how much natural oil you remove, with temperature differences of just ten to fifteen degrees Fahrenheit creating measurably different barrier disruption levels. Hot water liquefies sebum more effectively than lukewarm water, allowing surfactants to emulsify and remove it more completely—the same principle that makes hot water preferable for washing greasy dishes but problematic for dry skin care. Extremely cold water, while less stripping than hot, may feel uncomfortable and can cause temporary capillary constriction that some people with sensitive skin find irritating. Lukewarm water at approximately eighty-five to ninety-five degrees Fahrenheit, noticeably cooler than typical shower temperature but warmer than room temperature, provides the sweet spot for dry skin cleansing—warm enough to open pores slightly and allow cleanser penetration, but cool enough to avoid excessive sebum dissolution. This temperature recommendation applies to both facial cleansing and body showering, though many people find reducing shower temperature to lukewarm levels psychologically difficult initially, requiring gradual adjustment over several weeks rather than abrupt change.
Cleansing technique influences skin barrier impact nearly as much as product choice, with gentle methods preserving integrity while aggressive scrubbing creates micro-damage that accumulates into chronic roughness. Apply cleanser to damp skin using fingertips rather than washcloths or cleansing brushes, which create excessive mechanical friction despite marketing claims about superior cleaning. Use light circular motions for thirty to sixty seconds—adequate time for surfactants to emulsify oils and dirt without the prolonged rubbing that strips away protective layers. Focus cleanser application on areas that actually accumulate dirt and oil such as T-zone on face, underarms, groin, and feet, avoiding full-body lathering that unnecessarily exposes dry areas like shins and forearms to surfactants when they may need only water rinsing. Rinse thoroughly but briefly, ensuring all cleanser residue removal without excessive water contact—fifteen to twenty seconds per area typically suffices. Pat dry immediately after rinsing rather than allowing prolonged water contact while you complete other shower activities, and never rub skin vigorously with towels, which creates friction damage especially problematic for already-compromised rough skin.
Double cleansing, a technique borrowed from Korean skincare routines, provides effective makeup and sunscreen removal without harsh surfactants by using two gentler cleansers in sequence rather than one aggressive product. Begin with an oil-based cleanser or cleansing balm that dissolves makeup, sunscreen, and sebum through lipophilic attraction, massaging gently for thirty to sixty seconds before adding water to emulsify and rinse. Follow with a mild water-based cleanser to remove any remaining oil residue and water-soluble impurities, again using gentle motions for thirty to sixty seconds before rinsing. This two-step process effectively cleans skin more thoroughly than single cleansing with harsh surfactants while paradoxically leaving skin feeling softer and more hydrated rather than stripped—the gentler individual cleansers create less barrier disruption than the aggressive surfactants required to remove modern long-wear makeup and water-resistant sunscreens in a single step. For rough, dry skin, double cleansing in the evening after wearing makeup or sunscreen often works better than attempting to find a single cleanser strong enough to remove everything yet gentle enough to avoid excessive drying.
Cleansing tool selection matters more than skincare marketing would have you believe, with most mechanical cleansing devices creating unnecessary friction that worsens rather than improves dry skin conditions. Washcloths, loofahs, exfoliating gloves, and spinning brush devices all create mechanical abrasion that marketing materials describe as beneficial exfoliation but that dermatologists recognize as potential barrier damage, particularly for already-rough skin. Your fingertips provide adequate gentle mechanical action for effective cleansing without the excessive friction that tools create—and fingertips have the advantage of tactile feedback that helps you feel when you’re rubbing too hard, something tools lack. If you strongly prefer using a cloth for psychological reasons, choose soft microfiber or muslin rather than terry cloth or textured varieties, use extremely light pressure, and limit to a few times weekly rather than daily. Chemical exfoliation through gentle alpha-hydroxy acids like lactic acid serves dry skin far better than mechanical scrubbing, removing dead cell accumulation without creating the friction damage that mechanical methods produce.
Post-cleansing timing for moisturizer application significantly influences how effectively you combat rough skin, with dermatologists consistently recommending the “three-minute rule” that most patients ignore. Immediately after cleansing, your stratum corneum temporarily holds elevated water content that begins evaporating within minutes—and as that water evaporates, it carries away natural moisturizing factors and disrupts the lipid barrier unless you intervene quickly. Applying moisturizer to this damp, plumped skin within three to five minutes creates an occlusive seal that traps the temporarily elevated moisture content, essentially “locking in” the hydration boost that cleansing provided before evaporation can occur. Waiting until skin feels completely dry before moisturizing, a common mistake that people make while completing other bathroom routines, allows this opportunity to pass as transepidermal water loss peaks during the ten to fifteen minutes post-cleansing. This timing consideration matters enough that you should plan your cleansing routine to ensure moisturizer stands ready for immediate application—laying out your products before showering, keeping face moisturizer at the bathroom sink rather than bedroom dresser, and prioritizing moisturizing over other post-shower activities like hair styling or dressing.
The Science of Effective Moisturizing for Rough Skin
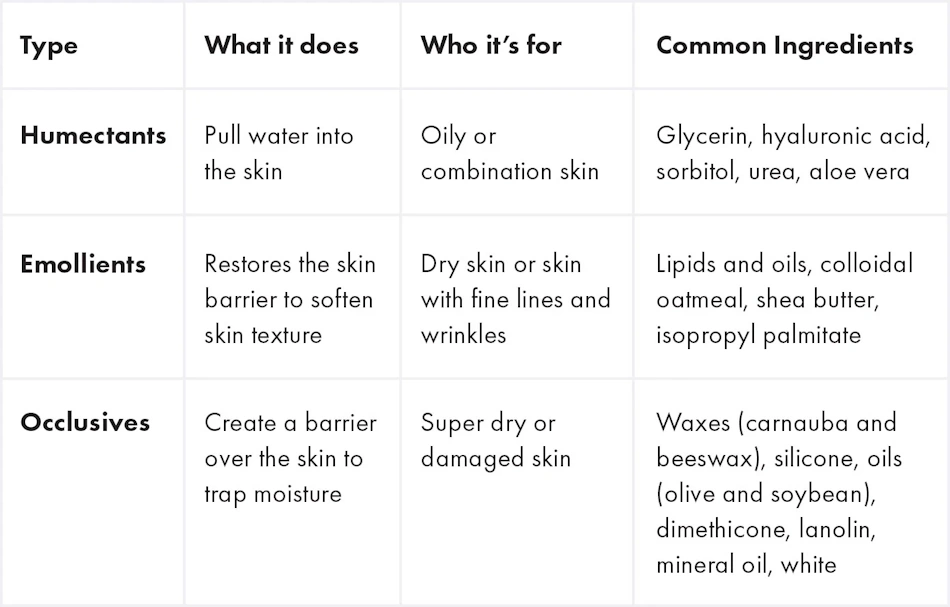
Moisturizer ingredient categories work through distinct mechanisms that understanding helps you select products matching your specific rough skin needs rather than choosing based on brand names or packaging aesthetics. Humectants including hyaluronic acid, glycerin, urea, and panthenol attract and bind water molecules from the environment or deeper skin layers, drawing moisture to the stratum corneum and temporarily plumping surface cells. These ingredients work brilliantly in humid environments where atmospheric water vapor provides abundant moisture to attract, but can paradoxically worsen dryness in low-humidity settings by pulling water from deeper skin layers without adequate external source to replace what evaporates. Emollients such as ceramides, squalane, cholesterol, and various fatty acids smooth rough texture by filling spaces between corneocytes and replenishing the lipid barrier components that have been depleted, directly addressing the structural deficits creating roughness. Occlusives including petrolatum, mineral oil, lanolin, and dimethicone create a physical barrier over skin surface that prevents transepidermal water loss, sealing in moisture rather than attracting it—these ingredients provide the most immediate relief for severely dry skin but can feel heavy or greasy, particularly on face. Effective moisturizers for rough skin typically combine all three categories, using humectants to attract water, emollients to repair barrier structure, and occlusives to prevent moisture loss, creating comprehensive hydration rather than relying on single-mechanism action.
Moisturizer formulation viscosity provides practical guidance for matching products to rough skin severity, with thicker products generally providing more intensive treatment suitable for more severe conditions. Lotions, the thinnest formulation, contain high water content that spreads easily and absorbs quickly but provides relatively modest occlusive protection, making them suitable for mild dryness or facial use where heavy products would feel uncomfortable. Creams contain less water and more oil than lotions, offering increased occlusive protection and emollient benefit while remaining spreadable and comfortable for most body areas—these represent the middle ground appropriate for moderate dry skin affecting most people with roughness concerns. Ointments contain minimal water and maximal oil content, often petroleum-based, creating superior occlusive barriers that provide maximum moisture retention but feel greasy and may stain clothing, best reserved for severely dry areas like hands, feet, and elbows where intensive treatment outweighs cosmetic concerns about product feel. Balms and salves similar to ointments use plant-based oils and waxes rather than petroleum, offering comparable occlusive benefits with different sensory characteristics some people prefer. The general principle suggests matching formulation thickness to problem severity—using thinnest products that control your symptoms to avoid unnecessary greasiness, but not hesitating to step up to thicker formulations if lighter options fail to provide adequate relief.
Application technique influences moisturizer effectiveness beyond simple product choice, with method and timing creating measurable differences in hydration outcomes. Apply moisturizer to damp skin immediately after bathing as discussed in the cleansing section, but also consider layering techniques that maximize penetration and retention. For face, apply thinner serums first while skin is wettest, allowing sixty seconds for initial absorption before layering thicker creams, creating a gradient from lightweight humectants that penetrate deepest to heavier occlusives that seal everything in. For body, consider applying richest products to problem areas like shins, elbows, and knees immediately after showering while those areas remain damp, then applying lighter body lotion to less-affected areas once you’ve dried off more thoroughly. Use enough product to create a thin visible layer initially, massaging gently until absorbed—underapplication represents the most common mistake people make, using cosmetically elegant amounts that feel comfortable but provide insufficient actual hydration. For severely rough areas, consider occlusive techniques like applying thick ointment to hands or feet at bedtime, then covering with cotton gloves or socks to prevent transfer to bedding while creating mini-occlusive chambers that maximize penetration overnight.
Moisturizing frequency demands honesty about your specific needs rather than following generic twice-daily recommendations that may prove insufficient for rough skin. At minimum, moisturize immediately after bathing and again before bed, capitalizing on the post-cleansing window and overnight repair period when cell turnover peaks and transepidermal water loss naturally increases. However, rough skin often requires additional midday applications, particularly for hands subjected to frequent washing, and reapplication after activities causing excessive water contact or sweating that depletes surface moisture. Listen to your skin’s signals—tightness, visible flaking, or discomfort indicate need for immediate moisturizing regardless of how recently you last applied product. Unlike some skincare actives where more isn’t better and excess causes problems, moisturizers rarely create issues from overuse assuming you’re using appropriate non-comedogenic formulations for your skin type. The principle “moisturize whenever your skin feels dry or uncomfortable” serves rough skin better than rigid schedules that may leave you under-treated during high-stress periods while potentially over-treating during favorable conditions.
Ingredient selection for rough skin requires avoiding common irritants that exacerbate barrier dysfunction even if they appear in moisturizers marketed toward dry skin. Fragrance, whether synthetic or natural essential oils, represents the most common contact allergen in skincare products, capable of triggering irritation and sensitization reactions that worsen rather than improve rough skin—yet appears in countless moisturizers because consumers prefer pleasant-scented products. Alcohol, particularly denatured alcohol and alcohol denat, causes immediate drying and ongoing barrier disruption, having no place in moisturizers for dry skin despite appearing in some gel-cream formulations marketed for combination skin. Certain preservatives including formaldehyde-releasing agents, methylisothiazolinone, and some parabens trigger allergic reactions in susceptible individuals, creating eczematous changes that mimic or worsen xerosis. High concentrations of alpha-hydroxy acids or retinoids, while beneficial for exfoliation and anti-aging, require careful introduction into rough skin routines since they increase cell turnover and temporarily worsen dryness before improving texture—these actives work best when introduced gradually after establishing solid baseline hydration, not as first-line treatments for already-compromised skin.
Specialized moisturizers targeting specific rough skin scenarios provide advantages over generic formulations, though marketing hype requires critical evaluation to distinguish genuine innovation from repackaging. Urea-containing creams at concentrations of 5 to 40 percent combine humectant properties with gentle keratolytic action, simultaneously attracting moisture and dissolving the intercellular cement holding dead cells together to improve penetration of other ingredients—particularly effective for rough heels, elbows, and severely dry body areas. Clinical research published by the National Institutes of Health examines the pathophysiology of xeroderma at molecular levels, revealing how deficiencies in the skin’s hydrolipid content create the characteristic roughness, tightness, and flaking that define this prevalent condition affecting millions worldwide. Their findings on xeroderma mechanisms inform evidence-based treatment protocols emphasizing moisturizer selection based on specific barrier repair ingredients rather than marketing claims. Ceramide-dominant formulations specifically replenish the lipid components most critical for barrier integrity, making them theoretically superior for true barrier repair disorders like eczema compared to generic emollient creams, though actual clinical benefit depends on ceramide type, concentration, and formulation that allows skin penetration. Colloidal oatmeal preparations soothe inflammation and itching while providing mild cleansing and moisturizing benefits, offering particular value for rough skin complicated by itch or sensitivity where standard moisturizers feel irritating. Prescription-strength moisturizers containing lactic acid or ammonium lactate combine alpha-hydroxy acid exfoliation with humectant action, more aggressively addressing severe roughness than over-the-counter options but requiring physician supervision to avoid over-exfoliation reactions.
Body area customization recognizes that different skin regions have distinct needs based on thickness, sebaceous gland density, and exposure patterns that one-size-fits-all moisturizing ignores. Face requires lighter, non-comedogenic formulations that won’t clog pores or interfere with makeup application, even if you have dry skin—heavy body creams appropriate for legs will cause breakouts if applied to facial skin. Hands need frequent reapplication due to constant washing but also require fast-absorbing formulations since greasy hands interfere with daily activities—look for hand creams specifically designed to absorb within sixty seconds while providing lasting protection. Feet with their exceptionally thick stratum corneum and complete lack of sebaceous glands benefit from the richest available ointments, particularly on heels prone to severe cracking, where intensive overnight occlusive treatments using thick products covered by socks provide optimal results. Lips require specialized balms with high oil content and sun protection, since the vermillion border lacks both sebaceous glands and melanin protection, making it uniquely vulnerable to drying and sun damage. Tailoring products to these distinct regional needs works better than applying the same moisturizer everywhere, allowing optimization for each area’s specific requirements and constraints.
Shop on AliExpress via link: wholesale-hyaluronic-acid-serum
Lifestyle Changes to Prevent Dry, Rough Skin
Indoor humidity control represents perhaps the single most impactful environmental modification for preventing winter xerosis, yet most people overlook this intervention in favor of topical treatments alone. Central heating systems warm air without adding moisture, reducing relative humidity to desert-like levels of 10 to 20 percent that aggressively pull moisture from your skin regardless of how much moisturizer you apply. Portable humidifiers in bedrooms where you spend eight hours nightly sleeping can maintain humidity around 40 to 50 percent optimal for skin health, dramatically reducing nighttime transepidermal water loss when cellular repair processes peak and skin naturally loses more water than during daytime. Whole-house humidifiers integrated with central heating systems provide comprehensive humidity control throughout your living space, representing significant upfront investment but offering superior long-term convenience compared to managing multiple portable units. Monitor humidity levels using inexpensive hygrometers to ensure you’re maintaining the target 40 to 60 percent range—too low provides insufficient protection while excessive humidity above 60 percent promotes mold growth and dust mite proliferation. Clean humidifiers weekly following manufacturer instructions to prevent bacterial and fungal contamination that can aerosolize pathogens, creating respiratory problems that outweigh skin benefits.
Sleep environment optimization extends beyond humidity to include bedding choices, room temperature, and pre-bedtime skincare rituals that either support or sabotage overnight skin repair. Cotton sheets and pillowcases allow better air circulation than synthetic fabrics while avoiding the mechanical irritation that rough linen or low-thread-count materials create, providing gentle environment for skin regeneration. Room temperature between 60 and 67 degrees Fahrenheit promotes optimal sleep quality while avoiding excessive heat that increases insensible water loss and nighttime sweating that can irritate already-dry skin. Intensive nighttime moisturizing takes advantage of the extended period when skin isn’t exposed to environmental stressors, environmental pollutants, makeup, or frequent handwashing—apply richer formulations before bed than you’d tolerate during the day, knowing absorption will occur during sleep hours without cosmetic concerns about greasy appearance. For severely dry hands or feet, overnight occlusive therapy using thick ointments covered with cotton gloves or socks creates mini-humid chambers that dramatically accelerate barrier repair, often producing noticeable improvement after just a single night and transformative results within a week of consistent application.
Mayo Clinic’s evidence-based treatment protocols demonstrate how addressing dry skin requires comprehensive approach beyond simple moisturizer application. Their clinical guidance on dry skin management emphasizes proper bathing techniques including water temperature control, cleanser pH selection, and the critical timing of moisturizer application within minutes of cleansing to maximize hydration benefit while minimizing transepidermal water loss.
Clothing choices influence skin moisture retention more than most people realize, with fabric selection, fit, and laundering practices all impacting dry skin severity. Natural fibers including cotton, silk, and bamboo allow skin to breathe while wicking moisture away from the surface, maintaining comfortable microclimate without trapping sweat that can irritate dry skin. Wool, despite being natural, can feel scratchy and irritating to sensitive dry skin, working better as an outer layer over cotton rather than directly against skin—though high-quality merino wool processes create softer fibers that some dry-skin individuals tolerate well. Synthetic fabrics like polyester and nylon trap heat and moisture, creating uncomfortable humid conditions that paradoxically can worsen dry skin by promoting sweat that irritates compromised barriers. Loose-fitting clothing reduces friction against rough skin compared to tight garments that create constant mechanical irritation, particularly important for areas like thighs, underarms, and torso where fabric constantly contacts skin during movement. Laundry detergent selection matters surprisingly—use fragrance-free, dye-free formulations specifically marketed for sensitive skin, skip fabric softeners that deposit coating chemicals, and ensure thorough rinsing to remove all detergent residue that can act as skin irritants.
Sun protection represents a year-round necessity for maintaining skin barrier health, not merely a summer beach concern, with ultraviolet radiation contributing significantly to premature skin aging and dryness. UV exposure degrades collagen and elastin fibers that provide skin structure, disrupts the lipid barrier organization, generates inflammatory mediators that damage keratinocytes, and increases transepidermal water loss—cumulative effects that manifest as dry, rough, prematurely aged skin. Winter sun reflecting off snow creates surprisingly high UV exposure levels despite cooler temperatures, while summer activities concentrate exposure during peak intensity hours. Daily broad-spectrum sunscreen with SPF 30 minimum should become as automatic as tooth brushing, with reapplication every two hours during extended outdoor exposure. Moisturizers containing sunscreen provide convenient combination products for facial protection, but ensure adequate application since most people apply far less than the recommended one-fourth teaspoon for face and neck. Protective clothing including wide-brimmed hats and long sleeves offers superior protection compared to sunscreen alone for prolonged outdoor activities, particularly relevant given that sunscreens themselves can dry sensitive skin despite protective benefits—mineral formulations with zinc oxide or titanium dioxide typically irritate dry skin less than chemical sunscreens containing avobenzone, oxybenzone, or octinoxate.
Hydration and nutrition influence skin moisture from inside, providing foundational support for topical treatments though unable to substitute for proper external care. Adequate water intake supporting cellular function throughout the body including skin cells, with most adults requiring approximately eight eight-ounce glasses daily though individual needs vary based on climate, activity level, and other factors. However, drinking excessive water beyond replacing actual losses provides no additional skin benefit since your body prioritizes water delivery to vital organs over skin, making topical hydration more direct and effective than oral for addressing surface dryness. Omega-3 fatty acids from fish, walnuts, and flaxseeds support cell membrane integrity and reduce inflammatory mediators that can disrupt barrier function, making dietary inclusion beneficial though effects develop gradually over weeks rather than immediately. Vitamins A, C, D, and E all contribute to skin health through antioxidant effects, collagen synthesis support, and barrier function optimization, ideally consumed through balanced diet though supplementation may benefit individuals with restricted eating patterns or malabsorption conditions. Severe caloric restriction, very low-fat diets below 15 percent of calories from fat, or highly restrictive elimination diets risk nutritional deficiencies that can manifest as dry skin among other symptoms, suggesting balanced eating serves skin health better than extreme dietary approaches.
Stress management deserves consideration given emerging research on the skin-mind connection and stress hormone effects on barrier function. Chronic psychological stress elevates cortisol levels that impair lipid synthesis needed for barrier repair, reduce skin’s ability to hold moisture, and slow wound healing processes that would normally repair rough, cracked areas. Stress also triggers behavioral changes including decreased skincare routine adherence, increased hand-to-face touching that spreads bacteria and irritates skin, and sleep disruption that impairs overnight repair processes. While you cannot eliminate all stress from modern life, implementing stress reduction techniques including regular exercise, meditation, adequate sleep, and leisure activities can indirectly support skin health alongside direct dermatologic benefits. Recent dermatology research examining dry skin management approaches published through academic medical centers confirms that comprehensive skin care protocols combining multiple barrier-repair mechanisms achieve superior outcomes compared to single-intervention strategies. Harvard Health’s analysis of dry skin treatment demonstrates how understanding sebum production, natural moisturizing factors, and environmental humidity interactions enables targeted interventions addressing specific deficiency patterns rather than generic moisturizing approaches. Additionally, stress about skin problems themselves creates vicious cycles where anxiety over appearance worsens the condition, making psychological acceptance and rational response to skin issues part of effective management rather than purely focusing on physical interventions.
Exercise benefits skin health through improved circulation delivering nutrients and oxygen to skin cells, enhanced lymphatic drainage removing metabolic waste products, and stress reduction effects mentioned above. However, exercise also creates challenges for rough skin through increased sweating, frequent showering post-workout, and environmental exposures in pools, gyms, or outdoor conditions that can worsen dryness. Minimize negative impacts by showering as soon as practical after exercise before sweat can irritate compromised barriers, using lukewarm water and gentle cleansers rather than aggressive scrubbing, moisturizing immediately after showering, and staying well-hydrated throughout workouts to support normal skin function. Indoor swimmers face particular challenges from chlorine exposure that strips oils and dries skin aggressively—rinse immediately after pool exposure, use specialized chlorine-removing body washes, apply rich moisturizers, and consider pre-swim barrier creams that protect skin from chemical exposure without interfering with swimming performance.
Treatment Options: From Drugstore to Dermatologist
Over-the-counter moisturizers represent first-line treatment for rough skin, with several specific product categories proven effective through clinical research despite their drugstore accessibility. Petroleum jelly, humble and inexpensive, provides arguably the most effective occlusive barrier available without prescription, preventing approximately 98 percent of transepidermal water loss when applied to damp skin—particularly valuable for severely dry hands, feet, and lips where cosmetic elegance matters less than intensive healing. Urea creams at 10 to 20 percent concentration combine humectant and gentle exfoliant properties, softening rough patches while improving penetration of other ingredients, available over-the-counter and effective for moderate xerosis though higher concentrations may sting initially on very dry, cracked skin. Ceramide-containing moisturizers specifically replenish the lipid components most critical for barrier function, with research showing superior improvement in barrier repair markers compared to generic moisturizers, available from multiple brands at various price points making them accessible while offering targeted repair. Colloidal oatmeal formulations soothe inflammation and reduce itch associated with rough skin while providing gentle cleansing and moisturizing, particularly helpful when xerosis triggers scratching that worsens barrier damage. Lactic acid or ammonium lactate lotions at 5 to 12 percent concentration combine alpha-hydroxy acid exfoliation with humectant benefits, smoothing roughness more aggressively than plain moisturizers, available over-the-counter though some people experience mild stinging initially.
Prescription treatments become necessary when over-the-counter approaches fail to control rough skin after four weeks of consistent use, or when underlying medical conditions require diagnosis and specific therapy. Prescription-strength urea at concentrations of 30 to 40 percent provides more aggressive keratolytic action for severely hyperkeratotic areas like heels with deep fissures, though high concentrations can irritate and require gradual introduction under medical supervision. Topical corticosteroids at various potencies reduce inflammation that often accompanies severe dry skin, providing rapid symptom relief though long-term use carries risks of skin thinning and other side effects requiring careful monitoring. Tacrolimus and pimecrolimus, nonsteroidal anti-inflammatory creams, treat inflammatory components of conditions like eczema that manifest as dry, rough skin without steroid side effects, particularly useful for sensitive areas like face where corticosteroid risks are highest. Prescription retinoids, though initially drying, eventually improve skin texture and normalize keratinization in conditions involving abnormal rough patches, requiring expert guidance for appropriate introduction and concurrent intensive moisturizing. Crisaborole, a relatively new phosphodiesterase-4 inhibitor, treats atopic dermatitis including its dry skin component through anti-inflammatory mechanisms distinct from steroids or calcineurin inhibitors, expanding prescription options for difficult cases.
Identifying when to escalate from self-care to professional evaluation requires recognizing specific warning signs that suggest your rough skin needs medical assessment. Persistence despite four weeks of consistent, appropriate home treatment including gentle cleansing and regular moisturizing with quality products indicates the need for dermatologic evaluation to identify underlying causes or access prescription therapies. Painful cracking that bleeds or creates open wounds carries infection risk requiring medical attention to prevent complications like cellulitis that can develop when bacteria enter through compromised barriers. Severe itching disrupting sleep or daily activities despite moisturizing and over-the-counter anti-itch treatments suggests inflammatory conditions like eczema or contact dermatitis requiring prescription management. Sudden onset of widespread dry skin without obvious environmental triggers could indicate underlying medical conditions like thyroid disorders, diabetes, or kidney disease needing systemic evaluation beyond just dermatologic treatment. Failure of specific body areas like hands to improve despite treatment when the rest of your skin responds appropriately might indicate occupational dermatitis, allergic contact dermatitis, or other localized conditions requiring patch testing and specialized intervention.
Professional treatments available through dermatology practices provide options beyond topical medications for rough skin resistant to standard approaches. Phototherapy using controlled ultraviolet light exposure helps certain dry skin conditions including eczema and psoriasis by modulating immune responses and normalizing keratinization, requiring multiple sessions weekly for several weeks under careful medical supervision to balance benefits against UV risks. Prescription oral medications including immunosuppressants for severe eczema or systemic retinoids for severe psoriasis address underlying pathology driving rough skin when topical treatments provide insufficient control. Wet wrap therapy, a dermatologist-supervised technique applying moisturizers followed by damp wraps and dry layers, dramatically accelerates barrier repair for severely dry skin, sometimes used in clinical settings for crisis intervention before transitioning to home maintenance regimens. Allergen identification through patch testing helps patients with rough skin triggered by allergic contact dermatitis identify specific substances to avoid, potentially resolving conditions that have resisted treatment because underlying allergen exposure continued. Nutritional assessment and supplementation for identified deficiencies addresses dry skin stemming from inadequate essential fatty acids, vitamins, or minerals, though rarely needed for well-nourished individuals in developed countries.
Alternative and complementary approaches warrant evidence-based consideration, distinguishing legitimate therapies from unproven or potentially harmful practices. Medical-grade probiotics show emerging evidence for supporting skin barrier function and reducing eczema severity through gut-skin axis mechanisms, though optimal strains, dosing, and patient selection remain under investigation. Evening primrose oil and borage oil containing gamma-linolenic acid demonstrate modest benefit in some studies of atopic dermatitis including associated dryness, though results remain inconsistent and these supplements may interact with blood-thinning medications. Acupuncture shows preliminary evidence for reducing itch associated with dry skin conditions in limited studies, offering potential adjunct option for patients interested in complementary approaches though requiring qualified practitioners. Conversely, certain popular natural remedies lack evidence or carry risks—coconut oil while generally safe can worsen acne-prone skin, apple cider vinegar at popular dilutions still has pH too acidic for damaged skin causing irritation, and many essential oils trigger allergic reactions despite “natural” marketing. When considering complementary approaches, discuss with your dermatologist to ensure compatibility with medical treatment and avoid potentially harmful interactions or substitutions that delay effective therapy.
Cost-effectiveness analysis helps prioritize treatment investments since rough skin management represents ongoing rather than one-time expense. Generic petroleum jelly at under five dollars per pound provides exceptionally cost-effective intensive treatment for severely dry areas, outperforming many expensive specialty creams in terms of occlusive barrier protection per dollar spent. Mid-range ceramide moisturizers from brands like CeraVe or Cetaphil offer scientifically-supported barrier repair ingredients at approximately fifteen to twenty dollars per bottle, representing good value for face and selective body areas though becoming expensive for whole-body application. Prescription treatments covered by insurance often cost less than expensive over-the-counter specialty products marketed for dry skin, making professional evaluation financially sensible if you’re already spending significant amounts on ineffective products. Generic versions of prescription medications cost substantially less than brand names while containing identical active ingredients, with lactic acid lotion generic costing approximately twenty dollars compared to eighty dollars for branded AmLactin. Whole-house humidifiers represent significant upfront investment of several hundred dollars but eliminate ongoing portable unit costs while providing superior humidity control, potentially justifying expense for families where multiple members struggle with winter dry skin.
Daily Skincare Routines for Different Rough Skin Severities
Mild dry skin affecting limited areas or occurring seasonally responds to simplified routines focusing on gentle cleansing and consistent moisturizing without extensive product layering or intensive treatments. Morning routine should begin with lukewarm water rinse or gentle micellar water cleansing if your face feels oily, avoiding full cleansing that strips natural overnight sebum production unless truly necessary. Apply lightweight moisturizer with humectants like hyaluronic acid and gentle emollients to damp skin, allowing two to three minutes for absorption before applying broad-spectrum SPF 30 sunscreen or combination moisturizer-sunscreen product. For body, simply rinse or skip showering entirely on days without exercise or significant dirt exposure, applying body lotion to any areas feeling tight or rough but not necessarily whole-body moisturizing if skin feels comfortable. Evening routine involves gentle cleansing with creamy, pH-balanced cleanser, patting skin damp-dry, and immediately applying slightly richer moisturizer than morning since overnight represents repair period and cosmetic elegance matters less. Target problem-prone areas like shins, elbows, and knees with thicker cream while using lighter formulations on areas that don’t typically dry out, customizing rather than one-size-fits-all application.
Moderate dry skin involving more extensive body areas or accompanied by visible flaking and discomfort requires more structured routine with layered products targeting different hydration mechanisms. Morning begins with brief lukewarm shower every other day rather than daily, using creamy syndet cleanser only on areas truly needing cleaning, limiting time to five to seven minutes maximum. Pat skin damp while still in humid bathroom environment, immediately apply humectant serum like hyaluronic acid to face while skin remains wet, wait sixty seconds for initial absorption, then layer regular moisturizer over serum creating humectant-emollient-occlusive gradient. Apply rich body cream to entire body within three minutes of showering while skin retains elevated water content, using thickest formulations on predictably dry areas like lower legs, hands, and arms. Reapply hand cream after each handwashing throughout day—keep small tubes at every sink, in car, at work desk enabling frequent reapplication without inconvenience excuses. Evening involves thorough but gentle cleansing to remove accumulated dirt, sunscreen, and environmental pollutants, followed by more intensive moisturizing than morning. For face, consider gentle chemical exfoliant like lactic acid serum two to three times weekly before moisturizing to improve product penetration, always followed by extra moisturizer since exfoliation temporarily increases transepidermal water loss. Apply richest available night cream or facial oil as final layer to seal everything in during overnight repair period.
Severe dry skin manifesting as painful cracking, widespread roughness, or diagnosed conditions like eczema demands intensive multi-step routine with specialized products and potentially prescription treatments under dermatologic supervision. Morning begins with cream cleansing rather than water-based washing, using cleansing cream that dissolves dirt through oil attraction then tissues off without water contact, avoiding even brief water exposure that can worsen severely compromised barriers. Layer multiple products targeting different mechanisms—start with prescription or specialized serum addressing underlying condition, wait two to three minutes for absorption, apply ceramide-rich barrier repair cream, wait another two minutes, finish with occlusive ointment on severely affected areas like hands and feet. Protect hands throughout day with cotton gloves under rubber gloves during wet work, barrier creams before anticipated irritant exposure, and immediate reapplication of moisturizer after any washing or irritant contact. Midday maintenance requires carrying intensive hand cream for frequent reapplication, facial mist to add quick hydration boost without disturbing makeup, and awareness of environmental triggers like excessive heating or air conditioning prompting protective measures. Evening involves oil cleansing to avoid water and harsh surfactants, followed by multi-step treatment application—medicated products if prescribed, followed by specialized barrier repair products, then thick occlusive ointment on worst areas. Employ occlusive therapy techniques at least several nights weekly—applying thick layer of petroleum-based ointment to hands or feet, covering with cotton gloves or socks, leaving overnight to create intensive repair environment. Weekly treatments might include gentle at-home peels with lactic acid for controlled exfoliation, sheet masks providing intensive hydration boost, or prescribed wet-wrap therapy sessions per dermatologist instructions.
Seasonal adjustments recognize that skin needs change with environmental conditions requiring routine modification rather than year-round identical approach. Winter requires intensified routine with richer products, more frequent application, whole-house or bedroom humidification, and potentially shorter, less frequent bathing than summer months. Switch from lightweight lotions to heavier creams or ointments for both face and body, add facial oils or overnight masks to evening routine, and employ occlusive hand and foot treatments more frequently. Summer allows lighter products with higher water content that feel more comfortable in heat and humidity, potentially more frequent cleansing if sweating or swimming, but continued attention to post-sun hydration and sunscreen compliance. Spring and fall transition periods require flexibility, adjusting products as environmental humidity shifts rather than rigid seasonal switching dates—pay attention to how your skin feels and modify routine responsively. Geographic variations matter tremendously—arid southwestern climates demand more intensive year-round moisturizing than humid southeastern regions where summer humidity might allow minimal routine while winter heating still causes problems. International travelers should anticipate increased dryness from airplane cabin low humidity, hotel air conditioning, and climate differences from home, packing intensive moisturizers and adjusting routine proactively rather than reactively after skin has already become uncomfortably dry.
Product minimalism versus extensive routine represents an ongoing debate in skincare communities, with evidence supporting effectiveness of simple three-to-four product routines for most people compared to ten-plus product layering marketed through social media. For dry skin, effective minimal routine consists of gentle cleanser, quality moisturizer with multiple hydration mechanisms, and broad-spectrum sunscreen—three products covering essential needs without unnecessary complexity or expense. Adding a fourth product like chemical exfoliant or specialized treatment serum makes sense for specific concerns but rarely do you need the extensive multi-step routines popular among beauty influencers. Excessive layering creates several problems including increased cumulative cost, higher likelihood of product interactions causing irritation, difficulty identifying which product causes problems if reactions occur, and time requirements making routine unsustainable long-term. Quality matters more than quantity—one excellent ceramide cream outperforms five mediocre lotions layered together, and simple routines you’ll actually maintain consistently beat elaborate protocols you abandon after two weeks due to complexity fatigue. Focus on finding genuinely effective gentle cleanser, truly moisturizing cream with proven barrier-repair ingredients, and reliable sunscreen rather than accumulating trendy products marketed through clever advertising but lacking substance.
Troubleshooting routine resistance when your skin fails to improve despite seemingly appropriate efforts requires systematic evaluation of potential problems. Ensure adequate quantity application—most people use far too little moisturizer for effective hydration, needing approximately one-quarter teaspoon for face and neck, palmful for each arm or leg, creating initially visible layer rather than cosmetically elegant thin film. Verify appropriate product selection for your skin type—using lightweight gel moisturizer marketed for oily skin won’t hydrate dry skin adequately regardless of how frequently you apply it. Examine timing—applying moisturizer thirty minutes after bathing when skin has dried completely misses the critical window for trapping moisture. Consider hidden irritants including fragrance in supposedly gentle products, fabric softener residue in clothing, or hand soap at work differing from gentle home cleanser, systematically eliminating suspects. Evaluate environmental factors beyond your direct control like workplace humidity, exposure to harsh chemicals, or medical conditions requiring frequent handwashing that overwhelm even good home routine. When systematic troubleshooting fails to yield improvement, professional dermatologic evaluation becomes necessary to identify underlying conditions, prescribe appropriate treatments, and rule out medical causes requiring different intervention than cosmetic dry skin.
Conclusion: Building Your Personalized Rough Skin Prevention Plan
The transformation from rough, uncomfortable skin to soft, healthy barrier function requires understanding that dry skin represents a medical condition deserving appropriate attention rather than mere cosmetic inconvenience to tolerate indefinitely. Your skin’s barrier serves critical protective functions including preventing infection, regulating temperature, maintaining hydration, and sensing environmental stimuli—functions compromised when roughness and dryness indicate barrier breakdown. Understanding the comprehensive approach to facial hygiene and skin protection helps prevent the cycle of excessive cleansing that worsens dry skin conditions. The CDC emphasizes proper facial cleanliness techniques that balance hygiene needs with skin barrier protection, particularly important for preventing respiratory illness transmission without creating the harsh over-washing that strips protective oils and natural moisturizing factors from vulnerable skin surfaces. Treating dry skin effectively means addressing root causes through gentle cleansing that preserves natural protection, strategic moisturizing that repairs barrier structure and prevents water loss, environmental modifications that reduce external stressors, and when necessary, professional medical intervention for conditions beyond home treatment capacity. The multi-factorial nature of dry skin requires comprehensive approach rather than expecting single-product miracles, but the good news is that relatively simple, consistent efforts produce dramatic improvement for most people within four to six weeks, with ongoing maintenance preventing recurrence rather than requiring perpetual crisis management.
Building your personalized prevention plan begins with honest assessment of your current situation, identifying which factors contribute most significantly to your rough skin. Environmental contributors like winter heating, low humidity climates, or occupational water exposure require environmental modifications like humidification, protective gloves, or adjusted work practices beyond just topical treatment. Lifestyle factors including excessive bathing, harsh soaps, or inadequate moisturizing need behavioral changes that may feel inconvenient initially but become habitual with practice. Underlying medical conditions like eczema, thyroid disorders, or diabetes demand professional diagnosis and appropriate medical management alongside supportive skincare. Genetic predisposition suggesting inherent vulnerability to dry skin means accepting need for more proactive, consistent prevention rather than hoping minimal effort will suffice as it might for genetically fortunate individuals with robust barrier function regardless of care quality.
The action plan for the next thirty days creates foundation for lasting improvement, focusing on establishing core habits rather than overwhelming yourself with extensive routines. Week one centers on cleanser modification—switch to pH-balanced, fragrance-free creamy cleanser for face and body, reduce bathing frequency to every other day when feasible, lower water temperature to lukewarm, and limit shower duration to five to seven minutes maximum. Week two adds proper moisturizing technique—apply moisturizer to damp skin within three minutes of bathing, use adequate quantity creating visible layer initially, reapply to hands after each washing, and introduce richer night cream for evening. Week three incorporates environmental improvements—set up bedroom humidifier running nightly, reduce thermostat slightly to decrease heating-related dryness, switch to fragrance-free laundry detergent, and add cotton gloves or socks for overnight occlusive treatments on severely dry areas. Week four involves targeted treatments for problem areas—introduce gentle lactic acid exfoliant twice weekly, apply specialized products like urea cream to rough patches, schedule dermatology appointment if improvement remains insufficient, and reassess routine effectiveness making adjustments before settling into maintenance phase.
Long-term maintenance requires lower ongoing effort than initial correction but demands consistency to prevent recurrence rather than cycling through repeated crisis-and-recovery patterns. Continue gentle cleansing practices indefinitely even after skin improves, since reverting to harsh soaps quickly recreates problems. Maintain twice-daily moisturizing as baseline with flexibility to increase frequency during winter, travel, or stressful periods when skin becomes more vulnerable. Keep environmental modifications like humidification during heating season as routine part of winter preparation alongside furnace servicing and storm window installation. Schedule annual dermatology check-ups even when skin feels good, allowing early identification of subtle changes before they progress to uncomfortable roughness. Recognize that aging naturally reduces sebum production and barrier function, requiring gradual intensification of routine over decades—products adequate at age thirty may prove insufficient at fifty, necessitating adjustment rather than assuming something has gone wrong when formerly effective routine no longer controls symptoms.
Common pitfalls to avoid include expecting instant results from lifestyle changes that require weeks to show full benefits, product-hopping when improvements don’t appear within days leading to never giving appropriate treatments adequate trial period, assuming expensive products work better than affordable options without evaluating actual ingredients and formulations, neglecting consistency in favor of intensive occasional efforts that provide temporary improvement but fail to address underlying causes, and perhaps most importantly, accepting uncomfortable roughness as normal aging rather than recognizing it as treatable condition deserving intervention. Success requires patience with gradual improvement trajectory, discipline maintaining routine even when results aren’t immediately apparent, informed product selection based on ingredients rather than marketing, and appropriate help-seeking when home management proves insufficient rather than suffering indefinitely with severe symptoms treatable through professional care.
The psychological component of chronic rough skin deserves acknowledgment, as visible or uncomfortable skin conditions impact quality of life beyond physical symptoms. Social anxiety about handshakes revealing rough, cracked hands, self-consciousness about flaking visible on dark clothing, frustration with makeup application highlighting rather than concealing dry patches, and sleep disruption from intense itching all contribute to emotional burden that exacerbates stress which further worsens skin through mechanisms discussed earlier. Recognizing these psychological impacts as legitimate rather than dismissing them as vanity helps you prioritize effective treatment and justify investing time and resources into comprehensive management. Navigating modern beauty information requires critical evaluation of sources since social media creates unrealistic expectations through digital manipulation. Examining how influencer beauty lies through filters create impossible standards helps people develop realistic expectations for their own skin, understanding that even dermatologists don’t achieve the airbrushed perfection promoted online and that healthy skin shows normal texture, pores, and individual characteristics rather than Instagram-filter smoothness. Conversely, avoiding perfectionist expectations that your skin must achieve Instagram-filter smoothness prevents unnecessary distress over minor imperfections that don’t indicate actual barrier dysfunction—healthy skin shows pores, slight texture variation, and individual characteristics differing from airbrushed marketing images without these representing problems requiring correction.
Moving forward with confidence requires accepting that some trial and error proves necessary when finding optimal products and routines for your individual needs, as skin varies substantially between people in ways that prevent universal one-size-fits-all recommendations. What works brilliantly for your friend with dry skin may fail for you due to differences in barrier composition, sensitivity, underlying conditions, or environmental exposure. Be willing to test different cleansers, moisturizers, and techniques systematically—changing one variable at a time and allowing adequate trial period—until you identify your personal effective combination. Keep notes tracking what you try, how your skin responds, and which modifications help or hurt, creating personal reference eliminating repeated failed experiments. Join supportive communities whether online forums or local eczema associations where people share practical tips learned through experience, but maintain critical thinking about advice since individual variation means not every suggestion will suit your situation. Most importantly, recognize that investing attention in your largest organ’s health represents sensible self-care rather than self-indulgent vanity, as healthy skin barrier function protects against infection, enhances comfort, and supports overall wellbeing deserving the same priority as dental care, nutrition, or exercise in your health maintenance routine.
Frequently Asked Questions
Question 1: What causes rough, dry skin on the face and body?
Answer 1: Rough, dry skin develops through multiple interconnected factors creating cumulative assault on your skin’s moisture barrier that eventually overwhelms its natural protective and repair mechanisms. Environmental conditions represent primary external contributors, with low humidity environments pulling moisture from skin’s surface through osmotic pressure, cold weather constricting blood vessels reducing nutrient delivery to skin cells while harsh wind physically abrading protective lipid layers, and indoor heating systems dramatically lowering relative humidity to desert-like levels often below twenty percent. Lifestyle factors significantly impact barrier integrity through excessive bathing with hot water that dissolves protective sebum faster than lukewarm alternatives, harsh alkaline soaps disrupting pH balance and stripping natural moisturizing factors, insufficient moisturizer application that fails to replace lost hydration, and occupational exposures for healthcare workers, food handlers, and others requiring frequent handwashing. Underlying medical conditions including hypothyroidism slowing cellular metabolism and sebaceous gland activity, diabetes disrupting microcirculation and nerve function affecting sweat production, atopic dermatitis involving genetic barrier defects, kidney disease producing uremic changes, and various autoimmune conditions can manifest as persistent dry skin before other symptoms become apparent. Aging inevitably reduces sebaceous gland output approximately twenty-three percent per decade after age twenty while slowing cellular turnover and decreasing natural moisturizing factor production. Medications including diuretics, retinoids, statins, and chemotherapy drugs can create dry skin as recognized side effects. Nutritional deficiencies in essential fatty acids, vitamins A and C, or zinc compromise barrier function though rarely occur except in restrictive diets or malabsorption disorders. Genetic predisposition determines baseline vulnerability, with variations in filaggrin genes affecting natural moisturizing factor production and barrier integrity creating inherent susceptibility that requires more proactive prevention than individuals with robust genetic barrier function naturally enjoy.
Question 2: How often should I moisturize to prevent rough skin?
Answer 2: Optimal moisturizing frequency depends on individual skin needs, environmental conditions, and lifestyle factors, making personalized approach more effective than rigid universal schedules that may under-treat some people while proving excessive for others. At absolute minimum, moisturize twice daily immediately after bathing while skin remains damp to trap temporarily elevated water content before evaporation occurs, and again before bedtime to support overnight repair periods when cellular turnover peaks and transepidermal water loss naturally increases. However, rough skin often demands additional midday applications particularly for hands subjected to frequent washing that strips applied moisturizers within hours, exposed areas like face affected by outdoor weather exposure, and any regions feeling tight or uncomfortable regardless of recent moisturizing. Environmental factors modify frequency requirements, with winter heating season, low-humidity climates, and air-conditioned office environments necessitating more frequent reapplication than moderate outdoor humidity allows, sometimes requiring application four to six times daily during particularly challenging conditions. Occupational needs vary tremendously, with healthcare workers washing hands twenty to forty times per shift requiring moisturizer reapplication after each washing to prevent cumulative barrier damage, while desk workers in climate-controlled offices may achieve adequate hydration with standard twice-daily routine. Activity level influences requirements since exercise-induced sweating, swimming in chlorinated pools, and outdoor sports exposure all demand post-activity moisturizing beyond baseline routine. Listen to your skin’s signals rather than adhering rigidly to predetermined schedules—tightness sensation, visible flaking, discomfort, or roughness indicate immediate need for moisturizer regardless of how recently you last applied product, while skin feeling comfortable and supple suggests current routine provides adequate frequency for your situation. Unlike some skincare actives where excessive use causes problems, moisturizers rarely create issues from overuse assuming appropriate non-comedogenic formulations for your skin type, making the principle “moisturize whenever your skin feels dry or uncomfortable” safer guidance than restricting application out of concern for using too much product.
Question 3: What’s the difference between dry skin and dehydrated skin?
Answer 3: Dry skin represents a chronic skin type characterized by insufficient oil production from sebaceous glands resulting from genetic factors, aging, hormonal changes, or underlying medical conditions, creating persistent inability to maintain adequate lipid barrier that prevents water loss regardless of external hydration efforts. People with dry skin type produce inadequate sebum from birth or develop progressive reduction through aging, experiencing rough texture, visible flaking, tendency toward fine lines earlier than normal, sensitivity to harsh products, and discomfort from tightness that persists year-round though potentially worsening during winter months. Treatment requires oil-based products with emollients like ceramides and squalane that replenish missing lipids, occlusives like petrolatum creating physical barrier against moisture loss, and lifelong commitment to gentle cleansing avoiding sebum-stripping practices since the underlying sebaceous gland insufficiency cannot be cured only managed through supportive care. Dehydrated skin represents temporary condition affecting water content in stratum corneum rather than oil production, potentially occurring in any skin type including naturally oily complexions, triggered by environmental factors like low humidity, excessive exfoliation removing natural moisturizing factors, inadequate water intake, diuretic medications, or acute illness causing fluid loss. Dehydrated skin feels tight and rough despite normal or even excessive oil production, shows fine dehydration lines differing from deep wrinkles of dry skin, may appear dull or ashen, produces both flaking and oily patches simultaneously creating confusing combination presentation, and typically resolves within days to weeks once triggering factors are addressed and adequate hydration restored. Treatment focuses on water-based humectants like hyaluronic acid that attract and bind moisture molecules, barrier repair to prevent transepidermal water loss, environmental humidity optimization, and addressing underlying causes like medication side effects or illness rather than necessarily requiring oil-rich products that dry skin types need. Distinguishing between these conditions matters because using heavy oil-based products appropriate for dry skin can worsen dehydrated oily skin by clogging pores and causing breakouts, while water-based treatments for dehydration provide insufficient lipid replenishment for true dry skin type, making accurate diagnosis essential for effective treatment selection rather than trial-and-error product testing that may accidentally worsen your condition through inappropriate intervention.
Question 4: Can drinking more water help with rough, dry skin?
Answer 4: The relationship between water consumption and skin hydration proves more complex and less direct than popular belief suggests, with oral hydration supporting but not substituting for proper topical skincare in preventing or treating rough skin. Your body tightly regulates water distribution, prioritizing vital organs including brain, heart, kidneys, and liver for hydration delivery before directing resources to non-essential functions, meaning skin receives water only after critical needs are met regardless of how much you drink beyond replacing actual fluid losses. This physiological hierarchy explains why people can consume eight or more glasses daily yet still suffer chronically dry skin—the water they’re drinking supports overall cellular function and waste elimination but doesn’t preferentially route to skin surface where roughness and dryness manifest. Additionally, stratum corneum hydration depends more on the lipid barrier’s ability to prevent transepidermal water loss than on water delivery from dermal layers, meaning a compromised barrier will allow moisture to evaporate regardless of adequate internal hydration levels. Clinical studies examining water consumption effects on skin properties show modest improvements in some hydration markers when previously dehydrated individuals increase intake, but dramatic skin transformation rarely occurs from water drinking alone without concurrent topical barrier protection and moisturizing. However, chronic dehydration absolutely worsens dry skin by reducing overall body water content including skin tissue, impairing cellular function that maintains barrier integrity, potentially decreasing natural moisturizing factor production, and creating systemic stress that diverts resources from non-critical functions like skin maintenance toward survival priorities. Optimal approach combines adequate oral hydration meeting your individual fluid needs based on activity level, climate, and health status—generally eight eight-ounce glasses daily for average adults though requirements vary—with proper topical skincare including gentle cleansing, consistent moisturizing, and environmental protection that directly addresses surface barrier function where rough skin problems actually occur. Think of internal hydration as necessary foundation supporting overall health including skin, while topical care provides specific targeted intervention for surface problems that internal measures alone cannot adequately address.
Question 5: Should I exfoliate rough, dry skin or avoid it?
Answer 5: Exfoliation for rough, dry skin requires nuanced approach distinguishing between appropriate gentle techniques that improve moisturizer penetration by removing dead cell accumulation versus harsh mechanical scrubbing that damages already-compromised barriers worsening rather than resolving roughness problems. Dead skin cells normally shed invisibly through enzymatic processes called desquamation, but dry skin accumulates excessive corneocytes that lose intercellular cohesion yet fail to detach properly, creating visible flakes and rough texture while simultaneously creating physical barrier preventing moisturizers from penetrating to living cells where hydration matters most. Gentle chemical exfoliation using alpha-hydroxy acids including lactic acid at five to ten percent concentration or glycolic acid at five to eight percent concentration works enzymatically to dissolve intercellular cement holding dead cells together, allowing removal without mechanical friction that can damage delicate compromised skin. These chemical exfoliants also function as humectants attracting moisture while improving subsequent product absorption, providing dual benefit for dry skin when used appropriately. Introduce chemical exfoliants gradually starting with once or twice weekly application, always followed immediately by rich moisturizer since exfoliation temporarily increases transepidermal water loss creating vulnerability window before barrier rebuilds. Physical exfoliation through scrubs containing granules, brushes, or rough cloths should be avoided or used extremely cautiously with rough dry skin since mechanical friction creates micro-tears and inflammation in already-damaged barriers, potentially worsening problems despite intuitive appeal of manually removing flakes. If physical exfoliation feels psychologically necessary, limit to once weekly maximum using extremely gentle pressure with fine-grain scrubs or soft washcloths, never daily or with aggressive rubbing that dermatologists consistently identify as common cause of chronic irritation and barrier damage. Severely cracked or inflamed dry skin should avoid all exfoliation temporarily until barrier repair through intensive moisturizing restores integrity sufficiently to tolerate gentle chemical exfoliants, as attempting to exfoliate actively damaged skin risks infection and delayed healing. The exfoliation timing matters significantly—always exfoliate in evening rather than morning to allow overnight recovery before environmental exposure, and always on days when you can apply extra moisturizer afterwards since exfoliation increases immediate hydration needs that inadequate follow-up moisturizing fails to address leaving skin worse than before treatment.
Question 6: What ingredients should I look for in moisturizers for rough skin?
Answer 6: Effective moisturizers for rough skin combine three essential ingredient categories working through complementary mechanisms to attract water, repair barrier structure, and prevent moisture loss rather than relying on single-action formulations. Humectants including hyaluronic acid capable of binding up to one thousand times its weight in water molecules, glycerin providing both humectant and mild antimicrobial properties, urea combining hydration with gentle keratolytic action softening rough patches, panthenol converting to vitamin B5 for anti-inflammatory benefits, and sodium PCA naturally occurring in skin’s natural moisturizing factors attract and bind water from environment or deeper skin layers to stratum corneum. Consumer product testing by major media organizations provides valuable real-world performance data on moisturizer effectiveness beyond manufacturer claims. NBC News Select’s evaluation of the best moisturizers for dry skin involved dermatologist consultations and extensive product testing across multiple formulations, identifying which combinations of humectants, emollients, and occlusives deliver measurable hydration improvements for different dry skin severities. These ingredients work brilliantly in humid environments where atmospheric moisture provides abundant water source but can paradoxically worsen dryness in very low humidity by pulling water from deeper skin layers without external moisture to replace what evaporates. Emollients including ceramides one through nine matching ratios found in healthy skin barriers to repair lipid structure, cholesterol supporting ceramide organization in intercellular spaces, free fatty acids like linoleic and oleic acid replenishing barrier components, squalane mimicking skin’s natural sebum without oxidation concerns, and niacinamide strengthening barrier while reducing inflammation smooth rough texture by filling spaces between corneocytes while directly replenishing depleted lipid components creating barrier dysfunction. Occlusives including petrolatum preventing approximately ninety-eight percent of transepidermal water loss when properly applied, dimethicone creating breathable silicone barrier comfortable for facial use, lanolin from sheep’s wool offering intensive protection though potential allergen for sensitive individuals, shea butter combining occlusive properties with vitamin E antioxidant benefits, and mineral oil providing non-comedogenic occlusion create physical barriers over skin surface preventing moisture evaporation from successfully attracted and held water. Additional beneficial ingredients worth seeking include allantoin soothing irritation while promoting cell regeneration, colloidal oatmeal calming inflammation and itching particularly valuable when roughness triggers scratching, alpha-hydroxy acids at low concentrations providing gentle exfoliation improving subsequent product penetration, and antioxidants like vitamin E protecting against environmental oxidative damage that disrupts barrier function. Conversely, avoid ingredients commonly appearing even in products marketed for dry skin that create irritation or barrier disruption including alcohol denat or denatured alcohol causing immediate drying, artificial fragrances representing most common contact allergen triggering eczematous reactions, essential oils despite “natural” marketing can sensitize skin creating ongoing problems, harsh sulfates like sodium lauryl sulfate stripping oils, and certain preservatives including formaldehyde-releasers causing allergic reactions in susceptible individuals.
Board-certified dermatologists provide specialized expertise in identifying which moisturizing ingredients work synergistically for optimal barrier repair. The American Academy of Dermatology’s dermatologists’ tips for dry skin relief outline evidence-based protocols including specific humectant-emollient-occlusive combinations that address multiple hydration mechanisms simultaneously rather than relying on single-action products that provide incomplete barrier support.
Question 7: How long does it take to see improvement in rough skin with proper moisturizing?
Answer 7: Timeline for visible improvement in rough skin varies significantly based on severity, underlying causes, treatment consistency, and individual healing capacity, requiring realistic expectations that prevent premature abandonment of effective routines before benefits fully manifest. Mild dry skin limited to small areas or seasonal occurrence typically shows initial improvement within three to seven days of proper moisturizing twice daily, with rough patches feeling softer, flakiness diminishing noticeably, and discomfort reducing substantially though complete resolution may require two to three weeks of consistent routine adherence before skin achieves optimal texture and comfort. Moderate dry skin affecting larger body areas with visible scaling and persistent discomfort generally requires two to four weeks before dramatic improvement becomes apparent, though subtle changes like reduced tightness and improved makeup application may appear within first week encouraging continuation through the longer timeline needed for substantial barrier repair. Severe dry skin involving painful cracking, widespread roughness, or diagnosed conditions like eczema or severe xerosis typically needs four to six weeks minimum before major transformation occurs, with initial treatment potentially producing minimal visible change during first two weeks while cellular-level repairs establish foundation for eventual surface improvement. Chronic lifelong dry skin from genetic factors, aging, or underlying medical conditions may require eight to twelve weeks reaching optimal improvement under new skincare routine, accepting that complete permanent resolution may not occur since underlying predisposition persists requiring ongoing management rather than one-time cure. Understanding these timelines prevents common mistake of product-hopping after one week when improvements don’t appear immediately, never giving appropriate treatments adequate trial period to demonstrate effectiveness—dermatologists typically recommend four-week minimum evaluation before concluding a routine isn’t working, assuming no active worsening or irritation occurs warranting earlier discontinuation. Factors accelerating improvement include addressing environmental contributors through humidification, avoiding hot water and harsh soaps that continuously damage even as you attempt repair, increasing moisturizing frequency beyond twice-daily minimum for severely affected areas, and treating any underlying medical conditions contributing to barrier dysfunction. Conversely, factors delaying improvement include inadequate product quantity using cosmetically elegant thin films insufficient for actual hydration needs, inappropriate product selection like using lightweight gel formulations for severe dryness requiring rich ointments, inconsistent application skipping days or using irregular timing that prevents cumulative repair, ongoing irritant exposure from occupation or lifestyle habits sabotaging topical treatment efforts, and undiagnosed medical conditions requiring specific therapy beyond generic moisturizing.
Question 8: Is hot water bad for dry, rough skin?
Answer 8: Hot water represents one of the most common yet frequently overlooked behavioral factors systematically damaging skin barriers and directly contributing to development and persistence of rough dry skin despite people’s intuitive attraction to hot showers feeling temporarily soothing on uncomfortable skin. The mechanism involves temperature-dependent effects on sebum and lipid barrier components, with hot water above approximately one hundred five degrees Fahrenheit liquefying and dissolving natural skin oils far more effectively than lukewarm water below ninety-five degrees, essentially degreasing your skin through the same chemical principles making hot water superior for washing greasy dishes but problematic for preserving protective lipid layers. Each hot shower or bath removes progressively more sebum and intercellular lipids than would be lost during equivalent-duration lukewarm bathing, creating cumulative damage that manifests as increasingly rough texture over weeks and months even if individual washing sessions don’t produce immediately noticeable drying. Additionally, hot water increases blood flow to skin surface creating temporary flushing and warmth that some people find pleasant, but this vasodilation can exacerbate inflammation in conditions like rosacea or eczema where vascular reactivity contributes to symptoms. Temperature also affects how thoroughly water penetrates stratum corneum, with hotter water achieving greater initial hydration that feels pleasant during bathing but creates more dramatic subsequent evaporative loss as that absorbed water carrying natural moisturizing factors evaporates over the thirty to sixty minutes post-bathing—essentially creating greater swing from temporary super-hydration to excessive dryness compared to moderate lukewarm washing producing less dramatic but more stable moisture levels. Scalding water additionally risks direct thermal damage to skin cells particularly problematic for individuals with reduced temperature sensation from diabetes or neurological conditions who may not realize they’re using dangerously hot water until burns occur. Optimal water temperature for rough dry skin hovers around eighty-five to ninety-five degrees Fahrenheit—noticeably warm but distinctly cooler than typical shower preferences, feeling comfortable without the steamy heat many people psychologically associate with thorough cleaning. Transitioning from habitual hot showers to lukewarm bathing often requires gradual adjustment over several weeks, reducing temperature incrementally by five degrees every few days rather than abrupt change from one hundred ten degrees to eighty-five degrees that feels uncomfortably cold creating poor compliance and routine abandonment. Establishing consistent skincare habits requires structured approach accessible even for those new to beauty routines. Understanding the complete skincare routine for beginners provides essential foundation covering proper cleansing sequences, moisturizer application timing, product layering order, and realistic expectations for visible improvement timelines that prevent premature routine abandonment when transformation doesn’t occur overnight. Additional protective measures beyond temperature reduction include limiting total bathing duration to five to seven minutes maximum regardless of temperature, closing bathroom door during showering to maintain humidity that helps skin retain moisture, and most critically applying moisturizer to skin while still damp within three to five minutes after bathing to trap temporarily elevated water content before evaporation reverses any hydration benefit and leaves skin drier than before washing.
Question 9: Can diet affect rough, dry skin?
Answer 9: Nutritional factors influence skin barrier function and moisture retention capacity through multiple mechanisms involving cell membrane integrity, lipid synthesis, antioxidant protection, and inflammatory modulation, though dietary changes alone rarely resolve established rough skin without concurrent appropriate topical skincare providing direct barrier support and protection. Essential fatty acids particularly omega-3s from fatty fish, walnuts, flaxseeds, and chia seeds provide structural components for cell membranes throughout body including skin cells, with inadequate intake potentially compromising membrane function and barrier lipid production though frank deficiency severe enough to cause clinical symptoms remains rare except in extremely restricted very-low-fat diets below fifteen percent of calories from fat or conditions causing fat malabsorption. Gamma-linolenic acid from evening primrose oil and borage oil shows modest benefit in some atopic dermatitis studies including improvement in dryness symptoms, though results remain inconsistent and individual response varies considerably making dietary supplements potential adjunct rather than primary treatment. Vitamins contributing to skin health include vitamin A regulating sebum production and keratinization with deficiency producing characteristic follicular hyperkeratosis rough bumpy texture particularly on arms and thighs, vitamin C essential for collagen synthesis supporting structural integrity, vitamin D modulating immune function and barrier repair though evidence for supplementation improving dry skin in non-deficient individuals remains limited, and vitamin E providing antioxidant protection against oxidative damage though most people consume adequate amounts through normal diet. Zinc supports wound healing, immune function, and cell division processes important for barrier maintenance, with deficiency producing various skin manifestations including dryness though true zinc deficiency primarily occurs with malabsorption disorders rather than simple dietary insufficiency. Adequate hydration through water and other beverages supports overall cellular function including skin cells, with chronic dehydration potentially worsening dry skin though excessive water consumption beyond replacing actual losses provides no additional skin benefit as discussed previously. However, several important caveats limit relying on dietary approaches alone for rough skin treatment. First, nutritional improvements require weeks to months showing skin effects since cellular turnover and barrier repair occur gradually rather than immediately, making dietary modifications best viewed as long-term preventive strategy rather than acute symptom relief. Second, topical moisture loss represents primary mechanism for dry rough skin meaning even optimal internal nutrition cannot overcome inadequate external barrier protection and moisturizing—you cannot “eat your way” to soft skin while continuing harsh cleansing and neglecting moisturizer application. Third, modern varied diets in developed countries rarely produce severe nutritional deficiencies causing obvious skin symptoms except in restrictive eating disorders, extreme elimination diets, or specific medical conditions, meaning most rough skin stems from external factors rather than nutritional lack. Optimal approach combines balanced nutrient-dense diet supporting overall health including skin alongside proper topical skincare directly addressing surface problems, viewing nutrition as foundation rather than sole solution.
Question 10: When should I see a dermatologist for rough, dry skin?
Answer 10: Professional dermatologic evaluation becomes necessary when rough dry skin persists despite four weeks of consistent appropriate home treatment including gentle cleansing with pH-balanced products, twice-daily moisturizing using quality barrier-repair formulations applied to damp skin, environmental modifications like humidity control, and lifestyle adjustments avoiding excessive bathing and harsh soaps. Four-week timeline allows adequate trial period for over-the-counter interventions to demonstrate effectiveness while preventing unnecessary delay for conditions requiring prescription treatment, though more urgent consultation is warranted if specific concerning features appear before completing full self-treatment trial. Painful deep cracking creating open fissures that bleed represents urgent concern requiring professional attention to prevent secondary bacterial infections like cellulitis that can develop when pathogens enter through compromised barriers, assess for underlying conditions like severe eczema or diabetes requiring specific management, and potentially provide prescription-strength barrier repair products or therapeutic procedures accelerating healing beyond over-the-counter capabilities. Severe itching disrupting sleep or daily activities despite consistent moisturizing and over-the-counter anti-itch treatments suggests inflammatory conditions like atopic dermatitis, contact dermatitis from allergen exposure, or systemic conditions producing uremic pruritus that require professional diagnosis and prescription anti-inflammatory treatments unavailable without medical supervision. Widespread dry skin suddenly appearing without obvious environmental trigger or affecting entire body surface could indicate underlying medical conditions including hypothyroidism, diabetes, kidney disease, liver disorders, or lymphoma that manifest skin changes before other symptoms become apparent, warranting systemic evaluation beyond purely dermatologic assessment. Localized rough skin affecting specific body areas like hands while rest of skin appears normal despite similar treatment might indicate occupational dermatitis from workplace exposures, allergic contact dermatitis requiring identification and avoidance of specific allergen through patch testing, or localized conditions like palmoplantar psoriasis needing targeted therapy. Signs of infection including increasing redness spreading beyond original dry patches, warmth, swelling, oozing of clear fluid or pus, crusting, or fever require prompt medical evaluation since skin barrier compromise creates vulnerability to bacterial or fungal invasion demanding antimicrobial treatment preventing serious complications. Children or elderly individuals with severe dry skin deserve lower threshold for professional consultation since these age groups have different barrier function compared to healthy young adults and may require specialized treatment approaches accounting for developmental or age-related factors. Additionally, anyone experiencing dry skin as new symptom after starting medications should discuss with prescribing physician whether drug represents contributing factor potentially requiring formulation change or dosage adjustment balancing therapeutic benefit against dermatologic side effects. When consulting dermatologist, prepare by noting onset timeline, treatments attempted with duration and response, family history of skin conditions, current medications and medical conditions, occupational exposures, and specific concerns prompting visit, helping physician efficiently assess situation and develop appropriate management plan.
Articles related:
Tags
📧 Get More Articles Like This
Subscribe to receive product reviews and buying guides in your inbox!
We respect your privacy. Unsubscribe at any time.