Treating Cold Feet Without Cost: How the Right Bath Temperature Improves Blood Flow

Table of Contents
- Introduction: The Universal Experience of Cold Feet
- Understanding the Science of Foot Temperature and Circulation
- The Optimal Water Temperature: What Research Reveals
- Duration and Technique: Maximizing Your Bath Benefits
- Who Can Benefit Most from Warm Foot Baths
- Special Considerations for Different Health Conditions
- Beyond the Bath: Complementary Strategies for Warm Feet
- Common Mistakes to Avoid
- Conclusion
- Frequently Asked Questions
Introduction: The Universal Experience of Cold Feet
The bedroom felt comfortably warm that December evening when Sarah climbed into bed, yet her feet remained stubbornly icy despite wearing thick socks. This nightly battle had persisted for months, disrupting her sleep and leaving her frustrated. Her doctor had ruled out serious conditions but offered little beyond expensive prescription creams and compression garments. Then a chance conversation with her grandmother revealed a simple solution that had helped generations before medications dominated healthcare: the therapeutic power of properly温度された warm water baths. What Sarah discovered transformed not just her cold feet but her entire understanding of how simple, cost-free interventions can address persistent health challenges that modern medicine sometimes overlooks in its rush toward pharmaceutical solutions.
Cold feet affect millions of people worldwide, transcending age, gender, and geographical boundaries. While some experience this merely as minor discomfort during winter months, others endure chronic coldness that significantly impacts quality of life. The feet, positioned furthest from the heart and bearing the body’s weight throughout each day, face unique challenges in maintaining adequate blood flow and warmth. Understanding why feet become cold and how to address this condition naturally requires examining the intricate relationship between temperature, blood vessels, and the circulatory system that sustains every cell in our bodies.
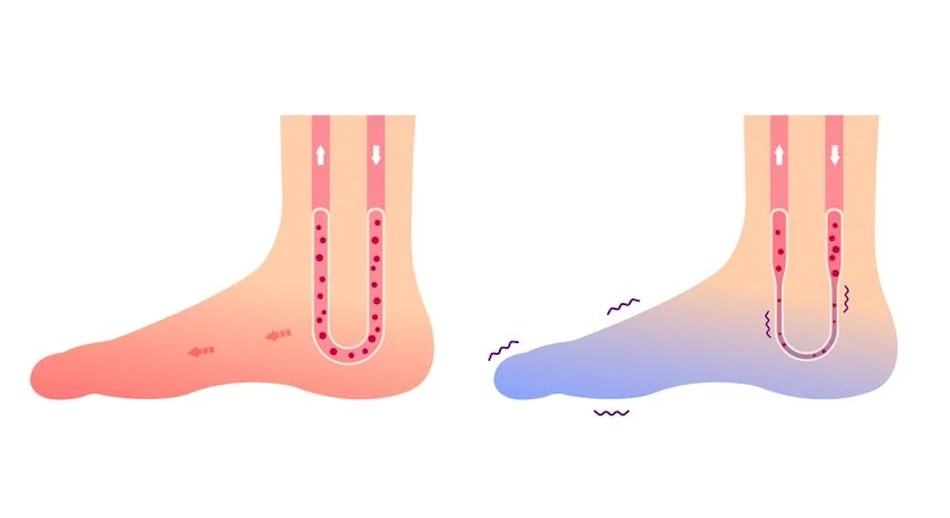
The human body maintains a core temperature around 37 degrees Celsius through remarkably complex thermoregulatory mechanisms. When environmental temperatures drop or the body perceives cold stress, the sympathetic nervous system triggers vasoconstriction in peripheral blood vessels. This protective response prioritizes vital organs by reducing blood flow to extremities, particularly hands and feet. While evolutionarily advantageous for survival in harsh climates, this same mechanism creates the uncomfortable sensation of persistently cold feet in modern life. The blood vessels in feet can constrict so severely that circulation decreases to merely ten percent of baseline levels, creating a cascading effect where reduced blood flow leads to lower tissue temperature, which further promotes vasoconstriction in a self-perpetuating cycle.
While this article discusses how bath temperature can improve foot warmth, we also offer a video explaining another method for warming feet using elements, vitamins, and movement exercises :
Beyond simple environmental cold, numerous factors contribute to chronically cold feet. Peripheral artery disease affects approximately 200 million people globally, causing narrowed arteries that restrict blood flow to limbs. Diabetes damages both nerves and blood vessels, creating a dangerous combination where reduced circulation meets diminished ability to sense temperature changes. Thyroid disorders disrupt metabolic processes that regulate body temperature. Certain medications, particularly beta-blockers used for heart conditions, intentionally reduce peripheral circulation as part of their therapeutic mechanism. Anemia reduces the blood’s oxygen-carrying capacity, affecting tissue warmth. Even lifestyle factors like smoking cause persistent vasoconstriction that leaves feet chronically cold regardless of external temperatures.
The economic burden of treating cold feet and related circulation issues reaches into billions annually when accounting for medical visits, prescription medications, specialized garments, and advanced interventions. Yet emerging research demonstrates that something as simple as properly温度された warm water baths can provide significant relief without financial cost. Recent studies from Japanese and Taiwanese research institutions have identified precise temperature ranges and durations that optimize circulation improvement. These findings challenge the assumption that effective treatments must be complex or expensive. The therapeutic mechanism operates through basic physiology: warm water causes peripheral vasodilation, increasing blood flow to feet and creating favorable temperature gradients that facilitate heat distribution throughout the body.
What makes this approach particularly compelling is its accessibility. Unlike medications requiring prescriptions and ongoing costs, or specialized equipment demanding significant investment, warm water baths require only a container, water, and a thermometer. The intervention respects both ancient wisdom and modern science, bridging traditional practices that cultures worldwide have employed for centuries with contemporary research validating their effectiveness. As healthcare systems globally struggle with rising costs and medication side effects, returning to fundamentally sound interventions offers promise for improving public health outcomes while reducing financial burdens on individuals and society.
This comprehensive exploration examines every aspect of using warm water baths to treat cold feet naturally. We will investigate the precise temperature ranges that research has identified as optimal, the duration required for maximum benefit, and the physiological mechanisms explaining why this simple intervention works so effectively. Special attention will be paid to safety considerations for people with different health conditions, from diabetes to heart disease. We will also examine complementary strategies that enhance bath effectiveness and address common mistakes that reduce benefits or create unnecessary risks. Throughout this journey, scientific evidence will illuminate practical applications, empowering readers to take control of their circulation health through informed, cost-free interventions.
Understanding the Science of Foot Temperature and Circulation
The circulatory system represents one of nature’s most elegant engineering solutions, transporting oxygen, nutrients, and warmth to every tissue while removing metabolic waste products. In the feet, this system faces unique challenges due to distance from the heart, gravitational effects, and exposure to varying environmental temperatures. Understanding how blood flow operates in the lower extremities provides essential context for why feet become cold and how warm water baths address this condition at the physiological level.
Blood begins its journey to the feet when the heart’s left ventricle contracts, propelling oxygen-rich blood into the aorta. This blood travels down through progressively smaller arteries until reaching the tiny arterioles and capillaries that permeate foot tissues. In healthy circulation, this journey takes only seconds, with each heartbeat pushing blood forward through approximately 100,000 kilometers of blood vessels throughout the body. The feet contain dense networks of these vessels, particularly in the toes where blood must reach the most distant tissues. Once oxygen and nutrients have been delivered, blood collects in venules and veins for the return journey to the heart, fighting against gravity in the upright human posture.
Temperature regulation in the feet depends heavily on blood flow volume and velocity. When circulation operates optimally, warm blood continuously replenishes heat that radiates from foot surfaces into the environment. The skin acts as the interface between internal warmth and external cold, with its temperature reflecting the balance between heat delivery through blood flow and heat loss to surroundings. Research has established that skin temperature in healthy feet at room temperature averages around 30-32 degrees Celsius, several degrees below core body temperature but warm enough to feel comfortable. This gradient allows efficient heat exchange while maintaining tissue viability.
The phenomenon of cold-induced vasoconstriction serves as the primary mechanism behind cold feet. Understanding peripheral vascular disease becomes essential when cold feet persist despite environmental warmth. Atherosclerotic plaque accumulation in leg arteries creates serious circulation impairments that require medical intervention to prevent tissue damage. When temperature sensors in the skin detect cold, they send signals through peripheral nerves to the hypothalamus, the brain’s thermoregulatory center. The hypothalamus responds by activating the sympathetic nervous system, which releases norepinephrine and other neurotransmitters that cause smooth muscle in blood vessel walls to contract. This vasoconstriction dramatically reduces vessel diameter, which according to Poiseuille’s law, decreases blood flow exponentially since flow rate varies with the fourth power of vessel radius. A fifty percent reduction in vessel diameter results in blood flow decreasing to approximately six percent of original levels.
This vasoconstriction prioritizes core body temperature maintenance over peripheral comfort. By reducing blood flow to extremities, the body minimizes heat loss through these high-surface-area regions while ensuring adequate perfusion to vital organs like the brain, heart, and kidneys. Understanding poor circulation symptoms helps individuals determine when cold feet represent a medical concern requiring professional evaluation rather than simply environmental sensitivity. Chronic coldness accompanied by pain, color changes, or numbness warrants vascular assessment. While beneficial in truly cold environments where hypothermia poses real danger, this response can become maladaptive in modern indoor settings where core temperature faces no actual threat but peripheral discomfort persists.
Beyond environmental cold, several pathological conditions disrupt normal foot circulation. Peripheral artery disease develops when atherosclerotic plaques build up inside arterial walls, narrowing the passages through which blood flows. These fatty deposits accumulate over years, typically affecting leg and foot arteries in people over fifty or younger individuals with risk factors like smoking, diabetes, or high cholesterol. As arteries narrow, less blood reaches foot tissues, causing not just coldness but also pain during walking, slow wound healing, and in severe cases, tissue death requiring amputation. Approximately one in twenty people over sixty has peripheral artery disease, though many remain undiagnosed because symptoms develop gradually.
Diabetes creates a particularly dangerous situation through multiple mechanisms. High blood sugar levels damage both large blood vessels, causing atherosclerosis, and small vessels, leading to microangiopathy. Simultaneously, diabetes causes peripheral neuropathy, damaging the nerves that sense temperature and pain. This combination proves deadly: reduced circulation impairs healing while nerve damage prevents patients from feeling injuries that might occur. The inability to sense appropriate water temperature creates burn risks during foot baths, requiring special precautions we will address in detail later. Understanding these diabetes-specific challenges explains why approximately sixty thousand diabetics require lower limb amputations annually in the United States alone.
Raynaud’s phenomenon represents another circulation disorder characterized by excessive vasoconstriction in response to cold or stress. During Raynaud’s attacks, blood flow to fingers and toes nearly ceases, causing affected areas to turn white, then blue, then red as circulation eventually returns. Primary Raynaud’s occurs without underlying disease, affecting mostly young women. Secondary Raynaud’s accompanies autoimmune conditions like lupus or scleroderma. While not typically dangerous, Raynaud’s causes significant discomfort and disrupts daily activities. Warm water baths provide particular relief for Raynaud’s patients by counteracting the excessive vasoconstriction that defines their condition.
The feet’s position at the body’s lowest point when standing or sitting introduces gravitational challenges to circulation. Blood returning from feet to the heart must work against gravity, relying on one-way valves in veins and muscle contractions in the legs to propel it upward. When people sit or stand motionless for extended periods, this return flow slows, causing blood to pool in leg and foot veins. This venous pooling reduces the pressure gradient driving blood through foot tissues, potentially contributing to coldness. Elevating feet above heart level reverses this gravitational challenge, facilitating venous return and improving overall foot circulation.
Research into foot circulation has revealed fascinating details about how blood flow varies throughout the day and in response to different stimuli. Studies using laser Doppler flowmetry, which measures blood velocity in skin capillaries, show that foot blood flow fluctuates significantly even at rest, varying by as much as threefold within minutes. These spontaneous variations reflect the complex interplay of neural, hormonal, and local metabolic factors regulating circulation. Understanding this natural variability helps explain why cold feet come and go unpredictably and why interventions must address underlying regulatory mechanisms rather than just providing momentary warmth.
The discovery of cold-induced vasodilation added an important nuance to our understanding of foot temperature regulation. Researchers observed that when hands or feet remain in cold water for extended periods, initial vasoconstriction gives way to periodic vasodilation, causing cyclical warming despite ongoing cold exposure. This hunting response, first described by Sir Thomas Lewis in 1930, appears to protect tissues from cold injury by periodically restoring blood flow before damage occurs. The mechanisms remain debated, but likely involve the inability of smooth muscle in vessel walls to maintain contraction indefinitely at very low temperatures. This phenomenon explains why some people adapt better to cold environments, maintaining warmer feet through more frequent or pronounced vasodilation cycles.
Nitric oxide has emerged as a crucial molecule in circulation regulation. This simple gas, produced by endothelial cells lining blood vessels, causes smooth muscle relaxation and vasodilation. When blood flow increases, the resulting shear stress on vessel walls stimulates nitric oxide production, creating a positive feedback loop where increased flow promotes further dilation. Conversely, conditions that reduce nitric oxide availability, including diabetes, hypertension, and smoking, impair this beneficial mechanism. Some research suggests that warm water exposure may enhance nitric oxide production, contributing to the circulation improvements observed during foot baths.
The lymphatic system, though often overlooked, plays a supporting role in foot health and temperature regulation. This parallel network of vessels collects excess fluid, proteins, and waste products from tissues, returning them to the bloodstream. In the feet, where gravitational effects promote fluid accumulation, efficient lymphatic drainage prevents swelling that could compress blood vessels and impair circulation. Some studies suggest that warm water immersion aids lymphatic drainage through mechanisms not fully understood but possibly related to improved tissue perfusion and reduced inflammation.
Modern imaging techniques have revolutionized our ability to study foot circulation in real-time. Infrared thermography creates visual maps of skin temperature distribution, revealing cold spots that might indicate circulation problems. Doppler ultrasound measures blood flow velocity through specific vessels, helping diagnose arterial blockages. Ankle-brachial index testing compares blood pressure in ankles versus arms, providing a simple screening tool for peripheral artery disease. These technologies have validated many traditional observations about foot circulation while revealing previously unknown details about how various interventions affect blood flow.
The autonomic nervous system’s role in circulation extends beyond simple vasoconstriction and vasodilation. This system maintains a baseline vascular tone that adjusts constantly based on multiple inputs including temperature sensors, baroreceptors monitoring blood pressure, chemoreceptors sensing oxygen and carbon dioxide levels, and higher brain centers processing emotional and cognitive information. Stress and anxiety activate sympathetic responses that constrict peripheral vessels, explaining why nervousness can cause cold hands and feet even in warm environments. Conversely, relaxation enhances parasympathetic activity, promoting vasodilation and warming. This mind-body connection means that warm foot baths may provide benefits beyond direct thermal effects, potentially reducing stress and anxiety that contribute to vasoconstriction.
Age-related changes in circulation help explain why cold feet become more common as people grow older. Blood vessels stiffen with age, losing some capacity for vasodilation. Endothelial function declines, reducing nitric oxide production. Atherosclerosis progresses even in people without diagnosed disease. Older adults also tend to have multiple conditions and take multiple medications that affect circulation. These cumulative changes don’t make cold feet inevitable in aging, but they do increase vulnerability and underscore the importance of maintaining circulation health through accessible interventions like warm water baths.
Understanding the science behind foot circulation and temperature regulation provides the foundation for appreciating why warm water baths work so effectively. By directly warming skin and underlying tissues, baths overcome vasoconstriction’s effects, forcing blood vessels to dilate regardless of sympathetic nervous system signals. This mechanical override bypasses the complex regulatory systems that might be malfunctioning in chronic cold feet, providing relief even when underlying conditions haven’t been fully addressed. The beauty of this approach lies in its directness: warm water delivers heat exactly where needed, triggering physiological responses that improve circulation both during and after the bath.
The Optimal Water Temperature: What Research Reveals
Determining the ideal water temperature for therapeutic foot baths represents more than academic curiosity. Too cold, and the bath fails to provide circulation benefits. Too hot, and risks of burns, cardiovascular stress, and skin damage emerge. Scientific research conducted over the past two decades has identified precise temperature ranges that maximize benefits while minimizing risks, though individual variation means some personalization remains necessary within these evidence-based guidelines.
Japanese researchers have led the field in studying optimal bathing temperatures, reflecting that culture’s deep tradition of therapeutic water use. A landmark 2022 study published in the Physical Therapy Research journal examined ten healthy male participants experiencing three different bathing conditions: half-body immersion, low-leg immersion, and foot-only immersion. Scientific research on foot bathing circulation has expanded significantly in recent years, providing evidence-based protocols that optimize therapeutic benefits. These studies validate traditional practices while establishing precise parameters for temperature, duration, and technique. Each session used water温度された at 42 degrees Celsius. The researchers measured peripheral blood flow using laser Doppler flowmetry on the earlobe, far from the heated area, to assess systemic circulation effects. Their findings revealed that foot baths at 42 degrees Celsius, with water reaching mid-calf level, provided optimal peripheral circulation improvement. Blood flow increased to 1.7 times baseline levels and maintained this elevation even after the bath ended, suggesting sustained benefits beyond the immediate warming effect.
Another significant study from Taiwan examined the effects of two water temperatures, 40 and 41 degrees Celsius, on elderly participants during hour-long foot baths. Research examining warm water therapy continues revealing new insights into how controlled temperature exposure influences vascular function. These findings help clinicians recommend evidence-based interventions for patients struggling with circulation-related symptoms. The researchers measured what they called the distal-proximal temperature gradient, calculated by subtracting abdominal temperature from foot temperature. Studies on peripheral blood flow measurement techniques have advanced our understanding of how localized warming affects systemic circulation. These methodologies provide objective evidence supporting therapeutic interventions previously based primarily on anecdotal reports. This gradient serves as an indirect measure of heat dissipation from body core to periphery. Both temperatures significantly increased the gradient within ten minutes and maintained it throughout the bath. Interestingly, no significant difference emerged between the two temperatures in terms of circulation benefits, suggesting that the 40-41 degree range provides a therapeutic sweet spot where slightly higher or lower temperatures within this range work similarly well.
Temperature recommendations must account for different populations and health conditions. For healthy adults without circulation problems, the research consensus points to 40-42 degrees Celsius as optimal. This range, equivalent to 104-108 degrees Fahrenheit, feels comfortably warm without being uncomfortably hot. Water at these temperatures triggers robust vasodilation without overtaxing cardiovascular systems or risking burns in people with normal temperature sensation. Starting at the lower end of this range and gradually increasing to personal tolerance ensures safety while maximizing comfort.
People with diabetes face special temperature considerations due to peripheral neuropathy that impairs temperature sensation. A diabetic person might not feel water that’s dangerously hot until burns have already occurred. Healthcare guidelines for diabetic foot care consistently recommend testing water temperature with a thermometer rather than relying on sensation. The recommended maximum temperature drops to 37-40 degrees Celsius for diabetics, providing therapeutic warmth while maintaining a greater safety margin. Some experts suggest diabetics use even lower temperatures around 35-37 degrees Celsius, sacrificing some circulation benefit for enhanced safety. The critical principle remains: always test water with a thermometer before immersing feet.
Pregnant women represent another population requiring modified temperature recommendations. Excessive heat exposure during pregnancy, particularly in the first trimester, has been associated with increased risk of neural tube defects and other developmental issues. While localized foot warming differs from whole-body heating in hot tubs or saunas, pregnant women should exercise caution. Water temperature should not exceed 38 degrees Celsius, and bath duration should be limited to 15 minutes maximum. As pregnancy progresses and circulation to the lower body increases naturally due to expanded blood volume, many women find they need less aggressive foot warming anyway.
Elderly individuals often have multiple factors affecting their temperature sensitivity and circulation. Many take medications like beta-blockers or diuretics that affect cardiovascular responses. Age-related changes in skin thickness and sweat gland function alter heat perception. Chronic conditions like heart disease or arthritis introduce additional considerations. For older adults, starting with lower temperatures around 38-40 degrees Celsius and monitoring closely for any signs of discomfort, dizziness, or excessive fatigue ensures safety. Having someone nearby during the first few baths provides an extra safety measure for elderly individuals who might experience orthostatic hypotension when standing after warming.
The concept of gradually increasing water temperature deserves special attention. Traditional hydrotherapy practices often begin with comfortable warm water, then slowly add hotter water over several minutes to reach the target temperature. This gradual approach allows the body’s cardiovascular system to adapt smoothly rather than experiencing sudden demands. Research supports this practice, showing that gradual温度據increases produce less cardiovascular stress while achieving similar circulation benefits compared to immediate hot water immersion. The practical application involves starting with water at 37-38 degrees Celsius, then adding small amounts of hotter water every few minutes until reaching the desired final temperature of 40-42 degrees for healthy adults.
Individual tolerance varies significantly based on factors that research hasn’t fully elucidated. Some people comfortably tolerate water at 43 degrees Celsius while others find 40 degrees uncomfortably hot. These differences likely reflect variations in nerve density, skin thickness, baseline circulation, and perhaps genetic factors affecting temperature perception. The key principle holds that personal comfort should guide temperature choice within the evidence-based range. If water feels uncomfortably hot, it probably is, regardless of what a thermometer reads. Conversely, water that feels merely warm rather than hot may not provide optimal circulation benefits.
Seasonal and environmental factors influence optimal bathing temperature. In winter, when ambient temperatures are low and feet tend to be colder initially, slightly warmer bath water may be needed to achieve the same circulation improvement compared to summer. Someone coming in from outdoors with freezing feet should exercise particular caution, starting with moderate warmth and gradually increasing temperature as feet warm up. Shocking extremely cold feet with very hot water risks injury and causes significant discomfort.
Water temperature stability throughout the bath presents a practical challenge. Without active heating, bath water cools steadily as it loses heat to the surrounding air and container. Studies using temperature-controlled foot bath equipment maintain constant温度, but most home users don’t have such devices. The solution involves periodically adding small amounts of hot water to maintain target temperature. However, this requires care: always remove feet from the water before adding hot water to prevent burns, test the temperature after mixing before re-immersing feet, and add hot water to the side opposite from where feet will return.
The relationship between water温度 and circulation improvement isn’t perfectly linear. Research shows that temperatures below 38 degrees Celsius provide minimal circulation benefits compared to baseline, presumably because they’re not warm enough to trigger robust vasodilation. Temperatures above 43 degrees Celsius increase burn risks substantially without proportional circulation improvements. The plateau effect suggests that once adequate vasodilation has been achieved, hotter water adds risk without additional benefit. This dose-response relationship supports using temperatures in the 40-42 degree range for maximum benefit-to-risk ratio.
Cultural practices around bathing temperatures offer interesting historical context. Japanese onsen typically maintain water at 40-42 degrees Celsius, precisely the range research has validated. Traditional Turkish hammams use varying temperatures in different rooms, allowing gradual adaptation. Scandinavian sauna practices alternate between intense heat and cold plunges, though this differs from sustained warm foot baths. These cultural traditions suggest that humans have intuitively discovered beneficial temperature ranges through centuries of experience, which modern science now confirms with precise measurements.
Home implementation of optimal温度據 requires minimal equipment: a reliable thermometer, preferably digital for easy reading, and containers large enough to comfortably hold both feet with water covering ankles and extending up the lower legs. Instant-read thermometers work well for checking water temperature before starting and periodically during the bath. Some people prefer continuous-reading thermometers that can remain in the water, though these aren’t necessary for safe bathing with periodic manual checks.
Shop on AliExpress via link: wholesale-digital-water-thermometer
Understanding temperature in different measurement systems prevents confusion. Most scientific research uses Celsius, where 40-42 degrees represents the optimal range. In Fahrenheit, this translates to 104-108 degrees. When reading international research or product specifications, always verify which temperature scale is being used to avoid dangerous mistakes. A temperature of 40 degrees Fahrenheit would be painfully cold, not therapeutic, illustrating why clarifying measurement units matters critically.
The optimal temperature discussion ultimately balances scientific evidence, individual circumstances, and practical safety considerations. While research has identified the 40-42 degree Celsius range as ideal for healthy adults, personalization within and slightly below this range accommodates individual tolerance, health conditions, and safety priorities. The consistent message across all studies remains that warm water at appropriate temperatures provides measurable circulation improvements, validating this simple intervention’s therapeutic potential when implemented thoughtfully.
Duration and Technique: Maximizing Your Bath Benefits
Knowing the right water temperature addresses only half the equation for effective therapeutic foot baths. How long you soak your feet and the specific techniques you employ during bathing significantly influence the circulation benefits you achieve. Recent research has provided increasingly precise guidance on optimal duration, water depth, frequency, and complementary practices that enhance effectiveness while maintaining safety.
The duration question has received substantial research attention, with findings converging on a remarkably consistent answer: twenty to twenty-four minutes provides optimal circulation benefits for most people. This specific timeframe emerged from multiple independent studies examining peripheral blood flow during and after foot baths of varying durations. A 2022 Japanese study found that twenty-minute foot baths at 42 degrees Celsius produced maximum sustained circulation improvement. Blood flow to peripheral regions including the earlobes, measured as an indicator of systemic circulation, increased progressively during the first twenty minutes, then plateaued, suggesting that longer durations added minimal additional benefit.
Taiwanese researchers examining hour-long foot baths discovered that while circulation improvements began within the first ten minutes, the benefits had largely plateaued by twenty-four minutes. Extending bathing beyond this point didn’t further enhance the distal-proximal temperature gradient that indicates improved heat distribution throughout the body. Additionally, prolonged immersion beyond twenty-five minutes started showing diminishing returns as cardiovascular stress accumulated without proportional circulation gains. These findings from different研究ers using different methodologies remarkably agree on the twenty to twenty-four minute sweet spot.
For people with heart conditions or limited cardiovascular reserves, shorter durations may be more appropriate initially. Starting with ten to fifteen minute sessions allows the cardiovascular system to adapt to the demands of increased peripheral blood flow without excessive stress. As tolerance builds over days to weeks, duration can gradually extend toward the twenty-minute target. Healthcare providers can offer personalized guidance based on specific cardiac conditions, with some patients requiring permanent limits on bathing duration to avoid overtaxing their hearts.
Water depth significantly influences both effectiveness and safety. Research comparing ankle-deep, mid-calf, and knee-high water levels found that mid-calf depth provided the best balance of circulation benefits and practical safety. Water reaching approximately ten to fifteen centimeters above the ankles, covering the lower calf, allows adequate thermal penetration to leg vessels while limiting cardiovascular demands compared to deeper immersion. Ankle-only bathing proved less effective, presumably because less tissue volume was warmed and fewer blood vessels experienced direct heating. Knee-high bathing didn’t significantly improve outcomes compared to mid-calf depth while requiring larger water volumes and bigger containers.
The position of feet during bathing influences comfort and circulation. Sitting in a comfortable chair with feet resting flat on the container bottom allows relaxation while maintaining natural foot position. Some people find that gently moving toes and ankles during bathing helps circulate warm water around all foot surfaces, though whether this enhances circulation benefits hasn’t been rigorously studied. What’s clear is that feet shouldn’t be cramped or uncomfortably positioned, as muscle tension could potentially impede circulation gains.
Frequency of foot baths balances achieving consistent benefits against practical considerations like time availability and skin health. Research examining daily foot baths over fifteen-day periods showed progressive improvements in baseline foot temperature, suggesting cumulative benefits from consistent practice. For chronic cold feet, daily bathing appears optimal, establishing a regular routine that maintains improved circulation. Those using foot baths primarily for relaxation or occasional cold feet might find three to four sessions weekly sufficient. The key lies in consistency rather than sporadic intensive use.
Timing of baths throughout the day can be optimized based on desired outcomes beyond circulation improvement. Evening baths performed one to two hours before bedtime leverage the body’s natural temperature regulation during sleep. As core body temperature drops in preparation for sleep, the heat load from a warm foot bath enhances the distal-to-proximal temperature gradient associated with faster sleep onset and better sleep quality. Multiple studies have demonstrated that pre-bedtime foot baths shorten the time required to fall asleep, even in people without diagnosed sleep disorders. This dual benefit of improved circulation and enhanced sleep makes evening timing particularly attractive for many users.
Morning foot baths provide different advantages, offering an energizing start to the day by stimulating circulation and potentially reducing morning stiffness in feet and ankles. People with Raynaud’s phenomenon who experience severe vasoconstriction upon waking might find morning baths particularly helpful for starting the day with warmer, more comfortable feet. The timing choice ultimately depends on individual schedules, preferences, and specific symptoms being addressed.
Preparation before bathing enhances both safety and effectiveness. Gathering all necessary supplies, including a thermometer, towels, and any additions like Epsom salts, before starting prevents having to interrupt the bath midway. Testing water temperature thoroughly before immersing feet prevents burns and ensures therapeutic warmth. Having a clock or timer visible helps monitor duration without repeatedly checking time. Setting up in a comfortable location where you can relax for twenty minutes without interruption maximizes the stress-reduction benefits that complement circulation improvements.
The post-bath routine deserves equal attention to the bath itself. How you transition from warm water back to room temperature influences both comfort and sustained circulation benefits. Abruptly standing after twenty minutes of warming can cause orthostatic hypotension, where blood pressure drops suddenly upon standing, potentially causing dizziness or fainting. To prevent this, transition gradually: first remove feet from water and let them cool slightly while remaining seated, then slowly stand while holding a stable surface, then walk slowly for the first few steps until circulation stabilizes.
Drying feet thoroughly, especially between toes, prevents fungal infections that thrive in warm, moist environments. Use gentle patting motions rather than vigorous rubbing, which could irritate skin that has softened during bathing. Pay particular attention to the spaces between toes where moisture accumulates. For people with diabetes or compromised immune systems, inspecting feet after each bath allows early detection of any cuts, blisters, or areas of irritation that might have gone unnoticed due to neuropathy.
Moisturizing immediately after bathing, while skin retains warmth and moisture, helps prevent excessive drying that prolonged water exposure can cause. Choose moisturizers appropriate for foot skin, which tends to be thicker than facial skin. Avoid applying moisturizer between toes, where it could create overly moist conditions favoring fungal growth. Urea-based lotions work particularly well for feet, providing deep hydration that standard lotions may not achieve. For people concerned about slipping, apply moisturizer then wear non-slip socks to protect floors while skin absorbs the lotion.
Covering feet with warm socks immediately after bathing helps retain heat longer, extending the circulation benefits beyond the bath duration. Choose breathable natural fiber socks like cotton or wool rather than synthetic materials that might cause sweating and subsequent chilling. This practice proves especially valuable for evening baths, as warm feet facilitate sleep onset as discussed earlier. Some research suggests that maintaining warmth for thirty to sixty minutes after bathing provides the most sustained circulation improvements.
Adding substances to bath water represents a common practice with varying evidence for benefits. Epsom salts, chemically magnesium sulfate, have a long tradition in therapeutic bathing. While evidence for magnesium absorption through skin remains debated, Epsom salts may reduce inflammation and promote relaxation through mechanisms not fully understood. For healthy individuals, adding one-half to one cup of Epsom salts to foot bath water is generally safe and might enhance relaxation benefits. However, people with diabetes should avoid additives including Epsom salts unless specifically approved by healthcare providers.
Essential oils added to foot baths provide aromatic benefits that may enhance relaxation, though they don’t improve circulation directly. Lavender oil promotes relaxation and might complement evening baths for sleep improvement. Peppermint oil provides an invigorating sensation some people enjoy. However, essential oils can irritate sensitive skin and should be well diluted, typically no more than a few drops in the entire bath. Never add essential oils to baths for diabetics or people with peripheral neuropathy, as any skin irritation might go unnoticed until becoming severe.
Ginger and mustard powder additions increase vasodilation and the warming sensation. Traditional hydrotherapy practices sometimes recommend adding one to two teaspoons of powdered ginger or mustard per gallon of water. These substances can significantly increase circulation through their natural warming properties, but they also increase burn risks and skin irritation potential. Only healthy adults without diabetes or skin sensitivity should consider these additions, and they should be introduced gradually to assess individual tolerance.
Combining foot baths with other circulation-promoting activities might provide synergistic benefits. Light foot and ankle exercises performed during bathing, such as rotating ankles, flexing and pointing toes, and spreading toes apart, could theoretically enhance circulation by engaging muscle pumps that assist venous return. While formal research on this combination is limited, the practices appear safe and might add marginal benefits. Alternatively, performing these exercises after bathing while feet remain warm provides similar potential advantages.
Environmental factors surrounding the bath influence comfort and potentially effectiveness. A warm room prevents chilling of upper body while feet are warmed, maintaining overall comfort. Good lighting allows inspection of feet before and after bathing. A comfortable chair at appropriate height prevents back strain during the twenty-minute session. These seemingly minor details affect whether people maintain a consistent bathing practice, which ultimately determines real-world effectiveness regardless of theoretical optimal techniques.
Monitoring your response to foot baths helps personalize the practice. Keep mental or written notes about how different temperatures, durations, and frequencies affect your cold feet symptoms. Some people discover they need slightly longer or shorter sessions than the research average to achieve optimal results. Others find certain times of day work better for their circulation and schedules. This individualization within evidence-based guidelines represents ideal healthcare practice: using science to establish a starting point, then adjusting based on personal response.
Common mistakes in bath technique can reduce benefits or increase risks. Adding hot water while feet remain in the container risks burns even in people with normal temperature sensation. Falling asleep during bathing creates drowning risks and allows water to cool below therapeutic temperatures. Using water that’s uncomfortably hot based on misguided beliefs that more heat provides more benefit actually increases injury risk without improving circulation. Bathing immediately after eating can cause digestive discomfort as blood flow diverts from intestines to skin. Avoiding these pitfalls ensures safe, effective practice.
The technique and duration recommendations ultimately serve one goal: making therapeutic foot baths a sustainable, safe, and effective practice that improves circulation and reduces cold feet symptoms. By following evidence-based guidelines while remaining attentive to individual responses and safety considerations, most people can successfully implement this cost-free intervention with meaningful benefits for foot warmth and overall circulation health.
Who Can Benefit Most from Warm Foot Baths
While virtually anyone experiencing cold feet can gain some benefit from properly conducted warm water baths, certain populations stand to experience particularly significant improvements based on their specific circulation challenges. Understanding which groups benefit most helps target this intervention where it can provide maximum impact while ensuring appropriate safety modifications for vulnerable populations.
People with primary Raynaud’s phenomenon represent an ideal population for warm foot bath therapy. This condition, affecting an estimated five to ten percent of the population, causes excessive vasoconstriction in response to cold or stress. During Raynaud’s attacks, blood flow to fingers and toes nearly ceases, causing affected areas to turn white, then blue, then painfully red as circulation eventually returns. These attacks can last minutes to hours, significantly disrupting daily activities and causing considerable distress. Warm water baths address the fundamental problem in Raynaud’s by mechanically overriding the excessive vasoconstriction. The warmth forces blood vessels to dilate despite nervous system signals telling them to constrict. Many Raynaud’s patients report that regular warm foot baths reduce both the frequency and severity of attacks, particularly when baths are timed strategically such as in the evening before bed or upon coming indoors from cold environments.
Individuals experiencing age-related circulation decline benefit substantially from regular foot baths. As people age beyond fifty, multiple factors conspire to reduce peripheral circulation. Blood vessels stiffen and lose elasticity, making vasodilation less robust. Atherosclerotic plaque accumulates even in people without diagnosed vascular disease. Endothelial function declines, reducing nitric oxide production that facilitates vessel dilation. Older adults also frequently take medications like beta-blockers that deliberately reduce peripheral circulation. These cumulative changes often manifest as chronically cold feet that traditional recommendations like wearing warmer socks fail to adequately address. Warm water baths bypass these age-related impairments by directly warming tissues and forcing circulation improvement through thermal mechanisms. Multiple studies specifically examining elderly populations have demonstrated that regular foot baths improve not just immediate comfort but also baseline circulation over time with consistent practice.
Women in the perimenopausal and postmenopausal periods often experience worsening circulation symptoms as hormonal changes affect vascular function. Estrogen plays important roles in maintaining blood vessel health, promoting nitric oxide production, and supporting appropriate vascular tone. As estrogen levels decline during menopause transition, many women notice increasingly cold hands and feet among numerous other symptoms. Hormone replacement therapy addresses these changes for some women, but others prefer non-pharmacological approaches or cannot take hormones due to contraindications. Regular warm foot baths provide a hormone-free intervention that addresses circulation symptoms directly while potentially offering stress reduction benefits that help with other menopausal symptoms.
Office workers and others whose occupations involve prolonged sitting face circulation challenges from sustained immobility. When legs remain still for hours, the muscle pump mechanism that assists venous return operates minimally, allowing blood to pool in leg and foot veins. This venous pooling reduces the pressure gradient driving blood through tissues, potentially contributing to cold feet even in warm offices. Research has shown that even people with healthy circulation develop reduced foot temperature after several hours of sitting. Evening foot baths help restore normal circulation after a day of desk work, potentially preventing the cumulative effects of chronic venous pooling that might eventually progress to varicose veins or more serious complications.
People recovering from lower extremity injuries or surgeries often experience reduced circulation due to prolonged immobilization, tissue swelling, or direct vascular injury. While specific medical guidance should govern any therapeutic interventions during recovery, warm foot baths appropriately timed and cleared by healthcare providers can aid rehabilitation by improving circulation to healing tissues. The enhanced blood flow delivers more oxygen and nutrients while removing metabolic waste products more efficiently, potentially accelerating healing. The warmth also provides comfort and relaxation during the often-frustrating recovery period.
Individuals with hypothyroidism, a condition affecting approximately five percent of the population, frequently complain of cold intolerance including persistently cold feet. The thyroid gland produces hormones that regulate metabolic rate throughout the body. When thyroid function decreases, metabolism slows, reducing heat production and making people feel cold even at normal room temperatures. While thyroid hormone replacement therapy addresses the underlying condition, it often takes weeks to months to fully optimize treatment. During this time, and for people with subclinical hypothyroidism that doesn’t warrant medication, warm foot baths provide symptomatic relief without interfering with medical treatment.
Athletes and physically active individuals might seem unlikely candidates for cold feet problems, but they experience unique circulation challenges. Intense training sometimes triggers overactive sympathetic nervous system responses that cause vasoconstriction. Endurance athletes in particular may develop relatively low resting metabolic rates as their bodies adapt to training demands, potentially contributing to feeling cold at rest. Some athletes report cold extremities despite excellent cardiovascular fitness. Post-workout foot baths provide relaxation while improving recovery through enhanced circulation that helps remove metabolic waste products accumulated during exercise.
People with anxiety disorders or chronic stress experience sympathetic nervous system overactivity that promotes peripheral vasoconstriction. The fight-or-flight response that anxiety triggers includes shunting blood away from extremities toward core organs and large muscle groups in preparation for action. When this stress response becomes chronic, as it does in anxiety disorders, persistently reduced peripheral circulation can result in chronically cold hands and feet. Warm foot baths address this issue through multiple mechanisms: the direct warming effect overcomes vasoconstriction, while the relaxing ritual of bathing may help reduce anxiety levels, creating a beneficial cycle where reduced anxiety further improves circulation.
Individuals living in cold climates or working in cold environments face obvious circulation challenges from environmental temperature exposure. While appropriate clothing helps, some people find their feet remain stubbornly cold despite insulated boots and warm socks. Daily evening foot baths provide relief after cold exposure while potentially helping the body adapt to cold stress over time through mechanisms similar to cold acclimatization seen in people with regular cold water immersion practice. The warm bath offers immediate comfort while potentially building long-term resilience.
People with mild peripheral artery disease who don’t yet require medical interventions might find warm foot baths beneficial as part of comprehensive lifestyle management. While baths won’t reverse arterial blockages, they can help maximize circulation through remaining open vessels. Combined with walking exercise, smoking cessation, and appropriate diet, regular foot baths might help manage symptoms and potentially slow disease progression. However, anyone with diagnosed peripheral artery disease should consult their healthcare provider before starting foot baths to ensure safety and appropriate integration with medical treatment.
Insomnia sufferers represent an interesting group who might benefit from warm foot baths for reasons partially independent of cold feet. Multiple studies have demonstrated that pre-bedtime foot baths improve sleep onset latency and sleep quality through mechanisms involving body temperature regulation. The evening foot bath creates favorable temperature gradients that facilitate the core temperature decline associated with sleep initiation. People whose cold feet actually disrupt sleep gain dual benefits from evening baths: warmer, more comfortable feet and better sleep through thermoregulatory mechanisms.
People using certain medications that impair circulation as a side effect might find symptom relief through regular foot baths. Beta-blockers, commonly prescribed for high blood pressure and heart conditions, deliberately reduce peripheral circulation as part of their therapeutic mechanism. While medically necessary for treating serious conditions, this effect unfortunately causes cold extremities in many users. Recognizing when persistently cold feet require medical evaluation helps distinguish between benign circulation variations and symptoms indicating serious underlying conditions. Healthcare professionals can assess whether cold extremities reflect normal individual variation or warrant further cardiovascular investigation. Calcium channel blockers and some other cardiovascular medications have similar effects. Warm foot baths provide symptomatic relief without interfering with medications’ primary therapeutic actions.
Shift workers whose schedules disrupt normal circadian rhythms often experience various health issues including circulation problems. The body’s temperature regulation follows circadian patterns, with peripheral temperature normally rising in the evening as sleep approaches. Shift work disrupts these patterns, potentially contributing to chronically cold extremities. Strategically timed foot baths might help realign temperature rhythms or at minimum provide symptom relief when circadian disruption causes uncomfortable cold feet at inappropriate times.
Caregivers and healthcare workers who spend long hours on their feet in sometimes cool hospital or facility environments frequently develop cold, aching feet by shift end. The combination of prolonged standing, cool temperatures, and stress conspires to create poor peripheral circulation. Post-shift foot baths address multiple issues simultaneously: improving circulation, reducing inflammation in tired feet, and providing much-needed relaxation after demanding work.
Understanding which populations benefit most helps healthcare providers, family members, and individuals themselves identify when warm foot baths might provide significant value. While nearly everyone with cold feet could experience some improvement, the groups identified here stand to gain the greatest benefits due to their specific circulation challenges, making foot baths a particularly worthwhile intervention to incorporate into their health routines.
Special Considerations for Different Health Conditions
While warm foot baths provide safe, beneficial therapy for most people, certain health conditions require special precautions, modified protocols, or in some cases consultation with healthcare providers before beginning regular bathing. Understanding these special considerations ensures safe practice while maximizing benefits for vulnerable populations whose circulation problems often create the greatest need for effective interventions.
Diabetes demands the most extensive modifications to standard foot bath protocols due to the dual risks of neuropathy and impaired healing. Peripheral neuropathy, affecting more than half of people with longstanding diabetes, damages nerves that sense temperature, pain, and touch. A diabetic person with severe neuropathy might immerse feet in dangerously hot water without feeling discomfort until burns occur. These burns heal slowly or not at all due to diabetes-related circulation problems and immune dysfunction, creating serious infection risks that sometimes require hospitalization or amputation. Cold-related foot injuries extend beyond burns to include conditions like trench foot and chilblains, particularly affecting people who work in cold wet environments. Understanding these risks helps prevent serious complications that could impact mobility and quality of life. The modifications required for safe diabetic foot bathing include absolute temperature limits around 37-40 degrees Celsius, mandatory thermometer use rather than relying on sensation, visual inspection of water temperature before immersion, duration limits around 10-15 minutes to minimize maceration that could create infection entry points, thorough drying especially between toes where moisture promotes fungal infections, and careful post-bath inspection for any skin changes, blisters, or injuries that may have occurred but weren’t felt.
People managing diabetes must prioritize comprehensive foot care extending beyond bathing to include daily inspection, appropriate footwear, and regular medical checkups. Preventing complications requires understanding how diabetes affects circulation and healing while implementing protective strategies consistently.
Healthcare providers often recommend that diabetics have someone else test water temperature and monitor the bathing process, at least initially, providing an extra safety check. Comprehensive diabetes foot care practices extend beyond temperature monitoring to include daily inspection for cuts or blisters, proper nail trimming techniques, and wearing appropriate footwear that prevents injuries. Regular professional foot examinations help detect problems early before they progress to serious complications.Some doctors discourage foot soaking entirely for diabetics due to infection risks, preferring simple washing and thorough drying. Others approve carefully controlled warm baths based on individual circumstances including quality of diabetic control, presence and severity of neuropathy, any history of foot ulcers or infections, and patient reliability in following safety protocols. This variation in medical opinion reflects legitimate concerns about balancing benefits against real risks in a vulnerable population.
Heart disease requires different considerations focused on cardiovascular stress rather than burn risks. Warm water immersion increases blood flow to skin and extremities, which the heart must pump through expanded vascular beds. For people with severe heart failure whose hearts already struggle to meet circulation demands at rest, this additional burden could precipitate symptoms or even acute decompensation. Similarly, people with severe coronary artery disease might experience angina if their diseased coronary arteries can’t increase blood flow enough to meet the heart’s increased demands during warming.
The appropriate precautions for heart disease patients include consultation with cardiologists before starting regular foot baths, starting with shorter duration sessions around 10 minutes and gradually extending if well tolerated, using slightly cooler water around 38-40 degrees Celsius to reduce cardiovascular demands, avoiding bathing soon after meals when blood flow already diverts to digestive organs, monitoring for symptoms like chest pain, unusual shortness of breath, or dizziness during or after bathing, and having someone nearby during initial baths in case assistance becomes needed. Many heart disease patients can safely enjoy foot baths with these precautions, but individual medical guidance ensures appropriateness based on specific cardiac conditions and overall health status.
Pregnancy introduces concerns about both fetal development and maternal circulation changes. Excessive heat exposure during early pregnancy has been associated with increased neural tube defect risks, though evidence specifically regarding foot baths remains limited. Localized foot warming differs substantially from whole-body heating in hot tubs or saunas that generate the clearest risk signals. Nevertheless, pregnant women should exercise caution, limiting water temperature to 38 degrees Celsius maximum, keeping duration to 15 minutes or less, avoiding bathing if feeling unwell or feverish, and stopping immediately if feeling dizzy, nauseated, or experiencing any unusual symptoms.
Later in pregnancy, many women experience increased swelling in feet and ankles due to expanded blood volume and pressure from the growing uterus on pelvic veins. Warm foot baths might provide comfort, though elevation combined with cool compresses may be more appropriate for reducing swelling compared to warm water which could potentially increase fluid accumulation. Pregnant women should discuss foot bathing with their obstetricians to receive personalized guidance based on pregnancy progression and any complications.
Peripheral artery disease creates a situation where people desperately need improved circulation but face potential risks from warm water exposure. Severe arterial blockages can create situations where increasing metabolic demands in tissues through warming exceeds the capacity of blocked arteries to deliver adequate blood flow, paradoxically causing ischemic pain rather than relief. Additionally, people with severe PAD often have reduced temperature sensation similar to diabetic neuropathy, creating burn risks.
The approach for PAD patients involves medical evaluation to assess disease severity before starting foot baths, using conservative temperatures around 38-40 degrees Celsius, watching for increasing pain during bathing which might indicate ischemia, limiting duration initially to 10-15 minutes, and coordinating with vascular specialists who may have specific recommendations based on arterial anatomy and blockage locations. Some PAD patients benefit significantly from warm foot baths while others find that exercise-based therapy like supervised walking programs provides more appropriate treatment. Medical guidance helps distinguish who falls into which category.
Raynaud’s phenomenon, while benefiting greatly from warm foot baths as discussed earlier, requires attention to preventing reactive attacks. Rapid cooling after warming can trigger severe vasoconstriction, potentially worse than the original cold feet. The solution involves gradual temperature transitions, keeping the bathing room warm, having warm socks ready to put on immediately after drying feet, avoiding sudden exposure to cold air or surfaces, and potentially using the bath as preparation before going into cold environments rather than after cold exposure when reactive attacks might occur.
Kidney disease, particularly chronic renal failure, can complicate warm water bathing due to fluid balance issues and cardiovascular stress. The kidneys play crucial roles in regulating blood pressure and fluid volume. When kidney function declines, these regulatory mechanisms fail, potentially making people more vulnerable to blood pressure swings during warm water exposure. Dialysis patients face particular challenges as they already deal with significant fluid and electrolyte fluctuations. Medical guidance becomes essential for people with moderate to severe kidney disease before starting regular foot baths.
Varicose veins might seem to contraindicate warm water exposure based on concerns that heat could worsen venous insufficiency. However, limited evidence suggests that brief warm foot baths probably don’t significantly worsen varicose veins and might even provide comfort through improved circulation. Very hot water or prolonged soaking might theoretically increase venous pressure, but the temperatures and durations recommended for therapeutic foot baths likely fall within safe ranges. People with severe varicose veins should consult vascular specialists, but most with mild to moderate varicosities can likely safely use foot baths with standard protocols.
Active infections including cellulitis or fungal infections might worsen with warm water exposure that promotes bacterial or fungal growth. Open wounds similarly should not be soaked as this could introduce infection, delay healing, or macerate tissue. The appropriate precaution involves treating any active infections completely before starting foot baths, keeping baths scrupulously clean to prevent introducing new infections, discontinuing bathing if any signs of infection develop, and maintaining excellent foot hygiene particularly thorough drying to prevent fungal growth in warm, moist environments.
Blood clotting disorders including thrombocytopenia or people taking anticoagulants face theoretical risks that warrant awareness though probably not absolute contraindication. Warm water causes vasodilation that might increase bruising tendencies in people with impaired clotting. There’s also theoretical concern that warm water might mobilize existing blood clots, though evidence for this risk from foot baths specifically remains minimal. Reasonable precautions include avoiding trauma to feet during bathing, inspecting carefully for any bruising or bleeding afterward, and discussing bathing plans with hematologists or physicians managing anticoagulation therapy.
Autoimmune conditions including lupus and scleroderma often feature Raynaud’s phenomenon as discussed earlier, but they may also involve additional considerations around skin fragility, immunosuppressant medications increasing infection susceptibility, and systemic inflammation. Working with rheumatologists helps ensure foot bath protocols integrate appropriately with overall disease management and don’t create unexpected complications.
Mental health conditions deserve mention not because warm foot baths pose physical risks but because incorporating them into self-care routines might benefit mental wellbeing beyond physical circulation improvements. The ritual of preparing a bath, the enforced twenty-minute break from stressors, and the physical comfort all potentially support mental health. However, foot baths should complement rather than replace evidence-based mental health treatments including therapy and medications when appropriate.
Children generally tolerate warm foot baths well but require adult supervision to ensure safety. Temperature should be tested by adults before allowing children to enter, duration should be shortened to 10-15 minutes for young children, and water depth should be minimal for small children to prevent any drowning risk. Teaching children about safe bathing practices establishes healthy habits while providing current symptom relief for those experiencing cold feet.
The overarching principle across all these special considerations involves balancing potential benefits against real risks in populations where both may be amplified compared to healthy adults. When approached thoughtfully with appropriate precautions and medical guidance where indicated, most people with health conditions can safely incorporate warm foot baths into their wellness routines and potentially experience significant benefits for circulation and overall comfort.
Beyond the Bath: Complementary Strategies for Warm Feet
While warm foot baths provide powerful direct intervention for cold feet, combining them with complementary approaches creates comprehensive circulation support that addresses multiple contributing factors simultaneously. These additional strategies range from simple lifestyle modifications anyone can implement to specific exercises and techniques that enhance long-term circulation health beyond temporary warming effects.
Regular physical activity stands as perhaps the single most important complement to foot baths for improving circulation. Exercise activates muscle pumps in the legs that propel blood back toward the heart against gravity, reduces arterial stiffness by promoting nitric oxide production in blood vessels, helps control risk factors like high blood pressure and elevated cholesterol that impair circulation, maintains healthy body weight reducing metabolic stress on cardiovascular systems, and stimulates development of collateral blood vessels that create alternate circulation routes around blockages. The most effective exercise for leg and foot circulation involves activities that engage leg muscles rhythmically including walking which requires no equipment and suits most fitness levels, swimming which provides non-impact cardiovascular conditioning, cycling whether outdoor or stationary, dancing which combines cardiovascular work with enjoyment, and yoga which improves flexibility while promoting circulation through various poses.
The recommendation to accumulate at least 150 minutes of moderate-intensity aerobic activity weekly provides measurable circulation benefits for most people. Those with existing circulation problems should start gradually and increase activity progressively under medical guidance. Even short walking sessions of ten to fifteen minutes several times daily provide benefits for people unable to sustain longer exercise periods. The key lies in consistency rather than intensity, establishing sustainable activity patterns that improve circulation progressively over weeks and months.
Foot and ankle exercises performed regularly supplement broader physical activity by specifically targeting muscles that assist circulation in the lower legs and feet. Simple movements anyone can perform while sitting include ankle rotations clockwise and counterclockwise ten times each direction, pointing and flexing feet to engage calf muscles that pump blood upward, spreading toes apart then squeezing together to activate small foot muscles, picking up small objects like marbles with toes to develop dexterity and circulation, and performing alphabet exercises by drawing letters in the air with toes to combine movement variety with mental engagement.
These exercises can be incorporated throughout the day during sedentary periods, particularly valuable for office workers or others whose occupations involve prolonged sitting. Performing them during television watching or while reading creates habits that persist without requiring dedicated exercise time. The cumulative effect of frequent brief movement sessions can rival longer dedicated exercise periods in terms of circulation benefits.
Proper footwear selection influences foot temperature and circulation more than many people realize. Shoes that fit correctly without compressing feet allow normal blood flow, natural fibers like leather breathe better than synthetic materials reducing moisture accumulation, adequate insulation protects against cold without excessive thickness that promotes sweating, and sufficient room for toes to move prevents compression that could impair circulation. Conversely, ill-fitting shoes create multiple circulation problems: tight shoes compress blood vessels restricting flow, narrow toe boxes squeeze toes together potentially triggering or worsening conditions like bunions, high heels shift body weight forward causing circulation problems in forefoot, and worn-out shoes provide inadequate support and insulation.
The recommendation to have feet measured regularly and replace shoes when they show significant wear ensures continued appropriate fit and support. Feet can change size with age, weight fluctuations, and certain health conditions, making assumptions about shoe size based on past measurements unreliable. Many people wear shoes that are one or even two sizes too small, creating unnecessary circulation impairment.
Sock selection deserves equal attention to shoe choice. Natural fibers including wool which provides excellent insulation even when damp, cotton which breathes well in moderate temperatures, and bamboo which offers moisture-wicking properties, generally outperform synthetic materials for circulation and comfort. Compression socks designed specifically for circulation support may benefit some people with venous insufficiency or those who sit for prolonged periods, though they should be properly fitted and used according to medical guidance. Poorly fitting compression socks can actually impair circulation rather than improving it.
Avoiding socks with tight elastic bands that constrict lower leg circulation, changing socks when they become damp from sweat, and choosing appropriate thickness for environmental conditions all contribute to optimal foot temperature and circulation. Some people find that wearing light socks to sleep keeps feet comfortably warm without overheating, though others prefer bare feet under covers.
Hydration status affects blood viscosity and circulation efficiency. Dehydration causes blood to become thicker and more difficult to pump through small vessels, potentially contributing to cold extremities. Maintaining adequate hydration by drinking water throughout the day rather than large volumes at once, consuming fruits and vegetables with high water content, limiting excessive caffeine and alcohol which promote fluid loss, and adjusting intake upward during hot weather or increased physical activity ensures blood maintains appropriate viscosity for efficient circulation.
The recommendation to drink enough water that urine remains pale yellow provides a practical hydration assessment method anyone can implement. While specific fluid requirements vary based on body size, activity level, and environmental conditions, most adults need approximately eight to ten cups of fluids daily from all sources. People with heart or kidney conditions requiring fluid restrictions should follow their healthcare providers’ specific recommendations rather than general hydration advice.
Dietary choices influence circulation through multiple mechanisms including effects on blood vessel health, inflammation levels, and blood clot formation. Foods that support circulation include fatty fish rich in omega-3 fatty acids that reduce inflammation and improve blood vessel function, leafy greens providing nitrates that the body converts to nitric oxide for vasodilation, berries containing anthocyanins that strengthen blood vessel walls, nuts offering healthy fats and vitamin E supporting vascular health, and garlic which may have mild blood-thinning and vasodilatory effects. Conversely, foods to limit include those high in saturated and trans fats that promote atherosclerosis, excessive sodium contributing to high blood pressure and fluid retention, refined sugars and carbohydrates that spike blood sugar and promote inflammation, and processed meats containing preservatives that may impair vascular function.
The Mediterranean diet, emphasizing vegetables, fruits, whole grains, fish, olive oil, and moderate red wine consumption, has demonstrated cardiovascular benefits in numerous studies and likely supports peripheral circulation as well. This dietary pattern doesn’t require expensive specialty foods or complicated meal preparation, making it accessible for most people interested in circulation-supporting nutrition.
Stress management deserves recognition as a circulation factor due to stress-induced sympathetic activation causing peripheral vasoconstriction. Chronic stress keeps the body in fight-or-flight mode, maintaining vasoconstriction that contributes to persistently cold extremities. Effective stress reduction techniques include meditation and mindfulness practices that calm nervous system responses, yoga combining gentle movement with mental focus, deep breathing exercises that activate parasympathetic relaxation responses, progressive muscle relaxation systematically releasing tension, and engaging hobbies and activities that provide mental respite from stressors.
The evening foot bath itself can serve as a stress management ritual when approached mindfully rather than as just another task to complete. Taking twenty minutes to focus on the physical sensations of warmth, consciously releasing the day’s tensions, and practicing gratitude or other positive mental exercises transforms the bath from purely physical intervention to mind-body practice supporting overall wellbeing.
Smoking cessation stands as one of the most impactful interventions anyone who smokes can undertake for circulation health. Smoking damages blood vessels through multiple mechanisms including direct toxic effects on endothelial cells, promotion of atherosclerosis and blood clot formation, reduced oxygen delivery to tissues, and vasoconstriction from nicotine. These effects accumulate over years of smoking, but significant improvements begin within weeks of quitting. Cold hands and feet often improve markedly within months of smoking cessation as blood vessels begin recovering from chronic nicotine-induced vasoconstriction.
The difficulty of quitting smoking shouldn’t discourage attempts, as numerous effective support programs, medications, and counseling services exist to help people overcome addiction. Healthcare providers can connect smokers with appropriate resources, and many insurance plans now cover smoking cessation treatments recognizing the enormous health benefits of quitting.
Elevation of feet above heart level whenever practical facilitates venous return and reduces pooling that can contribute to cold feet. Using a footstool while sitting, propping feet on pillows while resting, and sleeping with feet slightly elevated by placing books or blocks under the mattress at the foot of the bed all leverage gravity to assist circulation. This simple intervention costs nothing and can be implemented immediately by anyone experiencing cold feet related to venous insufficiency or prolonged sitting.
Massage of feet and lower legs stimulates circulation through mechanical effects and possibly through reflex mechanisms. While professional massage therapy provides benefits, simple self-massage techniques can be performed daily at minimal cost. Gentle stroking from feet toward knees following venous flow directions, kneading calf muscles to promote blood movement, and circular massage of foot soles all potentially enhance circulation beyond what passive warming alone achieves.
Temperature acclimatization through controlled cold exposure represents a more advanced strategy that some people find beneficial. Brief cold water foot baths or cold showers following warm bathing may trigger adaptive responses that improve long-term temperature regulation and circulation. However, this approach requires caution and gradual progression to avoid triggering excessive vasoconstriction or other adverse responses. People with Raynaud’s phenomenon or severe circulation problems should avoid deliberate cold exposure unless under medical supervision.
The synergy between warm foot baths and these complementary strategies creates comprehensive circulation support exceeding what any single intervention achieves alone. A person who combines daily twenty-minute foot baths with regular walking, improved nutrition, adequate hydration, stress management, and appropriate footwear addresses circulation from multiple angles simultaneously, maximizing the likelihood of significant sustained improvement in cold feet symptoms and overall vascular health.
Common Mistakes to Avoid
Understanding what not to do proves as important as knowing proper techniques when implementing therapeutic foot baths. Several common mistakes can reduce effectiveness, create safety hazards, or even worsen circulation problems rather than improving them. Recognizing these pitfalls allows people to avoid them, ensuring safe and effective bathing practices that maximize benefits.
Using water that’s too hot represents perhaps the most dangerous mistake, driven by the misconception that hotter water provides greater circulation benefits. In reality, water above 43 degrees Celsius increases burn risks substantially without proportional therapeutic gains. People with normal temperature sensation will find excessively hot water uncomfortable and instinctively withdraw feet, but those with diabetic neuropathy or other conditions impairing sensation might not feel pain until significant tissue damage has occurred. The solution involves always testing water temperature with a reliable thermometer, never relying solely on how water feels, starting at lower temperatures around 38-40 degrees Celsius and increasing gradually if desired, and establishing firm upper limits around 42 degrees for healthy adults and lower for people with diabetes or neuropathy.
The consequences of burn injuries extend beyond immediate pain, particularly for people with diabetes or circulation problems whose compromised healing abilities turn minor burns into serious infections requiring prolonged treatment or even hospitalization. Prevention through proper temperature control proves far simpler than treating burn complications.
Failing to dry feet thoroughly after bathing, particularly between toes, creates ideal conditions for fungal infections including athlete’s foot. The warm, moist environment following a bath provides perfect breeding grounds for fungi that naturally exist on skin but proliferate when conditions favor their growth. These infections cause itching, burning, and unpleasant odors while potentially spreading to toenails where they become much harder to treat. The preventive approach involves using clean towels for each bath, patting feet dry thoroughly rather than rubbing which could irritate softened skin, paying special attention to spaces between toes where moisture accumulates, and inspecting between toes for any signs of redness, maceration, or unusual odor that might indicate developing infection.
For people with diabetes or compromised immune systems, even minor fungal infections can progress to serious complications including bacterial superinfections that penetrate deeper tissues. The simple act of thorough drying becomes a critical safety measure in these populations.
Bathing too frequently or for excessive duration causes skin problems by stripping natural oils that protect and moisturize. While daily twenty-minute foot baths appear safe for most people, bathing multiple times daily or extending sessions beyond thirty minutes risks excessive skin dryness, cracking, and irritation. Some people mistakenly believe that more bathing provides more benefit, creating problems through overuse of an otherwise beneficial intervention. The balanced approach involves limiting bathing to once daily maximum for most purposes, keeping duration to the evidence-based twenty to twenty-four minute range, moisturizing feet after each bath to replace oils lost during washing, and reducing frequency if signs of excessive dryness appear despite moisturizing.
Skin changes indicating problematic bathing frequency include flaking or peeling skin, increased itching or irritation, redness or inflammation, and paradoxically, increased fungal infection susceptibility as damaged skin barriers allow easier organism penetration. Adjusting practices before these problems develop prevents the need to suspend bathing temporarily while skin heals.
Adding inappropriate substances to bath water creates various risks depending on the additive. Essential oils in excessive concentration can cause skin irritation or allergic reactions. Harsh substances like bleach sometimes mistakenly used based on internet cleaning recommendations can severely damage skin. Even seemingly benign additives like bubble bath or body wash can alter water properties in ways that increase skin drying or irritation. The safe approach involves using plain water for most baths, adding only well-established therapeutic substances like Epsom salts in appropriate amounts, avoiding essential oils unless properly diluted and tested for individual tolerance, never using household cleaning products or other harsh chemicals, and discontinuing any additive that causes skin irritation, unusual odor, or other concerning changes.
For people with diabetes, any additives including Epsom salts should be avoided unless specifically approved by healthcare providers, as even minor skin reactions could progress to serious complications in this vulnerable population.
Bathing immediately after eating diverts blood flow from digestive organs to skin, potentially causing digestive discomfort or in people with cardiovascular disease, insufficient blood supply to meet all demands simultaneously. While not dangerous for most people, this timing can cause bloating, nausea, or general discomfort that reduces enjoyment of the bath. The solution involves waiting at least thirty to sixty minutes after substantial meals before bathing, scheduling baths before meals rather than after when practical, and reducing meal size if bathing soon afterward becomes necessary. People with diagnosed digestive disorders or cardiovascular disease should exercise particular caution about post-meal bathing, potentially waiting even longer or checking with healthcare providers about appropriate timing.
Standing abruptly after bathing causes orthostatic hypotension in many people as blood pressure drops when gravitational effects suddenly increase. The warm bath dilates blood vessels throughout the body, reducing blood pressure during bathing. Upon standing quickly, blood pools in leg veins before compensatory mechanisms can activate, temporarily reducing blood flow to the brain and causing dizziness or even fainting. Falls resulting from bathing-related dizziness can cause serious injuries, particularly in elderly individuals with osteoporosis increasing fracture risks. The prevention strategy involves sitting for one to two minutes after removing feet from water, standing slowly while holding stable furniture or walls for support, remaining still briefly after standing to allow circulation to stabilize, and walking slowly at first until balance and stability feel normal.
People with particularly low blood pressure, those taking blood pressure medications, and elderly individuals should be especially vigilant about gradual position transitions after bathing. Having someone nearby during initial baths provides safety backup until the person has established that they tolerate bathing without significant orthostatic symptoms.
Neglecting to monitor water temperature throughout the bath allows temperature to drift below therapeutic levels as heat dissipates into surrounding air and container. A bath that starts at 41 degrees Celsius might cool to 35 degrees after fifteen minutes without active temperature maintenance, reducing circulation benefits during the latter portion of the bath. The solution involves checking temperature periodically with a thermometer, adding small amounts of hot water when temperature drops more than two to three degrees below target, always removing feet before adding hot water to prevent burns, and stirring or mixing water thoroughly after adding hot water to ensure even temperature before replacing feet.
Some people use temperature-controlled foot bath devices that maintain constant warmth, eliminating this particular concern. However, most home users employ simple containers requiring active temperature management throughout the bath duration.
Bathing in unhygienic conditions or reusing dirty water introduces infection risks, particularly for people with skin breaks, diabetes, or weakened immune systems. Bacteria and fungi can proliferate in warm water, potentially causing infections if they contact susceptible tissues. The hygiene practices include using clean containers for each bath, changing water between multiple baths on the same day, cleaning and drying the bathing container thoroughly between uses, using fresh clean towels for each bath, and never sharing bath water or towels between family members to prevent cross-contamination.
For people with open wounds, cuts, or any breaks in skin integrity, delaying foot baths until these heal prevents introducing infections into vulnerable tissues. Medical consultation helps determine when resuming bathing becomes safe after injuries or foot procedures.
Ignoring worsening symptoms or developing problems represents a serious mistake that can allow minor issues to progress into major complications. Signs warranting immediate medical attention include skin that remains very red or develops blisters suggesting burns, new numbness or tingling potentially indicating nerve problems, unusual pain during or after bathing, visible skin breaks, ulcers, or wounds, and signs of infection including increased warmth, redness, swelling, or drainage. The appropriate response involves suspending foot baths immediately when concerning symptoms develop, seeking prompt medical evaluation rather than waiting to see if problems resolve, providing detailed information to healthcare providers about bathing practices, and following medical advice about when resuming bathing becomes safe.
People with diabetes must be particularly vigilant about any foot changes given their elevated risk for serious complications from seemingly minor injuries or infections.
Using foot baths as a substitute for needed medical care rather than as a complement to it delays appropriate treatment of underlying conditions. While warm baths provide symptomatic relief for cold feet, they don’t treat peripheral artery disease, diabetes, thyroid disorders, or other conditions that might be causing circulation problems. The balanced approach involves using foot baths for symptom management while pursuing appropriate medical diagnosis and treatment, consulting healthcare providers about persistent cold feet to rule out serious conditions, and integrating baths into comprehensive treatment plans rather than relying on them exclusively. Some circulation problems require medications, procedures, or other medical interventions that foot baths can’t replace, though they can complement medical treatment by providing additional symptom relief.
Avoiding these common mistakes ensures that warm foot baths remain a safe, effective, beneficial intervention for cold feet rather than creating new problems. Most mistakes prove easily preventable through attention to proper techniques, safety precautions, and common sense. The modest effort required to implement foot baths correctly yields substantial returns in improved circulation, greater comfort, and reduced risk of complications.
Conclusion
The journey through understanding cold feet and the therapeutic power of properly温度されたwarm water baths reveals a remarkable truth: some of the most effective healthcare interventions require neither prescriptions nor significant expense, but rather informed application of simple approaches validated by both traditional wisdom and modern science. The convergence of research from multiple countries and disciplines has established that foot baths performed at specific temperatures for precise durations provide measurable circulation improvements that translate into real symptom relief for millions of people experiencing chronically cold feet.
The evidence base supporting warm foot bath therapy has grown substantially in recent years, moving this practice from folk remedy status to scientifically validated intervention. Studies using sophisticated measurement techniques including laser Doppler flowmetry, infrared thermography, and temperature gradient calculations have demonstrated that twenty to twenty-four minute foot baths at temperatures between 40 and 42 degrees Celsius produce peripheral vasodilation that increases blood flow not just to feet but throughout the body. This systemic circulation improvement extends beyond the bath duration, creating sustained benefits that accumulate with consistent practice over weeks and months.
What makes this intervention particularly valuable in contemporary healthcare contexts is its accessibility and sustainability. Unlike medications requiring ongoing prescriptions and costs, or specialized devices demanding significant investments, warm foot baths require only water, heat, a container, and a thermometer. These minimal requirements place effective circulation therapy within reach of nearly everyone regardless of economic circumstances, geographic location, or access to advanced medical facilities. In an era when healthcare costs burden individuals and healthcare systems globally, interventions that provide genuine benefits without financial barriers deserve serious consideration and wider implementation.
The comprehensive safety profile of appropriately performed foot baths further enhances their appeal. While certain populations require modifications to standard protocols, particularly people with diabetes, heart disease, or pregnancy, most individuals can safely implement foot baths with minimal risk when following evidence-based temperature, duration, and technique guidelines. The common mistakes discussed earlier prove readily avoidable through basic education and attention to proper procedures. Compared to many medical interventions carrying significant side effect burdens, warm foot baths present remarkably favorable risk-benefit ratios for most users.
The multiple mechanisms through which foot baths improve circulation help explain their effectiveness. Direct warming of foot tissues triggers local vasodilation through temperature-dependent relaxation of smooth muscle in blood vessel walls. This local effect propagates systemically as increased peripheral blood flow reduces overall vascular resistance, potentially lowering blood pressure slightly while improving overall circulation efficiency. The thermal load from warming activates various physiological responses including increased cardiac output, enhanced nitric oxide production, and reduced sympathetic nervous system activity, all contributing to sustained circulation improvements beyond the immediate warming period.
The complementary benefits of foot baths extend beyond circulation to include stress reduction, improved sleep quality, and enhanced overall wellbeing. The ritual of preparing a bath, setting aside twenty minutes for self-care, and experiencing the physical comfort of warmth provides mental and emotional benefits that synergize with physiological improvements. In populations experiencing chronic stress or anxiety that contributes to their circulation problems through sympathetic overactivity, these psychological benefits may enhance overall effectiveness beyond what purely physical warming achieves.
Integrating foot baths into daily routines requires minimal time investment relative to the potential returns. Twenty-four minutes represents less than two percent of waking hours, yet this brief daily practice can significantly impact comfort, circulation health, and quality of life for people whose cold feet disrupt sleep, limit activities, or cause ongoing distress. The evening timing that research suggests as optimal serves dual purposes by both improving circulation and facilitating better sleep through favorable temperature gradient effects, maximizing efficiency of the time invested.
The potential population health impact of wider foot bath adoption deserves consideration. If even a fraction of the millions experiencing cold feet symptoms implemented regular evidence-based bathing practices, the aggregate improvement in quality of life, reduction in healthcare utilization for circulation complaints, and decreased reliance on medications for symptom management could prove substantial. Public health initiatives promoting foot bath education might cost-effectively improve wellbeing across large populations, particularly in aging societies where circulation problems become increasingly prevalent.
Future research directions might further optimize foot bath protocols by investigating individual variation in optimal temperatures and durations, examining long-term outcomes in people using baths consistently over years, studying combination approaches integrating baths with other circulation interventions, and exploring potential benefits for additional conditions beyond simple cold feet. As our understanding of circulation physiology deepens, opportunities may emerge to personalize bathing recommendations based on individual characteristics, genetic factors, or specific circulation problems.
The convergence of ancient practices and modern science exemplified by warm foot bath therapy reminds us that effective healthcare interventions need not be complex, expensive, or technologically advanced. Sometimes the simplest approaches, when applied with understanding of underlying mechanisms and proper attention to safety, provide benefits rivaling or exceeding those of more elaborate interventions. This insight should encourage both healthcare providers and individuals to consider low-cost, accessible interventions alongside conventional medical approaches, creating comprehensive treatment strategies that maximize benefits while minimizing burdens.
For the individual reader experiencing cold feet, the message proves clear: warm water baths performed correctly represent a safe, effective, scientifically supported intervention worthy of consistent implementation. The investment of twenty minutes daily and the minimal cost of water and heat can yield substantial returns in comfort, circulation health, and overall wellbeing. Combined with complementary approaches including regular physical activity, appropriate footwear, good nutrition, and stress management, foot baths become part of comprehensive circulation care that addresses cold feet at multiple levels simultaneously.
As we move forward in a healthcare landscape increasingly focused on prevention, patient empowerment, and cost-effective interventions, practices like therapeutic foot bathing deserve greater recognition and promotion. They embody principles of accessible, sustainable healthcare that respects both individual autonomy and evidence-based practice. The simple act of warming one’s feet in properly温度されたwater, practiced consistently and mindfully, demonstrates how taking control of one’s health need not require expensive interventions or complex medical protocols, but rather informed application of straightforward practices validated by science and sustained by commitment to self-care.
Frequently Asked Questions
Question 1: What causes cold feet?
Answer 1: Cold feet develop through multiple interconnected mechanisms, with poor peripheral circulation serving as the primary culprit in most cases. When environmental temperatures drop or the body perceives cold stress, the sympathetic nervous system activates vasoconstriction in peripheral blood vessels, dramatically reducing blood flow to extremities. This evolutionary protective response prioritizes vital organs by conserving heat in the body’s core, but leaves hands and feet uncomfortably cold. Beyond environmental factors, numerous medical conditions contribute to chronically cold feet including peripheral artery disease where atherosclerotic plaques narrow arteries reducing blood flow, diabetes which damages both blood vessels and nerves affecting circulation and temperature sensation, hypothyroidism causing reduced metabolic heat production, anemia decreasing blood oxygen-carrying capacity, and Raynaud’s phenomenon triggering excessive vasoconstriction. Lifestyle factors compound these issues, with smoking causing persistent vasoconstriction, sedentary behavior reducing circulation efficiency, and poor footwear choices compressing blood vessels. Understanding the specific cause helps direct appropriate interventions, though warm water baths provide symptomatic relief regardless of underlying etiology.
Question 2: What is the optimal water temperature for a foot bath to improve circulation?
Answer 2: Research conducted across multiple countries and populations has converged on a remarkably consistent optimal temperature range of 40 to 42 degrees Celsius, equivalent to 104 to 108 degrees Fahrenheit, for healthy adults seeking maximum circulation benefits from foot baths. This temperature range effectively triggers robust peripheral vasodilation, forcing blood vessels in feet and legs to dilate despite any sympathetic nervous system signals promoting constriction. Studies using laser Doppler flowmetry to measure blood flow have demonstrated that temperatures in this range increase peripheral circulation to 1.7 to 2.7 times baseline levels, with improvements persisting even after bathing ends. Starting at the lower end of this range around 40 degrees and gradually increasing to personal tolerance ensures safety while maximizing comfort. Certain populations require modified temperature recommendations: people with diabetes should limit water to 37-40 degrees maximum due to burn risks from impaired temperature sensation, pregnant women should not exceed 38 degrees to avoid potential fetal development risks, elderly individuals might benefit from conservative temperatures around 38-40 degrees initially, and those with heart disease should use slightly cooler water around 38-40 degrees to reduce cardiovascular demands. The critical principle applies universally: always test water temperature with a reliable thermometer rather than relying on sensation alone, as subjective temperature perception varies widely between individuals and can be dangerously impaired in people with neuropathy or certain medical conditions.
Question 3: How long should a warm foot bath last for maximum circulation benefits?
Answer 3: Scientific research examining foot bath duration has identified twenty to twenty-four minutes as the optimal timeframe for achieving maximum circulation improvements in most people. This specific recommendation emerges from studies measuring peripheral blood flow during baths of varying lengths, which demonstrated that circulation benefits increase progressively during the first twenty minutes, plateau around the twenty-minute mark, and show minimal additional improvement with longer durations. Japanese researchers found that blood flow to peripheral regions reached 1.7 times baseline after twenty minutes of bathing at 42 degrees Celsius and maintained this elevation without further significant increases beyond twenty-four minutes. Extending bathing beyond twenty-five to thirty minutes begins showing diminishing returns as cardiovascular stress accumulates without proportional circulation gains. However, individual circumstances may require duration modifications: people with heart disease or limited cardiovascular reserves should start with shorter ten to fifteen minute sessions, gradually extending toward twenty minutes as tolerance builds. Elderly individuals might similarly benefit from conservative initial durations with gradual progression. Those using foot baths primarily for relaxation rather than circulation problems might find fifteen minutes sufficient for their purposes. Conversely, some research examining sleep improvements from pre-bedtime foot baths suggests that durations up to thirty minutes might be beneficial specifically when targeting sleep quality rather than just circulation. The practical implementation involves setting a timer when beginning the bath to track duration accurately, avoiding the temptation to extend bathing beyond recommended times based on enjoyment, and remaining attentive to how you feel during bathing, discontinuing if any discomfort, dizziness, or unusual symptoms develop regardless of elapsed time.
Question 4: Can warm foot baths help with conditions like Raynaud’s syndrome?
Answer 4: Yes, warm foot baths provide particularly significant therapeutic benefits for people with Raynaud’s syndrome, a condition characterized by excessive vasoconstriction in fingers and toes triggered by cold exposure or emotional stress. During Raynaud’s attacks, blood flow to affected extremities nearly ceases, causing them to turn white, then blue, then painfully red as circulation eventually returns. These episodes can last from minutes to hours, significantly disrupting daily activities and causing considerable distress. Warm water baths address the fundamental problem in Raynaud’s by mechanically overriding the excessive vasoconstriction through direct tissue warming that forces blood vessels to dilate despite nervous system signals telling them to constrict. Many Raynaud’s patients report that regular preventive foot baths reduce both attack frequency and severity, particularly when baths are strategically timed such as in the evening before bed or upon coming indoors from cold environments. The warm bath essentially provides a controlled environment where circulation can recover fully before the person re-enters potentially triggering situations. However, Raynaud’s patients must exercise caution about temperature transitions after bathing, as rapid cooling can paradoxically trigger reactive vasoconstriction potentially worse than the original cold feet. The solution involves keeping the bathing environment warm, having warm socks ready to put on immediately after drying feet, avoiding sudden exposure to cold air or surfaces after bathing, and potentially using the bath as preparation before going into cold environments rather than only after cold exposure. Water temperature should be kept at the lower end of the therapeutic range around 40 degrees Celsius, as Raynaud’s-affected tissue may be more vulnerable to heat injury during episodes when sensation becomes impaired. Some Raynaud’s sufferers find that combining warm foot baths with stress reduction techniques including meditation, deep breathing, or progressive muscle relaxation provides synergistic benefits by addressing both the physical vasoconstriction and the emotional stress that often triggers attacks.
Question 5: Are there any risks associated with warm foot baths for circulation?
Answer 5: While warm foot baths prove generally safe for most people when performed correctly, several important risks require awareness and appropriate precautions. Burn injuries represent the most immediate danger, particularly for people with peripheral neuropathy from diabetes or other conditions that impair temperature sensation. These individuals might not feel pain from dangerously hot water until significant tissue damage has occurred, with burns potentially progressing to serious infections given impaired healing in diabetic patients. Prevention requires mandatory thermometer use rather than relying on sensation, strict temperature limits around 37-40 degrees Celsius for at-risk populations, and visual inspection before immersion. Cardiovascular stress poses risks for people with severe heart disease whose hearts already struggle to meet circulation demands at rest. Warm water immersion increases blood flow to skin and extremities, requiring the heart to pump through expanded vascular beds, potentially precipitating symptoms or acute decompensation in vulnerable individuals. Those with significant heart disease should consult cardiologists before starting regular foot baths, use conservative temperatures and shorter durations initially, and monitor for symptoms like chest pain or unusual shortness of breath. Orthostatic hypotension affects many people after warm bathing as dilated blood vessels and gravitational effects combine to reduce blood pressure upon standing. This can cause dizziness or fainting with fall risks, particularly in elderly individuals. Gradual position transitions and having stable surfaces to hold while standing prevent most orthostatic problems. Skin problems including excessive dryness, fungal infections, and maceration can develop from overly frequent or prolonged bathing, improper drying, or poor hygiene practices. Limiting bathing to once daily, thorough drying especially between toes, and maintaining cleanliness of bathing equipment prevents most skin complications. Pregnant women face theoretical risks of excessive heat exposure affecting fetal development, requiring temperature limits below 38 degrees Celsius and duration limits around fifteen minutes, though localized foot warming appears considerably safer than whole-body heating. People with active infections, open wounds, or blood clotting disorders require special precautions or temporary bathing suspension to avoid worsening these conditions. The overarching principle involves understanding your individual risk factors, implementing appropriate modifications to standard bathing protocols, and consulting healthcare providers when uncertainty exists about safety for your specific circumstances.
Question 6: How often should I take warm foot baths for cold feet?
Answer 6: For people experiencing chronic cold feet, daily warm foot baths performed consistently provide optimal results by maintaining improved peripheral circulation and progressively enhancing baseline foot temperature over time. Research examining fifteen-day periods of daily foot bathing demonstrated cumulative benefits, with baseline foot temperature showing measurable improvement compared to sporadic bathing schedules. The daily routine establishes regular circulation enhancement similar to how daily medication maintains therapeutic drug levels, though through entirely different mechanisms. Evening timing approximately one to two hours before intended bedtime offers particular advantages by leveraging the body’s natural temperature regulation during sleep preparation while the thermal effects of bathing create favorable temperature gradients associated with faster sleep onset and improved sleep quality. Those using foot baths primarily for acute symptom relief during particularly cold days or after specific cold exposures might find less frequent bathing adequate for their purposes, perhaps three to four sessions weekly when symptoms occur. However, consistency generally produces better long-term outcomes than sporadic intensive use, as the physiological adaptations promoting improved circulation require sustained regular stimulus. Some individuals discover through experimentation that twice-daily bathing provides superior symptom control, particularly those with severe Raynaud’s phenomenon or peripheral artery disease, though skin health considerations including excessive dryness risks necessitate careful monitoring if bathing frequency exceeds once daily. The practical implementation involves establishing bathing as a routine habit similar to tooth brushing or other daily health practices, scheduling it at consistent times that fit reliably into your daily schedule whether morning, evening, or both, allowing the twenty-minute duration plus preparation and post-bath care in your time planning, and maintaining consistency even on days when cold feet symptoms seem less severe, as the cumulative benefits depend on regular practice regardless of daily symptom variation. People with demanding schedules might question whether daily twenty-four minute commitments justify the benefits, but consider that this represents less than two percent of waking hours while potentially significantly improving comfort and quality of life for those whose cold feet disrupt sleep, limit activities, or cause ongoing distress. The time investment becomes particularly justifiable when considering that foot baths simultaneously provide relaxation and stress reduction benefits beyond just circulation improvement, creating multiple returns on the invested time.
Question 7: Do cold feet always indicate a serious health problem?
Answer 7: No, cold feet do not necessarily indicate serious health problems, as many people experience occasional or even persistent cold feet due to benign factors that require no medical intervention beyond simple comfort measures. Normal physiological responses to environmental cold include vasoconstriction in extremities as the body prioritizes core temperature maintenance, a completely appropriate survival mechanism that leaves feet cold but doesn’t signal disease. Individual variation in circulation efficiency means some people naturally have colder extremities than others without underlying pathology, influenced by factors including body composition with people having lower body fat experiencing more heat loss, gender differences with women on average having colder hands and feet than men, and genetic factors affecting peripheral circulation that run in families. Lifestyle factors frequently contribute to benign cold feet including sedentary behavior reducing circulation efficiency, inadequate clothing or footwear for environmental conditions, and high stress levels promoting sympathetic nervous system activation and vasoconstriction. However, certain warning signs suggest that cold feet might indicate serious conditions requiring medical evaluation: persistently cold feet that feel cold to touch regardless of environmental temperature or clothing, color changes including pale, blue, or mottled appearance suggesting severe circulation impairment, pain accompanying coldness particularly if pain occurs during walking and improves with rest suggesting peripheral artery disease, numbness or tingling indicating possible nerve damage, differences between feet with one consistently colder than the other potentially indicating localized circulation problems, and associated symptoms including unexplained weight changes, unusual fatigue, or other systemic symptoms suggesting thyroid disorders or other conditions. The appropriate approach involves first trying simple interventions including wearing warmer socks and appropriate footwear, staying physically active to promote circulation, managing stress through relaxation techniques, and ensuring adequate hydration, then implementing regular warm foot baths as described in this article. If cold feet persist despite these measures, worsen over time, or occur alongside other concerning symptoms, medical evaluation becomes warranted to rule out peripheral artery disease, diabetes, thyroid disorders, anemia, Raynaud’s phenomenon, or other treatable conditions. Primary care physicians can perform initial evaluations including physical examination, blood pressure measurements in ankles and arms, blood tests assessing thyroid function and blood counts, and referrals to specialists when indicated. Early detection of serious circulation problems allows for timely treatment that can prevent complications including tissue damage, infections, or in severe cases, amputations, making medical consultation appropriate when uncertainty exists about whether cold feet represent benign inconvenience or symptoms of underlying disease requiring treatment.
Question 8: What water depth is most effective for circulation improvement?
Answer 8: Research comparing different water depths during foot bathing has identified mid-calf level, approximately ten to fifteen centimeters above the ankles, as optimal for maximizing peripheral circulation improvements while maintaining practical safety and efficiency. Studies examining ankle-deep, mid-calf, and knee-high water levels found that mid-calf depth provided superior circulation benefits compared to ankle-only immersion while offering little additional advantage from deeper knee-level bathing that required substantially more water volume and larger containers. The physiological explanation relates to the density of blood vessels throughout the lower leg that benefit from direct thermal exposure: ankle-only bathing warms foot tissues but misses the extensive vascular networks in the calf muscles where the muscle pump mechanism assists venous return. Warming these calf vessels enhances overall leg circulation more effectively than feet-only warming. Conversely, extending water above mid-calf to knee level or higher increases cardiovascular demands as more body surface area undergoes warming, requiring the heart to pump blood through increasingly expanded peripheral vascular beds. For most people, this additional cardiovascular stress doesn’t provide proportional circulation benefits, making mid-calf the sweet spot balancing effectiveness against demands on the cardiovascular system. Practical advantages of mid-calf depth include requiring moderate water volumes achievable in standard foot bath containers or small plastic tubs, allowing comfortable positioning where feet rest flat on container bottoms while calves remain immersed, minimizing water spillage risks compared to deeper bathing requiring fuller containers, and providing adequate thermal mass for stable temperature maintenance throughout twenty-minute sessions. People with severe heart disease might benefit from even shallower bathing initially, perhaps ankle-deep only, progressing to mid-calf depth as cardiovascular tolerance builds. Those with limited mobility who struggle with deeper container access might find ankle-level bathing sufficient rather than skipping bathing entirely due to difficulty with deeper immersion. Pregnant women concerned about excessive heat exposure might similarly choose conservative ankle-depth bathing as a precaution. The container selection should accommodate both feet comfortably side by side with water reaching mid-calf level when feet rest naturally on the bottom, typically requiring containers approximately thirty centimeters deep and forty to fifty centimeters wide. Specialized foot bath devices often feature built-in depth indicators or designs that naturally position water at optimal levels. Home users employing simple plastic tubs or buckets can mark desired water levels on container exteriors for consistent filling. The positioning during bathing influences how effectively mid-calf depth functions: sitting in a comfortable chair allows natural foot and leg positioning where full calf immersion occurs without awkward angles or muscle tension that might impair circulation benefits.
Shop on AliExpress via link: wholesale-foot-bath-massager
Question 9: Can I add anything to the water to enhance circulation benefits?
Answer 9: For healthy individuals without diabetes, several substances can be added to foot bath water potentially enhancing benefits beyond what plain warm water alone provides, though the temperature itself remains the primary therapeutic factor. Epsom salts, chemically magnesium sulfate, have the longest tradition in therapeutic bathing with many people reporting enhanced relaxation and reduced muscle soreness, though scientific evidence for magnesium absorption through skin remains debated and mechanisms of benefit aren’t fully elucidated. Adding one-half to one cup of Epsom salts to the bathing water appears safe for most healthy adults and might provide additional relaxation benefits complementing circulation improvements. Some research suggests Epsom salts reduce inflammation through mechanisms independent of magnesium absorption, potentially explaining reported benefits. Essential oils added in small quantities provide aromatic benefits that may enhance relaxation and stress reduction complementing physical warming effects. Lavender oil promotes relaxation making it appropriate for evening baths targeting both circulation and sleep improvement. Peppermint oil provides an invigorating sensation some people enjoy though it should be used sparingly as it can be irritating. Eucalyptus oil might benefit people combining foot bathing with cold or respiratory symptom management. However, essential oils require cautious use: they must be well diluted, typically no more than a few drops in the entire bath, they can cause skin irritation or allergic reactions requiring patch testing before widespread use, and they should never be used in foot baths for people with diabetes, peripheral neuropathy, or other conditions impairing sensation or healing due to risks of undetected skin reactions. Ginger powder or mustard powder added at rates of one to two teaspoons per gallon of water increases vasodilation through their natural warming properties, potentially enhancing circulation benefits beyond what temperature alone achieves. However, these substances also increase burn risks and skin irritation potential, making them appropriate only for healthy adults without diabetes or sensitive skin, and they should be introduced gradually to assess individual tolerance. Importantly, people with diabetes should avoid ALL additives including Epsom salts, essential oils, and spice powders unless specifically approved by healthcare providers, as even minor skin reactions could progress to serious complications in this vulnerable population. The diabetic foot’s impaired healing ability and reduced sensation creates situations where irritation from additives might go unnoticed until becoming severe infections requiring aggressive treatment. For most purposes, plain warm water at appropriate temperature provides the primary circulation benefits, with additives offering secondary enhancements primarily in relaxation and enjoyment domains rather than fundamentally improving circulation beyond what temperature achieves. People uncertain about whether specific additives are safe for their circumstances should consult healthcare providers before experimenting. The bathing water itself should always be clean, ideally fresh from municipal water supplies or wells, avoiding reuse of water from previous baths to prevent bacterial or fungal growth that could cause infections. Some people add small amounts of mild soap for cleansing purposes, though this should be followed by thorough rinsing and drying to prevent excessive skin drying or residue accumulation. The overarching principle involves recognizing that warm water temperature remains the active ingredient providing circulation benefits, while additives might enhance enjoyment, relaxation, or provide marginal supplementary benefits without fundamentally changing the physiological mechanisms by which temperature improves blood flow to feet and legs.
Question 10: How quickly will I notice improvement in cold feet with regular warm baths?
Answer 10: The timeline for experiencing noticeable improvements in cold feet from regular warm bath practice varies considerably depending on baseline circulation status, consistency of bathing, and individual physiological factors, though most people experience some benefits on multiple timeframes. Immediately during and shortly after each bath, nearly everyone experiences obvious warming as the direct thermal effects increase foot temperature and dilate blood vessels, providing instant symptom relief that lasts from thirty minutes to several hours depending on environmental conditions and individual circulation efficiency. This immediate benefit alone justifies bathing for many people even before longer-term circulation improvements develop. Within the first week of daily bathing, many people notice that their feet feel warmer for progressively longer periods after each bath, suggesting early adaptations in vascular responsiveness where blood vessels dilate more readily and maintain dilation longer. Research examining continuous daily bathing over fifteen-day periods has demonstrated progressive improvements in baseline foot temperature measurable with thermography, meaning feet maintain warmer temperatures even before bathing as vascular function improves. These early improvements typically become subjectively noticeable within one to two weeks for people with moderate circulation impairment, though those with severe peripheral artery disease or other serious conditions might require longer to experience measurable changes. Long-term vascular health improvements requiring several weeks to months of consistent practice include development of collateral circulation where new small blood vessels form creating alternate routes around blockages, improved endothelial function enhancing nitric oxide production and vascular responsiveness, reduced arterial stiffness as vessels regain some elasticity, and decreased baseline sympathetic nervous system activity promoting less persistent vasoconstriction. These structural and functional changes accumulate gradually with sustained regular practice rather than appearing suddenly, similar to how cardiovascular fitness improves progressively with consistent exercise rather than overnight. Individual variation significantly influences improvement timelines based on multiple factors: people with milder circulation problems generally respond faster than those with severe peripheral artery disease, younger individuals often experience quicker improvements than elderly people whose vascular systems have undergone more age-related changes, non-smokers improve faster than current smokers in whom ongoing tobacco use continues impairing circulation, and those combining foot baths with complementary interventions including regular exercise, improved nutrition, and stress management typically see better results than those relying solely on bathing. Setting realistic expectations helps maintain commitment to consistent practice: immediate symptom relief justifies bathing from the first session, noticeable improvements in baseline foot warmth typically require one to two weeks of daily practice, and substantial long-term vascular health benefits accumulate over months of sustained consistent bathing combined with other circulation-supporting lifestyle factors. People who don’t notice improvements within two to three weeks of consistent proper bathing should reassess their technique ensuring appropriate temperature, duration, and frequency, consider whether underlying medical conditions might be limiting response, and consult healthcare providers to rule out serious circulation problems requiring medical treatment beyond what bathing alone can provide. The key message involves recognizing that warm foot baths provide both immediate symptom relief valuable in itself and progressive long-term circulation improvements that develop with sustained practice, making consistent daily bathing worthwhile for managing chronic cold feet even though substantial improvements require time and commitment similar to other beneficial health practices including exercise, dietary changes, or stress management techniques.
Articles related:
Tags
📧 Get More Articles Like This
Subscribe to receive product reviews and buying guides in your inbox!
We respect your privacy. Unsubscribe at any time.