Smart Health Mirrors vs Wearables vs At-Home Lab Tests: Future of Health Monitoring

Table of Contents
- Introduction: The Health Monitoring Revolution
- Smart Health Mirrors: Your Daily Health Checkpoint
- Wearable Technology: Continuous Health Tracking
- At-Home Lab Tests: Deep Health Insights
- Accuracy and Reliability Comparison
- Cost Analysis and Value Assessment
- Technology Integration and Data Ecosystem
- Future Trends and Emerging Technologies
- Conclusion: Choosing Your Health Monitoring Strategy
Introduction: The Health Monitoring Revolution
The morning ritual had become so ordinary that Marcus barely noticed it anymore. He stood before his bathroom mirror, and within thirty seconds, the display showed his heart rate, blood pressure, body temperature, and even detected a slight irregularity in his breathing pattern that he hadn’t consciously noticed. The mirror suggested he might be developing a minor respiratory infection two days before he felt any symptoms. This wasn’t science fiction or a luxury available only to the wealthy. This was January 2026, and personal health monitoring had transformed from occasional doctor visits into continuous, sophisticated self-assessment available to millions of people worldwide. The revolution happening in bathrooms, on wrists, and through simple mail-order test kits represented the most significant shift in preventive healthcare since the invention of the stethoscope. But with three distinct technological approaches now competing for consumer attention and healthcare dollars, understanding which tools truly deliver value versus which merely collect dust on bathroom counters had become crucial for anyone serious about managing their health proactively.
The transformation began innocuously enough with fitness trackers counting steps and monitoring sleep patterns. But technology advanced rapidly, driven by miniaturized sensors, artificial intelligence breakthroughs, and growing consumer demand for health autonomy. What started as glorified pedometers evolved into sophisticated medical-grade devices capable of detecting atrial fibrillation, measuring blood oxygen levels, tracking menstrual cycles, and even providing preliminary electrocardiogram readings. Simultaneously, mirror manufacturers recognized an opportunity to transform the most-visited household fixture into an intelligent health monitoring station. Smart mirrors leveraged the natural human behavior of looking at oneself multiple times daily, embedding sensors that could assess vital signs without requiring any conscious effort from users. Meanwhile, laboratory testing companies democratized access to diagnostic blood work, allowing anyone to order comprehensive metabolic panels, hormone assessments, and genetic screening without a doctor’s order, receiving results directly through smartphone applications within days.
Before delving into the details of the article, to benefit from this, watch this video which provides a demonstration of one of the smart mirrors equipped with AI technology that analyzes health data:
These three technological approaches emerged from different origins but converged on a common promise: empowering individuals with unprecedented insight into their physiological state, enabling early detection of health problems, and facilitating data-driven conversations with healthcare providers. Yet each technology operated fundamentally differently, measured distinct health parameters, and suited different lifestyles and health goals. The smart health mirror offered passive monitoring during daily routines, requiring no behavior change beyond standing in front of it for less than a minute. Wearable devices provided continuous tracking throughout the day and night, accumulating massive datasets about physical activity, heart function, and sleep quality that revealed patterns invisible in occasional measurements. At-home lab tests penetrated beneath the surface, analyzing the biochemical markers that revealed metabolic function, hormone balance, nutritional deficiencies, and disease markers that no external sensor could detect.
The healthcare establishment initially approached these consumer technologies with skepticism. Traditional healthcare delivery models focused on episodic care during scheduled appointments, but public health data strategies have evolved to incorporate continuous monitoring capabilities. CDC remote monitoring initiatives recognize that real-time health surveillance between clinical visits can dramatically improve chronic disease outcomes and enable earlier intervention when problems develop. Traditional medical practice relied on periodic assessments during scheduled appointments, with physicians controlling the diagnostic process and interpreting results within established clinical frameworks. The democratization of health data challenged this model, raising concerns about accuracy, interpretation errors, unnecessary anxiety from false positives, and the risk that consumers might make dangerous health decisions based on unreliable information. However, attitudes shifted as evidence accumulated demonstrating that personal health monitoring could detect problems earlier, improve medication adherence, reduce emergency room visits for chronic disease patients, and increase patient engagement in their own health management. Clinical research validates the effectiveness of continuous monitoring approaches. NIH remote patient monitoring studies have documented measurable improvements in chronic disease management outcomes, with patients using connected health devices showing better adherence to treatment protocols and fewer acute care episodes compared to traditional care models. Regulatory agencies responded by establishing frameworks that distinguished between general wellness devices subject to minimal oversight and medical devices making diagnostic claims that required rigorous validation. This regulatory evolution enabled innovation while attempting to protect consumers from misleading or dangerous products.
By 2026, the market had matured considerably. Early enthusiasm for any gadget promising health insights gave way to more sophisticated consumer understanding about what different technologies could and couldn’t deliver. Smart health mirror concepts that seemed futuristic in 2025 were approaching commercial reality, with major manufacturers demonstrating prototypes that integrated multiple sensing technologies into a single elegant package. Wearable technology had become mainstream, with penetration rates exceeding fifty percent in developed markets and accuracy improvements narrowing the gap between consumer devices and clinical equipment. At-home lab testing had exploded into a multi-billion dollar industry, with dozens of companies competing to offer convenient, affordable access to the diagnostic tests previously available only through healthcare providers. This convergence created both opportunity and confusion. Consumers faced a bewildering array of options, each with different capabilities, costs, and limitations.
The fundamental question confronting health-conscious individuals in 2026 wasn’t whether to adopt personal health monitoring technology, but rather which combination of technologies would best serve their specific needs, health goals, and budget constraints. A marathon runner training for peak performance had different monitoring requirements than a cardiac patient managing heart disease or a perimenopausal woman tracking hormone fluctuations. Understanding the strengths and limitations of each technological approach had become essential for making informed decisions. The stakes were significant. Investing in the wrong technology meant wasted money on devices that collected data without providing actionable insights. More seriously, over-reliance on inaccurate measurements could lead to false reassurance about deteriorating health conditions or unnecessary anxiety driving expensive medical investigations for phantom problems. Conversely, the right combination of monitoring technologies could detect life-threatening conditions years before symptoms appeared, optimize athletic performance, guide dietary and lifestyle interventions, and provide peace of mind through continuous surveillance of vital health parameters.
Smart Health Mirrors: Your Daily Health Checkpoint
The concept of a smart health mirror sounds almost magical to anyone raised in an era when health assessment required medical appointments and invasive procedures. Peer-reviewed research validates the potential of contactless health monitoring through everyday fixtures. npj Digital Medicine smart mirror studies demonstrate how computer vision and deep learning enable medical-quality health assessments through simple reflection-based monitoring, fundamentally changing how individuals can track health status daily without conscious effort. Standing before a mirror for thirty to forty-five seconds while an integrated system scans your face and body, measuring vital signs and detecting changes invisible to the naked eye, represents a fundamentally different approach to health monitoring. The technology underlying smart mirrors combines multiple disciplines including computer vision, artificial intelligence, photoplethysmography, thermal imaging, and spectral analysis to extract health information from visual data. Unlike wearable devices that require physical contact with skin or lab tests that analyze biological samples, smart mirrors perform completely non-contact assessment using cameras, infrared sensors, and sophisticated algorithms that interpret subtle variations in skin color, temperature distribution, facial features, and body composition. This passive monitoring approach offers unique advantages, particularly for individuals who dislike wearing devices or forget to use them consistently.
The operational principle centers on the fact that many physiological processes manifest as visible or near-infrared changes detectable by appropriate sensors. Heart rate measurement through facial recognition relies on photoplethysmography, which detects minute color changes in facial skin corresponding to blood volume changes with each heartbeat. Specialized cameras capture these nearly imperceptible variations, and signal processing algorithms extract heart rate with remarkable accuracy. Blood pressure estimation employs similar principles but analyzes pulse wave velocity, the speed at which pressure waves travel through arteries, which correlates with arterial stiffness and blood pressure. Respiratory rate assessment tracks subtle chest movements or alternating color changes associated with breathing. Body temperature measurement uses infrared sensors that detect thermal radiation from exposed skin, particularly the face, which reflects core body temperature more reliably than extremities. Advanced mirrors incorporate full-body scanning capabilities, using depth sensors and body outline detection to calculate body mass index, track weight changes, and estimate body composition including muscle mass and fat distribution.
The most sophisticated smart mirror systems integrate multiple measurement modalities into comprehensive health assessments that would require several separate devices using traditional approaches. Skin analysis represents one of the most promising applications, where dermatological assessment through high-resolution imaging and computer vision algorithms can detect suspicious moles warranting professional evaluation, track skin condition changes over time, identify signs of dehydration or inflammation, and even estimate sun damage and skin age. Some mirror concepts incorporate posture analysis, using skeletal tracking algorithms to identify postural deviations that might contribute to back pain or other musculoskeletal problems, then providing corrective recommendations through visual overlays or voice guidance. More experimental features under development include eye health assessment through pupil examination, cardiovascular risk estimation from facial feature analysis, and stress level evaluation based on micro-expressions and facial tension patterns.
The user experience with smart mirrors emphasizes convenience and integration into existing daily routines. Most systems require only that users stand in front of the mirror for a brief period, typically less than one minute, while maintaining a relatively still position. The mirror might provide visual or audio cues to ensure proper positioning for optimal measurements. Some systems incorporate voice commands for hands-free operation, allowing users to request specific measurements or historical data without physical interaction. Results appear on the mirror display immediately, often with color-coded indicators showing whether measurements fall within healthy ranges. Many smart mirrors connect to smartphone applications where users can review historical trends, receive personalized health recommendations, set goals, and share data with healthcare providers. The integration with existing bathroom mirrors means the technology occupies no additional space, a significant advantage in homes where counter and wall space are limited.
However, smart health mirrors face significant technical challenges that have delayed widespread commercial availability and limited current accuracy compared to clinical measurements. Lighting conditions dramatically affect measurement reliability, with results varying based on ambient light color temperature, intensity, and directionality. Most current systems work best under consistent lighting conditions, which may require specific installation considerations or limiting measurements to particular times of day. Distance from the mirror affects accuracy, requiring users to stand within a specified range for reliable results. Skin tone variation influences optical measurements, with darker skin presenting particular challenges for photoplethysmography-based techniques that rely on detecting subtle color changes. Movement artifacts from breathing or involuntary movements can corrupt measurements, requiring sophisticated algorithms to filter noise from signal. Environmental factors including room temperature and humidity may affect thermal measurements and overall system performance.
The accuracy question remains central to evaluating smart mirror technology. Current research suggests that heart rate measurements from facial photoplethysmography achieve correlation coefficients above 0.9 compared to reference electrocardiogram measurements under controlled conditions, but accuracy degrades in real-world settings with variable lighting and user movement. Blood pressure estimation remains considerably less reliable, with errors often exceeding 10-15 mmHg for systolic pressure and 8-10 mmHg for diastolic pressure, accuracy levels insufficient for clinical blood pressure management. Body temperature measurements show reasonable accuracy for detecting fevers but may not match precision thermometer measurements. Skin analysis capabilities continue improving as training datasets expand and algorithms advance, but dermatologists caution that remote visual assessment cannot replace professional evaluation for suspicious lesions. The fundamental limitation stems from attempting to infer internal physiological states from external observations, a mathematically challenging inverse problem where multiple internal conditions might produce identical external appearances.
Regulatory agencies have approached smart mirrors cautiously, generally treating them as general wellness products rather than medical devices provided they avoid making diagnostic or treatment claims. This regulatory positioning allows innovation to proceed without burdensome approval processes but limits the health claims manufacturers can make. The regulatory framework surrounding health monitoring devices continues evolving to balance innovation with consumer protection. Recent FDA digital health guidance clarifications have helped manufacturers understand when their wellness products require formal clearance versus when they can operate under enforcement discretion. These updates address the rapid technological advancement in consumer health devices while maintaining safety standards. Smart mirrors marketed for “wellness monitoring” or “health awareness” occupy different regulatory territory than devices claiming to “diagnose disease” or “measure blood pressure for hypertension management.” This distinction affects not only regulatory requirements but also liability exposure and insurance reimbursement eligibility. The regulatory landscape continues evolving as technology improves and clinical evidence accumulates. Some manufacturers pursue regulatory clearance for specific measurements, particularly if they achieve clinical-grade accuracy and target populations with specific health conditions. This dual-track approach allows basic wellness features to reach consumers quickly while more ambitious diagnostic capabilities undergo rigorous validation.
The current smart mirror market in 2026 consists primarily of high-end prototypes and limited commercial offerings rather than mass-market products. Several major consumer electronics manufacturers have demonstrated concept devices at industry events, generating significant media attention and consumer interest but few actual products available for purchase. The technical challenges, regulatory considerations, and high development costs have slowed commercialization. Early commercial offerings typically cost between eight hundred and two thousand dollars, positioning them as premium products for early adopters and affluent health-conscious consumers rather than mainstream household items. This pricing reflects not only the sophisticated sensor packages and computing requirements but also limited production volumes that prevent economies of scale. As technology matures and production scales increase, prices should decline, potentially reaching mainstream affordability within three to five years.
Wearable Technology: Continuous Health Tracking
Wearable health technology has achieved what smart mirrors and at-home lab tests cannot: continuous monitoring throughout daily life, capturing the dynamic patterns and variations that tell richer health stories than isolated measurements. The evolution of wearables from simple step counters to sophisticated health monitoring platforms represents one of the most successful consumer health technology transformations. By 2026, over two hundred million people worldwide wore some form of health tracking device, generating billions of data points daily about physical activity, heart function, sleep quality, and numerous other physiological parameters. This massive deployment created the largest distributed health monitoring network in human history, fundamentally changing how individuals and healthcare systems approach preventive medicine and chronic disease management. The continuous nature of wearable monitoring addresses a fundamental limitation of traditional healthcare: the fact that health assessments typically occur during brief appointments that capture only momentary snapshots of physiological function, missing the variations and patterns that develop between visits.
The technological foundation of modern wearables combines multiple sensor types including accelerometers that measure motion and orientation, optical heart rate sensors using photoplethysmography, electrodes for electrical signals, temperature sensors, and increasingly sophisticated additions like bioimpedance sensors for body composition analysis and even chemical sensors for sweat analysis. Professional engineering organizations have extensively documented the technological advancements enabling sophisticated health monitoring. IEEE wearable biosensors research demonstrates how integration of artificial intelligence with nanotechnology and Internet of Medical Things creates precision care capabilities that were impossible just a few years ago. These sensors operate continuously or at frequent intervals, accumulating massive datasets that capture not just absolute values but also patterns, trends, and contextual relationships. Heart rate monitoring illustrates this advantage clearly. A single heart rate measurement taken during a doctor’s visit reveals limited information, influenced by anxiety, activity immediately before the appointment, and time of day. Continuous heart rate monitoring from a wearable device captures resting heart rate across different sleep stages, heart rate variability indicating autonomic nervous system function, exercise heart rate response and recovery patterns, and detection of irregular rhythms like atrial fibrillation that occur intermittently rather than constantly.
The sophistication of wearable algorithms has advanced dramatically, applying artificial intelligence and machine learning to extract meaningful health insights from raw sensor data. Sleep tracking exemplifies this progression. Early fitness trackers estimated sleep duration based solely on movement, essentially detecting periods of stillness. Modern wearables combine accelerometer data with heart rate patterns, heart rate variability, respiratory rate derived from subtle chest movements detected through accelerometer, and skin temperature to identify different sleep stages including light sleep, deep sleep, and REM sleep with accuracy approaching clinical polysomnography studies. The algorithms learn individual patterns over time, improving personalized accuracy and enabling detection of deviations from normal sleep architecture that might indicate health problems or lifestyle factors affecting sleep quality. Similar advancement occurred in activity recognition, where sophisticated algorithms now automatically identify specific exercise types including running, cycling, swimming, strength training, and yoga, calculating appropriate metrics for each activity without requiring manual input.
Advanced health features have transformed wearables from fitness accessories into legitimate health monitoring tools. Electrocardiogram capability appeared in premium smartwatches several years ago, enabling users to capture single-lead ECG readings by touching the watch crown with a finger, creating an electrical circuit through the body. While this simplified ECG cannot match the diagnostic power of a clinical twelve-lead ECG, it reliably detects atrial fibrillation, the irregular heart rhythm affecting millions and significantly increasing stroke risk. Multiple published studies have validated wearable ECG accuracy for atrial fibrillation detection, with sensitivity and specificity exceeding ninety-five percent compared to physician interpretation of simultaneous clinical ECG recordings. This capability has genuine clinical utility, enabling opportunistic screening during daily activities that might catch intermittent arrhythmias missed during brief medical appointments. Blood oxygen saturation monitoring through pulse oximetry became standard in many wearables, particularly valuable during the COVID-19 pandemic for detecting respiratory compromise before symptoms became severe.
The continuous monitoring paradigm enables several unique applications impossible with other monitoring approaches. Trend analysis over weeks or months reveals patterns that might predict health problems before symptoms appear. Gradually increasing resting heart rate might indicate developing illness, inadequate recovery from training, or emerging cardiac problems. Progressive decline in heart rate variability often precedes illness or indicates chronic stress affecting health. Sleep duration and quality trends correlate with numerous health outcomes, and deterioration often precedes other problems. Menstrual cycle tracking through temperature sensing and self-reported symptoms helps women understand their cycles, optimize conception timing, or detect irregularities warranting medical evaluation. Medication adherence and effectiveness monitoring through activity patterns and vital sign changes provide objective feedback about whether treatments are working. Falls detection through accelerometer and gyroscope data can automatically alert emergency contacts if an elderly person experiences a serious fall, potentially saving lives through faster response.
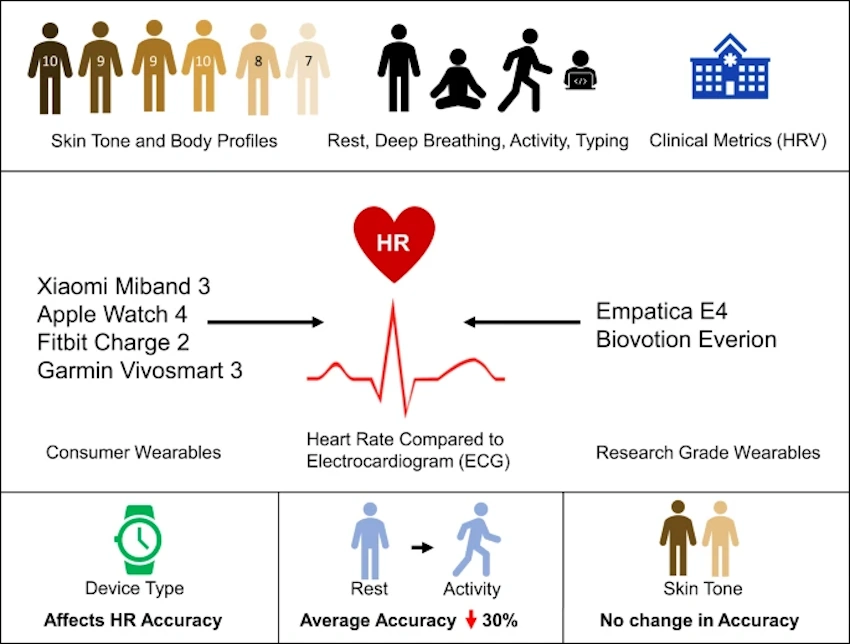
The accuracy of wearable measurements varies considerably across different parameters and device quality. Heart rate monitoring during rest and moderate exercise achieves excellent accuracy, typically within five to ten beats per minute compared to chest strap heart rate monitors or ECG, sufficient for most fitness and general health monitoring purposes. Accuracy degrades during intense exercise, particularly activities involving significant arm movement that creates motion artifacts interfering with optical heart rate detection. Step counting accuracy generally ranges from eighty-five to ninety-five percent under normal walking conditions but struggles with non-standard movements or when devices are not worn on the typical wrist location. Sleep stage detection shows reasonable overall accuracy but individual stage identification may vary, with algorithms performing better at distinguishing wake from sleep than differentiating between light sleep and deep sleep. Blood oxygen saturation measurements perform adequately for detecting significant hypoxemia but show more error than clinical pulse oximeters, particularly in individuals with darker skin tones where optical measurements face greater challenges.
Blood pressure measurement represents a frontier where wearable technology has struggled to achieve clinical accuracy. Several approaches have been attempted including pulse transit time methods that analyze the delay between heart electrical signals and arterial pressure waves detected in the wrist, and oscillometric methods adapted to wrist-worn form factors. However, wrist blood pressure measurements face inherent challenges because blood pressure varies with arm position relative to heart level, and wrist arteries are smaller and more easily compressed than upper arm arteries used in standard blood pressure cuffs. Most wearable blood pressure measurements require frequent calibration against traditional cuff measurements and show accuracy inferior to upper arm devices. Continuous glucose monitoring represents another area where wearable approaches show promise but face technical hurdles. Current continuous glucose monitors require sensor insertion under the skin, technically not non-invasive though far less burdensome than finger-stick testing. Truly non-invasive glucose measurement through optical spectroscopy or other approaches has been a holy grail of diabetes technology for decades but remains elusive due to the extremely small glucose signal compared to confounding factors.
The data ecosystem surrounding wearables has become as important as the devices themselves. Most wearables connect to smartphone applications that visualize data, provide coaching, enable social features for motivation, and increasingly integrate with healthcare systems. Some platforms allow data export to electronic health records, enabling physicians to review weeks or months of continuous data rather than relying on patient recollection or brief in-office measurements. Third-party applications can access wearable data through standardized APIs, creating ecosystems where specialized coaching, analysis, or research applications leverage the monitoring platform. The data aggregation across millions of users has enabled unprecedented population health research, identifying relationships between activity patterns, sleep habits, heart rate characteristics, and various health outcomes that would be impossible to study through traditional clinical research approaches. Privacy protections around this sensitive health data remain critical but often inadequate, with many wearable companies retaining broad rights to aggregate and analyze user data for research and commercial purposes.
At-Home Lab Tests: Deep Health Insights
While smart mirrors and wearables assess external manifestations of health and physiological signals accessible through skin contact, at-home lab tests penetrate beneath the surface to analyze the biochemical markers that reveal metabolic function, hormone balance, organ health, genetic predispositions, and disease presence. Blood, saliva, and urine contain thousands of measurable substances that reflect the body’s internal state with precision and specificity unattainable through external monitoring. A blood glucose measurement reveals current carbohydrate metabolism status. Hemoglobin A1C indicates average blood sugar control over the previous three months, providing critical information for diabetes management. Thyroid hormones determine metabolic rate and energy levels. Testosterone and estrogen affect everything from mood to muscle mass to bone density. Vitamin D influences bone health and immune function. C-reactive protein and other inflammatory markers signal chronic inflammation linked to cardiovascular disease and numerous other conditions. The democratization of lab testing through at-home collection kits has made this deep physiological insight accessible without requiring doctor’s orders, insurance approval, or clinic visits.
The at-home testing process typically begins with ordering a kit online after selecting desired tests from a menu ranging from focused panels measuring specific biomarkers to comprehensive metabolic assessments analyzing dozens of parameters. The kit arrives by mail containing collection supplies such as lancets for finger-stick blood samples, collection tubes, preservatives if needed, instructions, and prepaid shipping materials. Collection procedures vary by test type. Blood spot tests require pricking a finger with a lancet and squeezing drops of blood onto filter paper cards that are dried and mailed to the laboratory. Some tests require liquid blood collected in small tubes, achieved through multiple finger pricks or small collection devices. Saliva tests involve passive drool or cheek swab collection. Urine tests require collecting sample in a cup and transferring it to a preservation container. After collection, samples are packaged according to instructions and mailed to the testing laboratory using the provided shipping materials. The laboratory processes samples using the same instrumentation and methodologies as clinical laboratories, analyzing biomarker concentrations through techniques like immunoassays, mass spectrometry, or genetic sequencing.
Results typically become available within three to ten days after the laboratory receives samples, accessible through secure online portals or smartphone applications. The presentation format varies across companies but generally includes measured values, reference ranges indicating normal levels, and often interpretation guidance explaining what the results mean. More sophisticated platforms provide personalized recommendations based on results, suggesting dietary changes, supplements, lifestyle modifications, or medical consultation for abnormal findings. Some services include access to healthcare professionals for result interpretation, either through asynchronous messaging, scheduled phone consultations, or telemedicine video visits. This added service addresses a significant concern about at-home testing: that consumers may misinterpret results or fail to recognize when medical evaluation is necessary. The boundary between consumer lab testing and medical care remains somewhat ambiguous, with testing companies generally disclaiming diagnosis or treatment while providing information that inherently influences health decisions.
The range of tests available through at-home channels has expanded dramatically, now encompassing most common screening tests and many specialized assessments previously available only through healthcare providers. Lipid panels measuring cholesterol and triglycerides form a cornerstone of cardiovascular risk assessment. Comprehensive metabolic panels assess kidney function, liver enzymes, blood sugar, and electrolyte balance. Hormone panels measure sex hormones including testosterone, estrogen, progesterone, and DHEA, valuable for evaluating fertility, menopause symptoms, or hormone imbalance symptoms. Thyroid testing includes TSH, free T4, and free T3 to assess thyroid function. Vitamin and mineral testing measures vitamin D, vitamin B12, iron, magnesium, and other essential nutrients. Inflammatory marker testing including high-sensitivity C-reactive protein and homocysteine provides cardiovascular disease risk information. Food sensitivity testing identifies immune reactions to specific foods, though interpretation of these results remains somewhat controversial. Genetic testing offers insights into ancestry, disease predispositions, medication metabolism, and traits, though the clinical utility varies considerably across different genetic findings.
Advanced testing options continue expanding. Microbiome analysis examines the bacterial populations inhabiting the gut, providing information about digestive health and potentially broader health implications, though the practical utility of microbiome testing remains debated within the medical community. Heavy metal testing measures toxic elements like lead, mercury, and cadmium that may accumulate from environmental exposures. Omega-3 index testing assesses the percentage of red blood cell fatty acids comprised of EPA and DHA, biomarkers associated with cardiovascular health and anti-inflammatory status. Hormone metabolite testing provides more detailed information about how the body processes and eliminates hormones, valued by functional medicine practitioners though not typically part of conventional medical assessment. Cancer screening tests including liquid biopsies that analyze circulating tumor DNA represent an emerging frontier, with the potential to detect cancers years before symptoms appear, though sensitivity and specificity require further validation before becoming standard screening tools.
The accuracy of at-home lab tests depends critically on proper sample collection and handling. Blood spot tests collected from finger pricks may show slightly different results than venous blood draws due to capillary versus venous blood composition differences and potential contamination from tissue fluid. Sample degradation during mailing can affect results if samples are not properly preserved or if transit takes too long. Collection technique matters enormously, with inadequate blood samples leading to insufficient sample errors or contaminated specimens producing spurious results. Despite these challenges, most at-home tests show good correlation with clinical laboratory results when samples are collected and handled properly. Multiple studies have validated specific at-home tests against clinical laboratory results, generally finding agreement within acceptable clinical ranges for most analytes. Laboratory accreditation and quality control procedures at the receiving facilities play crucial roles in ensuring accurate results. Reputable at-home testing companies use laboratories certified under the Clinical Laboratory Improvement Amendments program, the federal standards that regulate all clinical laboratories in the United States.
The interpretation challenge represents perhaps the most significant concern surrounding at-home lab testing. Laboratory values exist along continua rather than representing simple normal versus abnormal categories, and interpreting whether a particular value warrants concern requires consideration of clinical context, symptoms, other test results, medical history, and individual risk factors that algorithms and written explanations cannot fully capture. Reference ranges provided with results represent statistical distributions from healthy populations but may not represent optimal ranges for an individual. Some values naturally vary based on age, sex, ethnicity, time of day, recent meals, hydration status, and other factors. A borderline abnormal result might represent normal variation, testing error, or the early stages of a developing problem. The appropriate response to borderline results is often observation and repeat testing rather than immediate intervention, but anxious consumers may seek unnecessary medical evaluation or self-treat with supplements that might be inappropriate or even harmful.
Accuracy and Reliability Comparison
Comparing accuracy across smart mirrors, wearables, and at-home lab tests requires understanding that each technology measures fundamentally different types of health information using different methodologies, making direct comparison challenging. The question is not which technology is most accurate in absolute terms but rather which achieves sufficient accuracy for its intended purpose and target measurements. Clinical-grade accuracy represents the gold standard, defined as the accuracy achieved by medical devices used in clinical settings under controlled conditions by trained professionals. Consumer health technologies rarely match clinical-grade accuracy but may achieve adequate accuracy for screening, trend monitoring, or general health awareness purposes even when individual measurements show more variability than clinical methods. The practical question becomes whether the accuracy achieved enables users to make better health decisions and improve health outcomes compared to having no monitoring at all.
Heart rate monitoring serves as a useful case study because all three technology types can measure it, enabling direct comparison. Clinical ECG provides the reference standard with essentially perfect accuracy. Medical-grade pulse oximeters and chest strap heart rate monitors achieve accuracy within one to two beats per minute of ECG. Wearable optical heart rate monitors during rest typically achieve accuracy within five to ten beats per minute compared to ECG, adequate for most fitness and general health purposes but insufficient for medical diagnosis. Smart mirror heart rate monitoring through facial photoplethysmography shows similar accuracy to wearable optical sensors under optimal conditions but greater variability under real-world conditions with variable lighting and user positioning. Laboratory tests do not measure heart rate, though some biomarkers like troponin indicate heart muscle damage and natriuretic peptides reflect heart failure severity. The accuracy hierarchy clearly places clinical measurements at the top, consumer wearables in the middle with acceptable accuracy for non-medical purposes, and smart mirrors showing promise but requiring further development for reliability.
Blood pressure comparison reveals larger accuracy gaps between consumer technologies and clinical measurements. Clinical upper arm cuff measurements performed properly represent the standard, with automated oscillometric devices showing excellent agreement with mercury sphygmomanometer measurements. Wrist blood pressure monitors show reduced accuracy compared to upper arm measurements, with systematic differences often exceeding ten mmHg that stem from hydrostatic pressure differences when the wrist is not positioned at heart level and differences in arterial characteristics between wrist and upper arm. Wearable blood pressure monitoring through pulse wave analysis or pulse transit time methods remains experimental, generally showing unacceptable inaccuracy compared to cuff measurements, with errors often exceeding fifteen mmHg for systolic pressure. Smart mirror blood pressure estimation through photoplethysmography analysis faces similar challenges and generally achieves insufficient accuracy for clinical blood pressure management. Laboratory tests can measure biomarkers related to blood pressure regulation like renin and aldosterone but do not directly measure blood pressure. For blood pressure monitoring, clinical measurements remain clearly superior, with validated home blood pressure monitors providing an acceptable middle ground, while smart mirrors and most wearables lack sufficient accuracy for reliable blood pressure assessment.
Biochemical marker measurement strongly favors laboratory testing, as this represents information inaccessible to external sensors or wearable devices. Glucose represents the most extensively studied analyte given the large diabetes population requiring glucose monitoring. Clinical laboratory glucose measurements from venous blood drawn under fasting conditions represent the gold standard with excellent accuracy and precision. Continuous glucose monitors inserted under the skin generally achieve mean absolute relative difference of eight to twelve percent compared to venous glucose measurements, accuracy considered acceptable for diabetes management though not perfect. Finger-stick glucose meters show similar accuracy. At-home lab tests using blood spot samples dried on filter paper cards generally achieve accuracy within fifteen percent of venous samples when properly collected, adequate for screening purposes though potentially showing more variability than fresh liquid blood. Smart mirrors and standard wearables cannot measure glucose non-invasively, representing a fundamental capability gap. For metabolic assessment, hormone measurement, nutritional status evaluation, and most disease biomarker testing, laboratory tests remain the only viable option among the three technology categories.
Sleep monitoring comparison highlights how different technologies provide complementary rather than competing information. Clinical polysomnography in a sleep laboratory represents the gold standard, using multiple sensors including EEG brain wave monitoring, eye movement tracking, muscle tone assessment, heart rhythm analysis, respiratory effort measurement, and blood oxygen monitoring to comprehensively assess sleep architecture. This comprehensive assessment cannot be replicated by consumer devices. Wearable sleep tracking using accelerometer movement detection, heart rate patterns, and heart rate variability analysis achieves reasonable accuracy for total sleep time and broad wake versus sleep classification, with studies showing seventy-five to eighty-five percent agreement with polysomnography for sleep stage identification. The accuracy suffices for general sleep awareness and detecting major sleep problems but misses subtleties that clinical studies would identify. Smart mirrors do not track sleep directly, though morning measurements might detect signs of poor sleep like elevated resting heart rate or physical appearance changes. Laboratory tests can measure melatonin levels and other biomarkers related to circadian rhythm function but provide only indirect sleep assessment. For practical sleep monitoring, wearables dominate this application, with clinical polysomnography reserved for diagnosing specific sleep disorders when wearable data suggests problems.
The reliability dimension involves consistency of measurements across repeated tests under similar conditions. Laboratory tests generally show excellent reliability when samples are properly collected and handled, with coefficients of variation typically below five to ten percent for most analytes. Wearable measurements show variable reliability depending on the parameter and conditions. Heart rate measurements show good test-retest reliability during rest but more variability during exercise. Step counting reliability depends on activity type and device placement. Sleep stage identification shows moderate reliability, with night-to-night variations stemming partly from genuine sleep differences and partly from measurement variability. Smart mirror reliability remains less well characterized given limited deployment but appears sensitive to environmental conditions including lighting and user positioning. The reliability of all consumer devices tends to be better for relative changes over time within an individual than for absolute values compared across different individuals or different measurement conditions.
Cost Analysis and Value Assessment
The financial investment required for health monitoring varies dramatically across technologies, from under fifty dollars for basic fitness trackers to thousands of dollars for comprehensive monitoring systems, creating important questions about cost-effectiveness and value. Understanding the total cost of ownership requires looking beyond initial purchase prices to include ongoing costs, the value of information provided, potential healthcare savings from early problem detection, and the opportunity cost of money spent on monitoring versus other health investments. The assessment becomes personal rather than universal, as different individuals derive different value from the same technology based on their health status, health goals, monitoring preferences, and whether they actually use the devices consistently over time. A sophisticated health monitoring system sitting unused in a drawer provides zero value regardless of its theoretical capabilities, while a simple device used consistently might deliver substantial health benefits despite limited sophistication.
Wearable technology presents the broadest price range, from basic fitness trackers available for thirty to fifty dollars to premium smartwatches costing five hundred to eight hundred dollars. The price differences reflect varying sensor packages, build quality, brand positioning, and feature sets. Basic fitness trackers typically provide step counting, sleep tracking, basic heart rate monitoring, and smartphone notifications. Mid-range options around one hundred to three hundred dollars add more sophisticated heart rate analysis, swim-proof designs, built-in GPS for outdoor activity tracking without phone, music storage, and extended battery life. Premium smartwatches incorporate all these features plus cellular connectivity allowing phone-free operation, electrocardiogram capability, blood oxygen monitoring, advanced health algorithms, premium materials, and comprehensive app ecosystems. Beyond initial purchase costs, many wearables require charging every one to seven days depending on battery capacity and usage patterns, contributing minor electricity costs. Some advanced features require monthly subscriptions, typically five to fifteen dollars monthly, for personalized coaching, detailed health analysis, or data storage beyond basic periods. Replacement costs matter given that wearables typically last two to four years before battery degradation, physical wear, or obsolescence from improved models encourage replacement.
At-home lab testing presents a different cost structure, with per-test costs ranging from thirty dollars for basic single-marker tests to over three hundred dollars for comprehensive panels measuring dozens of analytes. Unlike device purchases representing one-time investments that enable unlimited measurements, lab tests involve recurring costs each time testing is performed. The appropriate testing frequency depends on what’s being monitored and why. Someone tracking thyroid function during medication adjustment might test every six to eight weeks. A person monitoring cholesterol response to dietary changes might test every three months. Athletes tracking biomarkers for training optimization might test monthly during intensive training periods. Athletic performance monitoring extends beyond simple activity tracking to encompass comprehensive nutritional optimization supporting training demands. Understanding how to support muscle development and recovery through targeted nutrition strategies enables athletes to maximize the performance insights gained from monitoring technologies. An individual simply establishing baseline health status might test once or twice yearly. Subscription models offered by some testing companies provide regular testing at scheduled intervals for reduced per-test costs, typically ranging from thirty to seventy dollars monthly depending on which tests are included. The cumulative annual costs for regular at-home lab testing can easily reach several hundred to over one thousand dollars for comprehensive monitoring, substantially exceeding wearable device costs but providing information wearables cannot access.
Smart health mirror costs remain somewhat speculative given limited commercial availability in early 2026, but announced pricing for near-future products ranges from eight hundred to two thousand dollars, positioning them as premium purchases requiring careful value justification. These prices reflect sophisticated sensor packages including multiple cameras, infrared sensors, depth sensors, and computing power for real-time image processing and artificial intelligence analysis. Installation costs might add several hundred dollars if professional mounting, electrical work, or specific lighting installations are required for optimal operation. Unlike wearables that require periodic replacement, mirrors should last many years, though technological obsolescence might encourage upgrades as capability improves. Ongoing costs may include software subscriptions for advanced features, analysis, or cloud storage, potentially adding five to fifteen dollars monthly though some manufacturers might include these services at no additional charge. The smart mirror value proposition centers on convenience and passive monitoring requiring no behavior change, but whether this convenience justifies the substantial initial investment remains an individual decision.
Shop on AliExpress via link: wholesale-smart-health-monitor
Healthcare cost savings represent potential financial benefits offsetting monitoring technology costs. Detecting health problems early, when they are more easily and affordably treated, can prevent expensive hospitalizations, emergency interventions, or chronic disease complications. A person whose wearable device detects atrial fibrillation enabling stroke prevention through anticoagulation treatment might avoid a devastating stroke costing hundreds of thousands in acute care and rehabilitation plus immeasurable personal costs. Comprehensive fitness and health monitoring extends beyond cardiovascular surveillance to encompass metabolic health, body composition changes, recovery adequacy, and sleep quality. Integrated approaches combining multiple monitoring modalities with evidence-based fitness principles create complete pictures enabling optimization across all health dimensions. Someone whose lab test reveals vitamin D deficiency or thyroid dysfunction might resolve fatigue and other symptoms through simple, inexpensive treatments rather than suffering unnecessarily or undergoing expensive diagnostic workups searching for causes. A smart mirror detecting skin cancer early might enable simple surgical removal rather than advanced cancer requiring chemotherapy. These scenarios represent legitimate potential value, though quantifying the probability and magnitude of cost savings for any particular individual remains difficult. Population-level studies suggest remote monitoring reduces hospitalizations for certain chronic conditions, but whether an individual realizes these savings depends on whether they actually have detectable problems, whether they take appropriate action on abnormal findings, and numerous other factors.
The value assessment ultimately requires considering both tangible financial metrics and intangible benefits that may matter more than dollars. Peace of mind from knowing your health status is being monitored might be worth substantial cost to someone with health anxiety or family history of serious disease. The motivation to maintain healthy behaviors provided by visible activity and health metrics might prevent weight gain or encourage exercise consistency worth far more than the device cost through long-term health impacts. Learning about your body’s responses to different foods, stress, sleep patterns, and activities provides knowledge enabling better self-care decisions throughout life. Social motivation from sharing goals and competing with friends might make exercise more enjoyable and sustainable. The convenience of avoiding doctor’s appointments for routine screening tests saves time worth money. Home-based health optimization requires appropriate equipment supporting consistent training and monitoring routines. The right exercise equipment selection enables individuals to maintain fitness habits that generate meaningful data through monitoring technologies while achieving their performance and health objectives. Conversely, false positives creating anxiety and spurring unnecessary medical evaluation represent intangible costs that monetary figures don’t capture. Obsessive health monitoring that creates unhealthy preoccupation with bodily functions might reduce quality of life despite appearing beneficial on paper.
Technology Integration and Data Ecosystem
The future of personal health monitoring lies not in any single technology but in the seamless integration of multiple complementary systems creating a comprehensive health data ecosystem. Smart mirrors provide daily checkpoint assessments. Wearables deliver continuous monitoring throughout daily activities. Lab tests reveal biochemical insights into internal function. Electronic health records maintained by healthcare providers contain medical history, diagnoses, medications, and professional assessments. Genetic information reveals inherited predispositions and medication response predictions. Environmental exposure data from air quality monitors, water testing, and lifestyle apps add context. Nutrition tracking applications record food intake and dietary patterns. Mental health applications monitor mood, stress levels, and cognitive function. The convergence of these data streams enables artificial intelligence systems to identify patterns, predict health trajectories, and provide personalized recommendations impossible from any single data source. Achieving this integrated vision requires overcoming substantial technical, regulatory, and privacy challenges that have limited progress but represent the clear trajectory of digital health evolution.
Data interoperability represents the fundamental technical challenge, requiring different systems using different data formats, measurement units, and communication protocols to exchange information seamlessly. Healthcare has historically suffered from poor interoperability, with different electronic health record systems unable to share patient information efficiently, diagnostic equipment storing data in proprietary formats, and consumer health devices operating in isolated silos where data remains locked within manufacturer-specific applications. Industry standards organizations have worked for years to develop interoperability frameworks like Fast Healthcare Interoperability Resources that define standard methods for exchanging healthcare data. These standards enable, in theory, any system to share data with any other compatible system regardless of manufacturer. Implementation lags considerably behind standard development, with many systems claiming standards compliance while implementing only partial functionality or adding proprietary extensions that limit true interoperability. Consumer health device manufacturers have particular incentive to maintain data silos that lock users into their ecosystems, preventing easy migration to competing products or services.
Privacy and security concerns intensify as health data aggregation increases. Individual data streams from wearables, lab tests, or smart mirrors contain sensitive information, but combining multiple streams creates comprehensive profiles revealing far more about individuals than any single source. The aggregated data might expose mental health conditions, substance use, sexual behavior, genetic disease risks, and other highly personal information that individuals might not choose to share even with close family members. Unauthorized access to this comprehensive health data through security breaches could enable identity theft, insurance discrimination, employment discrimination, targeted scams, blackmail, or simply embarrassing exposure of private health information. Different countries and regions have implemented varying privacy regulations addressing health data protection. The Health Insurance Portability and Accountability Act governs medical information in the United States but does not cover consumer health applications and devices not considered covered entities. More recent state privacy laws and international regulations like the General Data Protection Regulation provide broader protections but enforcement remains inconsistent. Many consumer health companies retain broad rights to use aggregated anonymous data for research and commercial purposes, with fine print privacy policies that few users read thoroughly.
The practical integration approach most users pursue involves selecting compatible devices within a single ecosystem, such as choosing a smartwatch, smart scale, and blood pressure monitor from the same manufacturer where data automatically synchronizes to a unified application. This approach sacrifices selecting the best individual device in each category for the convenience of integration, but the tradeoff often makes sense given the hassle of manually transferring data between incompatible systems. Some third-party platforms act as aggregators, connecting to multiple device manufacturers and health services to combine data from different sources into unified dashboards. These platforms typically require users to grant access permissions to their accounts with each connected service, raising additional security considerations but enabling broader integration. Healthcare providers increasingly offer patient portals where individuals can view their medical records, test results, and care plans, with some supporting the ability to share data from consumer health devices or upload lab results from at-home testing services.
Leading healthcare institutions are pioneering integration approaches that connect consumer health technologies with clinical care systems. Mayo Clinic digital health initiatives demonstrate how intelligent technologies embedded in electronic health records can predict patient needs and enable more personalized care delivery based on continuous monitoring data.
Artificial intelligence represents the technology enabling meaningful insights from integrated health data that human analysis cannot easily extract. Machine learning algorithms can identify subtle patterns across multiple data streams that predict health problems before symptoms appear. A person whose wearable shows declining heart rate variability, whose smart mirror detects subtle facial changes, whose at-home lab test reveals elevated inflammatory markers, and whose activity level has decreased might be developing an infection, cardiac problem, or other issue that no single data point would flag but the pattern reveals. Predictive algorithms trained on population health data can estimate disease risks based on comprehensive personal data, providing earlier and more accurate risk assessment than traditional methods considering limited factors. Personalization algorithms learn individual baselines and patterns, enabling detection of deviations that might be normal for the general population but abnormal for a particular person. Recommendation algorithms can suggest interventions personalized to individual characteristics, preferences, and goals based on evidence about what works for people with similar profiles.
However, algorithmic decision-making in healthcare raises concerns about transparency, bias, accountability, and the appropriate role of automated systems in decisions affecting health and wellbeing. Most commercial health algorithms operate as black boxes where users receive recommendations without insight into how the algorithm reached its conclusions or what data inputs most influenced the output. This opacity prevents users from meaningfully evaluating whether to trust algorithmic advice. Algorithmic bias can arise when training data does not represent diverse populations, leading to algorithms that work well for majority groups but poorly for minorities, women, elderly individuals, or others underrepresented in training datasets. The allocation of responsibility when algorithmic recommendations lead to adverse outcomes remains unclear, with manufacturers disclaiming responsibility while users lack the expertise to override algorithmic advice when it might be wrong. The balance between algorithmic assistance and human judgment in healthcare decisions continues evolving, with growing recognition that the optimal approach combines artificial intelligence capabilities with human oversight rather than replacing human decision-making entirely.
Future Trends and Emerging Technologies
The personal health monitoring landscape continues evolving rapidly, with numerous emerging technologies and capabilities poised to enhance, extend, or potentially supersede current approaches over the coming five to ten years. Understanding these trends helps anticipate how health monitoring might change and what new capabilities might become available. The trajectory points clearly toward greater sensor diversity measuring more physiological parameters, improved accuracy approaching clinical-grade measurements, deeper integration creating unified health data ecosystems, more sophisticated artificial intelligence providing increasingly personalized and predictive insights, and broader accessibility making advanced health monitoring affordable to larger populations worldwide. However, technical challenges, regulatory requirements, privacy concerns, and the need for rigorous validation to ensure safety and efficacy will moderate the pace at which promising technologies actually reach widespread deployment.
Non-invasive glucose monitoring represents one of the most anticipated breakthroughs, with the potential to transform diabetes management and enable broader metabolic monitoring for non-diabetic individuals. Current continuous glucose monitors require sensor insertion under the skin, remaining minimally invasive but representing a barrier to casual use by individuals without diabetes who might benefit from understanding their glucose responses to different foods and activities. Multiple companies and research teams are pursuing true non-invasive glucose measurement through various approaches including optical spectroscopy analyzing tissue absorption of specific light wavelengths, electromagnetic sensing detecting glucose effects on skin dielectric properties, and analysis of tears, sweat, or interstitial fluid without puncturing skin. Despite decades of research investment, reliable non-invasive glucose measurement remains elusive due to the extremely low glucose signal-to-noise ratio and confounding factors that influence measurements more than glucose itself. However, advances in sensors, algorithms, and artificial intelligence may finally overcome these obstacles, with several companies claiming to be nearing commercial products though skepticism remains warranted given the history of unfulfilled promises in this arena.
Advanced biofluid analysis represents another frontier, extending at-home testing beyond blood, saliva, and urine to analyze sweat, tears, interstitial fluid, and exhaled breath. Sweat contains numerous biomarkers reflecting hydration status, electrolyte balance, metabolic function, stress hormones, and drug levels, potentially enabling real-time monitoring during exercise or daily activities through wearable sweat sensors. Current research prototypes demonstrate feasibility but practical challenges including sufficient sweat generation, preventing contamination, maintaining sensor functionality over extended periods, and achieving reliable quantitative measurements remain. Tear analysis through smart contact lenses could monitor glucose, inflammatory markers, and drug levels while providing vision correction or augmented reality capabilities, with multiple companies pursuing this futuristic vision though significant technical and regulatory hurdles remain before commercial deployment. Breath analysis devices could detect specific volatile organic compounds indicating various diseases, infections, or metabolic states, functioning as non-invasive screening tools though commercial development has proceeded slowly despite promising research results.
Implantable and ingestible sensors may enable continuous monitoring of internal physiological parameters currently inaccessible through external devices or requiring invasive procedures. Small sensor capsules swallowed and excreted naturally could monitor gastrointestinal function, detect bleeding, measure internal temperature, or assess medication absorption as they transit the digestive system. Long-term implantable sensors about the size of a grain of rice could continuously monitor specific biomarkers in blood or tissue, wirelessly transmitting data to external receivers, enabling chronic disease monitoring without repeated blood draws. Cardiac monitoring implants smaller than current pacemakers could detect arrhythmias over years rather than weeks that wearable monitors capture. These invasive approaches face higher regulatory requirements, safety concerns, and patient acceptance barriers compared to external devices but offer monitoring capabilities impossible through non-invasive methods. The appropriate use cases likely focus on serious chronic diseases where the benefits clearly outweigh the risks and inconvenience rather than general wellness monitoring.
Artificial intelligence enhancement across all monitoring modalities represents perhaps the most transformative trend, as algorithms become more sophisticated at extracting health insights from raw sensor data and identifying patterns predicting future health events. Current health monitoring devices mostly perform relatively simple data processing, calculating basic metrics like average heart rate, step counts, or sleep duration. Advanced algorithms could analyze these same data streams to detect early signs of infections before fever develops, predict cardiac events hours or days before they occur, identify subtle gait changes indicating neurological problems, or recognize cognitive decline from changes in daily activity patterns. Federated learning approaches allow algorithms to improve through exposure to data from millions of users while preserving individual privacy by never centralizing raw data. The fundamental shift from descriptive monitoring reporting what happened to predictive analytics forecasting what might happen represents a paradigm change in personal health monitoring value. However, achieving reliable predictions requires enormous training datasets, careful validation to prevent false alarms eroding user trust, and regulatory frameworks ensuring safety of algorithmic recommendations.
Augmented reality and virtual reality integration could enhance health monitoring through visualization making abstract data tangible and understandable. Imagine viewing your circulatory system overlaid on your body through augmented reality glasses, with color-coded blood vessels indicating good circulation versus areas with restricted flow. Virtual reality environments could gamify physical therapy exercises, making rehabilitation engaging rather than tedious. Augmented reality guidance during at-home lab test collection could ensure proper technique reducing errors. Virtual health coaching through realistic avatars might improve adherence to recommendations compared to text-based suggestions. While these applications remain mostly conceptual in early 2026, the underlying technologies exist and integration into health monitoring seems inevitable as augmented reality and virtual reality devices become mainstream consumer products over the next decade.
Conclusion: Choosing Your Health Monitoring Strategy
The convergence of smart health mirrors, wearable devices, and at-home lab testing into the personal health monitoring landscape has created unprecedented opportunity for individuals to take control of their health through continuous assessment, early problem detection, and data-driven decision-making. Each technology brings unique strengths addressing different aspects of health monitoring while carrying distinct limitations preventing any single approach from providing comprehensive surveillance. The optimal personal health monitoring strategy in 2026 involves thoughtfully selecting and combining technologies matched to individual health goals, medical conditions, lifestyle preferences, budget constraints, and commitment to using monitoring tools consistently over time. The sophistication of available technologies has advanced dramatically, but the value realized depends ultimately on human factors including motivation, interpretation capability, and willingness to act on findings rather than merely accumulating data that sits unexamined or unheeded.
Smart health mirrors offer the compelling promise of passive health monitoring requiring minimal behavior change beyond standing in front of a mirror during daily routines. For individuals who dislike wearing devices or struggle with consistent wearable use, the mirror’s integration into existing habits represents a significant advantage. The convenience of receiving immediate health assessments without any active monitoring effort may encourage more consistent monitoring compared to technologies requiring conscious engagement. However, current smart mirrors remain expensive, availability is limited, accuracy lags behind clinical measurements for many parameters, and environmental sensitivity requires proper installation and usage conditions. The technology suits individuals willing to invest in cutting-edge health technology who value convenience and daily checkpoint monitoring but should not be considered a replacement for more established monitoring approaches given current maturity levels. As the technology improves and costs decline over the next three to five years, smart mirrors may become mainstream health monitoring tools, but early adoption in 2026 represents a premium investment for technology enthusiasts rather than a necessity for effective health monitoring.
Wearable devices have become the workhorse of personal health monitoring, offering the most mature technology with proven accuracy for continuous tracking of physical activity, heart rate, sleep, and increasingly sophisticated health metrics. The breadth of available options across price points makes wearables accessible to almost anyone interested in health monitoring, from basic fitness trackers costing less than fifty dollars to sophisticated smartwatches providing near-medical-grade capabilities. The continuous monitoring paradigm that captures patterns and trends throughout daily life provides health insights impossible through occasional measurements, making wearables particularly valuable for fitness optimization, sleep improvement, chronic disease monitoring, and general health awareness. The ecosystem of supporting applications, social features, and integration options creates comprehensive platforms extending far beyond simple data collection. However, wearables require consistent use to provide value, with devices languishing in drawers providing zero benefit regardless of their capabilities. Some individuals find constant device wearing uncomfortable, inconvenient, or anxiety-producing rather than empowering. The accuracy limitations for certain measurements like blood pressure and the inability to assess biochemical markers represent fundamental constraints that no amount of wearable sophistication can overcome.
At-home lab testing fills the critical capability gap by providing access to internal biochemical markers that reveal metabolic function, hormone balance, nutritional status, and disease presence invisible to external monitoring. The democratization of laboratory testing enables proactive health assessment without requiring doctor’s orders or insurance approval, empowering individuals to investigate symptoms, track biomarkers over time, and optimize health based on objective internal data. The accuracy of at-home tests has improved to near-clinical-laboratory levels when samples are properly collected, providing reliable information for health decisions. However, the per-test costs create a fundamentally different economic model than device purchases, with regular comprehensive testing potentially costing hundreds or thousands of dollars annually. The recurring cost makes at-home testing most appropriate for targeted purposes like monitoring specific health conditions, investigating symptoms, or periodic comprehensive assessment rather than casual continuous monitoring. The interpretation challenge requires either significant health literacy to understand results or access to healthcare professionals for guidance, and the temptation to over-test or respond inappropriately to borderline results represents a legitimate concern.
The integrated approach combining multiple monitoring modalities likely provides the most comprehensive health assessment for individuals serious about proactive health management. A basic wearable device providing activity tracking, heart rate monitoring, and sleep assessment serves as the foundation, offering continuous physiological surveillance at reasonable cost with proven value for health awareness and behavior motivation. Selecting appropriate monitoring devices requires understanding the capabilities and limitations of different fitness trackers and health monitoring wearables available in 2026. Comprehensive evaluations help consumers identify which devices provide the specific measurements and features most relevant to their personal health goals. Periodic at-home lab testing, perhaps quarterly or semiannually, adds biochemical insights into internal function that wearables cannot access, enabling detection of nutritional deficiencies, hormone imbalances, metabolic problems, or early disease markers. Smart mirrors, when they become more widely available and affordable, could supplement these tools by providing convenient daily vital sign checkpoints without additional effort. The combination creates a comprehensive monitoring system where external physiological measures, continuous behavioral tracking, and internal biochemical assessment together paint a complete picture of health status. The investment required for this integrated approach might range from a few hundred to over one thousand dollars initially plus several hundred dollars annually for ongoing lab testing, representing a significant but potentially justifiable expense for health-conscious individuals focused on longevity and disease prevention.
The ultimate question is not whether to adopt personal health monitoring technology but rather how to do so thoughtfully, avoiding both the extremes of obsessive health tracking that creates anxiety and reduces quality of life and the opposite extreme of ignoring available tools that might detect serious problems early. The appropriate balance varies individually based on current health status, family history, personal health goals, and psychological relationship with health information. Someone with multiple chronic diseases requiring careful management benefits immensely from comprehensive monitoring enabling optimization of treatments and early detection of complications. An athlete training seriously gains valuable insights about recovery, training load, and performance from wearables and periodic lab testing assessing biomarkers affecting performance. Competitive athletes require specialized nutritional strategies that general fitness guidance cannot address. Understanding the specific dietary requirements and timing protocols that optimize athletic performance enables proper interpretation of monitoring data and targeted interventions when biomarkers indicate suboptimal nutrition status. A generally healthy person with family history of heart disease might focus on wearables detecting cardiac irregularities and periodic lipid testing for cardiovascular risk assessment. Someone managing anxiety might benefit more from simplified monitoring avoiding overwhelming data that fuels health anxiety rather than reducing it.
Mental wellbeing profoundly affects how individuals approach and benefit from health monitoring technologies. Supporting cognitive function through proper nutrition enhances the ability to interpret health data meaningfully and make wise decisions based on monitoring insights rather than reacting emotionally to every fluctuation.
The health monitoring revolution continues accelerating, with technologies improving, costs declining, and capabilities expanding rapidly. The landscape five years from now will likely look dramatically different, with capabilities that seem futuristic today becoming commonplace and new technologies emerging that we can barely imagine now. Staying informed about these developments while maintaining healthy skepticism about marketing claims and unvalidated technologies represents the wise approach. The most important lesson from evaluating smart mirrors, wearables, and at-home lab tests is that technology serves only as a tool enabling better health decisions and behaviors, but it cannot replace fundamental health practices including balanced nutrition, regular exercise, adequate sleep, stress management, and strong social connections. The highest-tech health monitoring system in the world provides limited value if not accompanied by commitment to healthy living and willingness to act on the insights technology provides. The future of health is personal, data-driven, and empowered by technology, but ultimately successful health outcomes require human wisdom, discipline, and care that no device can provide.
Question 1: What are smart health mirrors and how do they work?
Answer 1: Smart health mirrors represent an innovative fusion of everyday bathroom fixtures with advanced health monitoring technology. These intelligent devices incorporate multiple sensors including cameras, infrared detectors, and depth sensors embedded within or around a mirror surface that appears normal to casual observation. When you stand in front of the mirror for a brief period, typically thirty to forty-five seconds, the integrated sensors actively scan your face and body while sophisticated algorithms analyze the captured data in real-time. The system employs photoplethysmography to detect subtle color changes in facial skin corresponding to blood flow patterns, enabling heart rate calculation. Blood pressure estimation relies on analyzing pulse wave velocity through similar optical techniques. Infrared sensors measure thermal radiation from exposed skin to assess body temperature. Advanced computer vision algorithms track respiratory rate by detecting chest movement and skin color variations associated with breathing. Some mirrors include body composition assessment using depth sensors that map body contours to estimate body mass index and fat distribution. The measurements appear on the mirror display within seconds, often accompanied by trend charts showing changes over time and personalized health recommendations based on detected patterns. Connection to smartphone applications enables detailed historical review and data sharing with healthcare providers.
Question 2: How accurate are wearable fitness trackers compared to clinical devices?
Answer 2: The accuracy of wearable fitness trackers has improved dramatically over the past decade, approaching but not quite reaching the precision of clinical medical devices. Heart rate monitoring represents one of the most accurate wearable measurements, with current optical sensors achieving correlation coefficients exceeding 0.95 compared to electrocardiogram reference measurements during rest and moderate exercise. However, accuracy decreases during vigorous exercise with significant arm movement, sometimes showing errors of ten to fifteen beats per minute. Step counting accuracy typically ranges from eighty-five to ninety-five percent under normal walking conditions, but struggles with non-standard movements or when devices are not worn on the wrist. Sleep tracking shows reasonable overall accuracy for total sleep time estimation, usually within thirty minutes of polysomnography measurements, but individual sleep stage identification shows more variability, with algorithms performing better at distinguishing wake from sleep than differentiating between light sleep and deep sleep. Optimizing sleep quality requires understanding multiple factors beyond simple duration tracking. Research comparing sleep adequacy with exercise timing reveals that both quantity and quality of rest profoundly influence recovery, body composition changes, and overall health outcomes measured through comprehensive monitoring approaches. Blood oxygen saturation measurements provide adequate screening for significant hypoxemia but show more error than clinical pulse oximeters, particularly in individuals with darker skin tones where optical measurement challenges are greater. Blood pressure remains the most problematic measurement, with wrist-based approaches showing errors often exceeding ten to fifteen mmHg compared to upper arm cuff measurements, accuracy insufficient for clinical blood pressure management. The key insight is that wearables excel at trend detection and relative changes over time rather than absolute measurements, making them valuable for continuous health awareness and pattern recognition while clinical devices remain superior when precise measurements are required for medical decisions.
Question 3: What health metrics can at-home lab tests measure reliably?
Answer 3: At-home laboratory testing has expanded dramatically to encompass most common screening tests and numerous specialized assessments previously available only through healthcare providers. Lipid panels measuring total cholesterol, LDL cholesterol, HDL cholesterol, and triglycerides achieve clinical-grade accuracy when samples are properly collected, providing critical cardiovascular risk assessment information. Hemoglobin A1C testing for diabetes management shows excellent reliability, with most at-home tests agreeing within 0.5 percentage points of clinical laboratory results. Thyroid function testing including TSH, free T4, and free T3 enables evaluation of metabolic rate and energy regulation. Comprehensive metabolic panels assess kidney function through creatinine and blood urea nitrogen measurements, liver health through enzyme tests, blood sugar control, and electrolyte balance. Hormone testing reliably measures testosterone, estrogen, progesterone, DHEA, and cortisol levels, valuable for evaluating fertility issues, menopause symptoms, and endocrine function. Vitamin and mineral testing accurately determines vitamin D, vitamin B12, folate, iron, ferritin, and magnesium status, identifying nutritional deficiencies that might impair health. Inflammatory marker testing including high-sensitivity C-reactive protein and homocysteine provides cardiovascular disease risk information. The key to reliability involves proper sample collection following instructions precisely, ensuring samples are not exposed to excessive heat during mailing, and using testing services that employ certified clinical laboratories. Most reputable at-home testing companies achieve accuracy within ten to fifteen percent of venous blood draw results, adequate for screening and monitoring purposes though physicians may prefer confirmation testing for critical medical decisions.
Question 4: Which health monitoring method provides the most comprehensive data?
Answer 4: No single health monitoring method provides comprehensive data across all aspects of health, making the integration of multiple complementary technologies the most thorough approach to personal health assessment. Wearable devices excel at continuous monitoring of external physiological signals including heart rate, heart rate variability, activity levels, sleep patterns, and in some cases blood oxygen saturation and electrocardiogram readings. This continuous surveillance captures dynamic patterns throughout daily life, revealing trends and variations invisible in occasional measurements. However, wearables cannot penetrate beneath the skin to assess biochemical markers that reveal metabolic function, organ health, nutritional status, or hormone balance. At-home laboratory tests fill this critical gap by analyzing blood, saliva, or urine samples to measure cholesterol, glucose, vitamins, hormones, inflammatory markers, and numerous other biomarkers that no external sensor can detect. These internal measurements provide insights into the body’s chemical processes that might appear normal externally but indicate developing problems at the cellular level. Smart health mirrors add another dimension by providing convenient daily vital sign assessments and visual monitoring for changes in skin condition, posture, and physical appearance that might indicate health issues. The most comprehensive monitoring strategy combines a wearable device for continuous physiological tracking, periodic at-home lab testing quarterly or semiannually for biochemical assessment, and potentially a smart mirror for daily checkpoint monitoring when the technology becomes more accessible. This integrated approach creates a complete picture incorporating external physiology, continuous behavior patterns, internal biochemistry, and visual assessment that together enable far more sophisticated health insights than any single technology could provide.
Question 5: Are smart health mirrors approved by regulatory authorities?
Answer 5: The regulatory status of smart health mirrors depends critically on how manufacturers position and market their products, specifically whether they make diagnostic claims or focus purely on wellness monitoring. In January 2026, regulatory agencies including the United States Food and Drug Administration issued updated guidance clarifying that devices intended solely for general wellness use and presenting low risk to users generally receive enforcement discretion, meaning they operate without requiring formal regulatory approval. Smart mirrors marketed for wellness awareness, such as tracking vital signs for general health consciousness without making disease diagnosis claims, typically fall under this general wellness category. However, mirrors making specific health measurements for disease diagnosis, treatment guidance, or medical decision-making constitute medical devices requiring regulatory clearance through pathways like 510(k) premarket notification demonstrating substantial equivalence to existing cleared devices. The distinction rests on intended use claims and the specificity of health assertions made in marketing materials. A mirror claiming to “provide awareness of your heart rate” faces minimal regulatory scrutiny, while one claiming to “diagnose atrial fibrillation” or “measure blood pressure for hypertension management” requires rigorous validation and clearance. Most smart mirrors currently in development or early commercialization focus on wellness positioning to avoid regulatory burdens and accelerate market entry, though some manufacturers are pursuing regulatory clearance for specific measurements like heart rate or body composition where they believe they can demonstrate sufficient accuracy. European regulatory frameworks operate somewhat differently under Medical Device Regulations but follow similar principles distinguishing wellness devices from medical devices based on intended use and risk classification.
Shop on AliExpress via link: https://s.click.aliexpress.com/e/_c2zv8sEJ
Question 6: How much do these health monitoring technologies typically cost?
Answer 6: The financial investment for personal health monitoring technologies spans a dramatic range, from minimal expenditure to thousands of dollars depending on sophistication level and monitoring objectives. Basic fitness trackers from reputable manufacturers start around thirty to fifty dollars, providing fundamental capabilities including step counting, sleep tracking, basic heart rate monitoring, and smartphone notifications adequate for casual health awareness and fitness motivation. Mid-range fitness trackers and smartwatches in the one hundred to three hundred dollar range add more sophisticated features including continuous heart rate monitoring, waterproof designs for swim tracking, built-in GPS for outdoor activities without phone, music storage, and more comprehensive health algorithms. Premium smartwatches from major technology companies cost between four hundred and eight hundred dollars, incorporating advanced health monitoring like electrocardiogram capability, blood oxygen measurement, cellular connectivity, premium materials, and comprehensive app ecosystems. Beyond initial purchase costs, some wearables require monthly subscriptions ranging from five to fifteen dollars for personalized coaching, detailed health analysis, or extended data storage. Smart health mirrors represent premium investments, with expected pricing between eight hundred and two thousand dollars when commercially available, reflecting sophisticated sensor packages and limited production volumes. At-home lab testing operates on a different economic model with per-test costs rather than upfront device investments. Individual tests range from thirty dollars for basic single-marker assays to over three hundred dollars for comprehensive panels measuring dozens of biomarkers. Subscription testing services offering regular scheduled testing cost approximately thirty to seventy dollars monthly. Someone pursuing comprehensive monitoring combining a quality wearable device, smart scale, and quarterly lab testing might invest four hundred to six hundred dollars initially plus three hundred to eight hundred dollars annually for ongoing lab tests and subscriptions.
Question 7: Can these technologies replace regular doctor visits?
Answer 7: Personal health monitoring technologies serve as powerful complements to professional medical care but cannot replace the comprehensive assessment, diagnostic expertise, and treatment guidance that physicians provide during clinical encounters. These consumer technologies excel at specific functions that enhance healthcare between appointments, including continuous monitoring of vital signs and activity patterns that reveal trends invisible during brief clinic visits, early warning detection of potential problems enabling timelier medical consultation, tracking chronic disease markers helping patients and providers optimize treatment effectiveness, and empowering patients with objective data that facilitates more informed discussions with healthcare providers. However, these devices face fundamental limitations preventing them from substituting for medical visits. They cannot perform physical examinations assessing findings like heart murmurs, lung sounds, abdominal masses, or joint abnormalities that require hands-on evaluation. They cannot provide definitive diagnoses that require integrating clinical history, physical findings, laboratory results, imaging studies, and medical expertise. They cannot prescribe medications, adjust treatment plans, or provide medical advice tailored to individual circumstances. The interpretation of monitoring data requires clinical context that algorithms cannot fully capture, and borderline abnormal results often need professional evaluation to determine appropriate response. Healthcare is increasingly evolving toward a collaborative model where personal monitoring technologies extend the reach of professional care by maintaining surveillance between appointments, enabling virtual check-ins that may reduce unnecessary office visits, and providing objective data that makes limited face-to-face time with providers more productive. The future involves partnership between technology-enabled patient self-monitoring and professional medical expertise rather than replacement of traditional care delivery models.
Question 8: What privacy concerns exist with health monitoring devices?
Answer 8: Privacy and security concerns surrounding personal health monitoring devices have intensified as these technologies collect increasingly detailed and sensitive physiological information. The primary concerns center around several key issues. First, data collection extent often exceeds user expectations, with devices capturing not only the primary health metrics advertised but also location data, usage patterns, and behavioral information that reveals intimate details about daily life. Second, data storage security remains variable across manufacturers, with inadequate encryption, weak authentication, or vulnerable cloud storage potentially exposing personal health information to unauthorized access through hacking or data breaches. Third, data sharing practices often involve selling or sharing aggregated user data with third parties including advertisers, insurers, data brokers, or research organizations, sometimes with limited transparency about these practices despite disclosure in lengthy privacy policies that few users read thoroughly. Fourth, the combination of data from multiple sources creates comprehensive profiles revealing far more about individuals than any single data stream, enabling inference of sensitive conditions like mental health status, substance use, sexual behavior, or genetic disease risks. Regulatory protections vary considerably across jurisdictions, with traditional medical privacy laws often not covering consumer health devices classified as wellness products rather than medical devices. Some manufacturers demonstrate strong privacy commitment through encryption, local data processing that minimizes cloud transmission, clear privacy policies, user control over data sharing, and explicit consent requirements before sharing data with third parties. Others show concerning practices including retroactive privacy policy changes that authorize new data uses without clear notification, inadequate security measures that have resulted in breaches exposing millions of user records, and opaque practices making it difficult for users to understand exactly what happens to their health data. Users should carefully review privacy policies before purchasing health monitoring devices, preferring manufacturers with strong security track records and transparent practices.
Question 9: How do these technologies help with chronic disease management?
Answer 9: Personal health monitoring technologies have transformed chronic disease management by enabling continuous surveillance outside clinical settings, early detection of deteriorating conditions, objective assessment of treatment effectiveness, and empowerment of patients as active participants in their care. The continuous monitoring paradigm represents a fundamental shift from periodic clinical assessments that capture only momentary snapshots to ongoing surveillance revealing patterns and trends over weeks or months. For cardiac patients, wearables provide continuous heart rate and heart rate variability monitoring that can detect arrhythmias like atrial fibrillation warranting medical intervention, track heart rate recovery after exercise indicating cardiovascular fitness trends, and measure activity levels providing objective feedback about physical conditioning. Diabetes management benefits enormously from continuous glucose monitoring enabling patients to understand glucose responses to different foods and activities, detect hyperglycemic or hypoglycemic episodes, optimize insulin dosing based on real-time data, and track hemoglobin A1C trends through at-home testing. Hypertension management improves through regular blood pressure monitoring using validated home devices, revealing patterns throughout the day that single office measurements miss, including white coat hypertension where anxiety in medical settings produces artificially elevated readings. Respiratory disease patients benefit from monitoring activity tolerance, sleep quality affected by breathing difficulties, and blood oxygen saturation that might indicate worsening respiratory function requiring medical attention. At-home laboratory testing enables regular monitoring of critical biomarkers without frequent clinic visits, such as kidney function tests for chronic kidney disease patients, liver enzyme monitoring for medication side effect surveillance, thyroid hormone levels during medication adjustment, and inflammatory markers indicating disease activity in conditions like rheumatoid arthritis. Smart mirrors could potentially detect subtle physical changes like skin color variations indicating circulation problems or edema suggesting heart failure decompensation. The critical benefit involves enabling early intervention when problems develop, rather than waiting until symptoms become severe enough to prompt medical visits or emergency situations.
Question 10: What does the future hold for personal health monitoring technology?
Answer 10: The future trajectory of personal health monitoring points toward increasingly sophisticated integration of artificial intelligence, expanded sensor capabilities measuring additional physiological parameters, seamless connectivity creating unified health data ecosystems, improved accuracy approaching clinical-grade measurements, and broader accessibility making advanced monitoring affordable to larger populations worldwide. Non-invasive glucose monitoring represents one of the most anticipated breakthroughs, with multiple companies pursuing optical, electromagnetic, and other approaches to measure blood sugar without skin penetration, potentially transforming diabetes management and enabling metabolic monitoring for non-diabetic individuals. Sweat, tear, and breath analysis may enable real-time biomarker monitoring during daily activities, detecting hydration status, stress hormones, metabolic markers, drug levels, and even volatile compounds indicating various diseases. Miniaturized sensors embedded in contact lenses, ingestible capsules, or tiny implants could continuously monitor internal physiological parameters currently inaccessible through external devices. Artificial intelligence enhancement will transform raw sensor data into sophisticated health insights, predicting health events hours or days before they occur, personalizing recommendations based on individual patterns learned over time, and identifying subtle changes indicating developing problems before symptoms appear. Integration between personal monitoring devices and healthcare systems will become seamless, with continuous data flowing directly into electronic health records enabling physicians to review weeks of objective data during appointments rather than relying on patient recollection. Augmented reality visualization might overlay health data onto the physical world, making abstract measurements tangible and understandable. Regulatory frameworks will continue evolving to balance innovation encouragement with safety assurance, potentially creating new regulatory pathways specifically for AI-enabled health monitoring that operates differently from traditional medical devices. The shift from episodic care delivery to continuous health surveillance represents perhaps the most fundamental transformation, moving healthcare from reactive treatment after problems develop to proactive prediction and prevention enabled by comprehensive continuous monitoring throughout life.
Articles related:
Tags
📧 Get More Articles Like This
Subscribe to receive product reviews and buying guides in your inbox!
We respect your privacy. Unsubscribe at any time.