Herbs That Strengthen the Nervous System: Ancient Wisdom Meets Modern Science

Table of Contents
- Introduction: The Crisis of Modern Nervous System Health
- Understanding Your Nervous System: More Than Just Nerves
- The Science Behind Herbs and Neurological Health
- Adaptogenic Herbs: Building Long-Term Resilience
- Nervine Herbs: Immediate Calming and Support
- Neuroprotective Herbs: Guarding Your Brain’s Future
- Traditional Medicine Systems and Nervous System Support
- How to Choose and Use Nervous System Herbs Safely
- Conclusion: Integrating Herbal Wisdom into Modern Life
Introduction: The Crisis of Modern Nervous System Health
Sarah’s hands trembled as she reached for her third cup of coffee that morning. The thirty-eight-year-old marketing executive had barely slept again, her mind racing through tomorrow’s presentation even as exhaustion pulled at every cell in her body. Her doctor had suggested anxiety medication, but something in Sarah wanted to understand why her nervous system had become so fragile in the first place. What she discovered changed everything about how she approached her health, leading her down an unexpected path into the world of medicinal herbs that had supported human nervous systems for thousands of years.
This story plays out millions of times across the modern world. Our nervous systems, designed for occasional acute stressors like fleeing predators or hunting food, now face relentless chronic activation from work deadlines, financial pressures, relationship conflicts, and the constant digital bombardment of information our brains never evolved to process. The statistics paint a sobering picture of the crisis. According to the National Institute of Mental Health, over forty million American adults experience anxiety disorders annually, while stress-related conditions cost the economy an estimated three hundred billion dollars in healthcare expenses and lost productivity. The World Health Organization reports that neurological disorders affect up to one billion people globally, with numbers rising as populations age and stress intensifies across societies.
Yet buried within this modern crisis lies ancient wisdom that contemporary science increasingly validates. Long before pharmaceutical companies synthesized molecules in laboratories, traditional healers across every continent identified specific plants that could calm frazzled nerves, sharpen dulled minds, and protect delicate brain tissue from the ravages of stress and aging. These botanical medicines worked through mechanisms science only recently began to understand, operating on principles that conventional Western medicine often overlooks. The herbs didn’t merely suppress symptoms like pharmaceutical drugs often do. Instead, they worked to restore balance to entire systems, addressing root causes rather than masking effects.
Research from leading neuroscience institutions has documented how traditional medicinal herbs contain complex phytochemical profiles that work synergistically to protect brain tissue. Studies examining neuroprotective herbs traditional medicines demonstrate these botanical compounds cross the blood-brain barrier to reduce oxidative stress, inhibit inflammatory cascades, and even promote neurogenesis in specific brain regions. The convergence of ancient herbal wisdom with contemporary neuroscience validates what traditional healers observed through millennia of clinical experience.
Before delving into the details of the article, watch this video which presents 10 herbs to repair nerves and promote calmness :
Recent research published in medical journals has confirmed what traditional practitioners knew through centuries of observation. Studies demonstrate that specific herbal compounds cross the blood-brain barrier to influence neurotransmitter synthesis, protect neurons from oxidative damage, reduce neuroinflammation, and even stimulate the growth of new brain cells through neurogenesis. These aren’t just folk remedies passed down through superstition. They represent sophisticated phytochemical interventions that target multiple pathways simultaneously, offering benefits that single-molecule drugs struggle to replicate without side effects.
The convergence of traditional herbal knowledge and modern neuroscience research has created unprecedented opportunities for anyone seeking to strengthen their nervous system naturally. We now understand the biochemical mechanisms behind why ashwagandha reduces cortisol levels, how bacopa monnieri enhances memory formation, and why compounds in certain mushrooms stimulate nerve growth factor production. This knowledge empowers informed choices about incorporating these powerful botanicals into comprehensive wellness strategies that support long-term neurological health.
The scientific validation of herbal neuroprotection continues expanding through rigorous research methodologies. Comprehensive reviews examining nutraceuticals in neurological disorders demonstrate how herbal compounds influence protein synthesis, prevent neuronal degradation, and provide multi-targeted therapeutic effects that pharmaceutical interventions struggle to replicate. These evidence-based findings provide the scientific foundation supporting traditional herbal approaches to nervous system wellness.
This comprehensive guide explores the most effective herbs for strengthening the nervous system, backed by both traditional use and contemporary scientific validation. We’ll examine adaptogenic herbs that build resilience against stress, nervine herbs that provide immediate calming relief, and neuroprotective botanicals that guard brain health for decades to come. More importantly, we’ll discuss how to use these herbs safely and effectively, understanding both their remarkable benefits and important precautions. The goal isn’t to replace necessary medical care but to reclaim the powerful tools nature provides for supporting optimal nervous system function throughout life.
Understanding Your Nervous System: More Than Just Nerves
Before diving into specific herbs and their applications, understanding how your nervous system actually functions proves essential for making informed decisions about herbal support. The nervous system represents far more than just the network of nerves threading through your body. It encompasses the intricate command center that coordinates every thought, movement, sensation, and automatic function keeping you alive. This biological marvel processes approximately eleven million bits of information every second, though conscious awareness handles only about forty bits. The rest operates beneath conscious perception, managing heart rate, breathing, digestion, immune responses, and countless other vital processes.
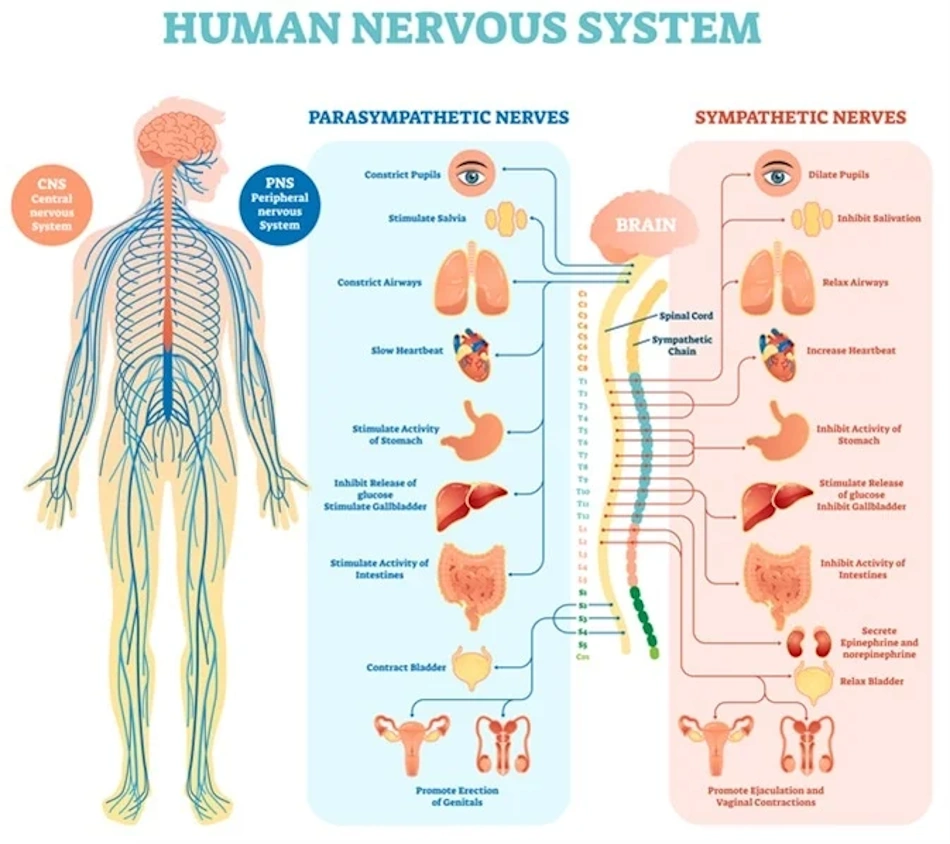
The nervous system divides into two major components that work in seamless coordination. The central nervous system consists of the brain and spinal cord, serving as the main processing center where information integrates and decisions form. Your brain alone contains approximately eighty-six billion neurons, each connecting to thousands of other neurons through synapses, creating a network of staggering complexity. The peripheral nervous system encompasses all nerves extending beyond the spinal cord, carrying sensory information inward and motor commands outward. These peripheral nerves transmit messages about temperature, pain, pressure, and position while simultaneously directing muscle movements and gland secretions.
Within the peripheral nervous system lies a critical subdivision called the autonomic nervous system, which regulates involuntary functions without conscious control. This autonomic system further divides into two branches that ideally maintain dynamic balance but often fall into chronic imbalance in modern life. The sympathetic nervous system activates the famous “fight or flight” response, releasing stress hormones, accelerating heart rate, dilating pupils, and diverting blood flow to muscles while temporarily shutting down non-essential functions like digestion. This response evolved for brief emergencies, not the prolonged activation that characterizes contemporary existence.
Understanding how chronic stress affects the central nervous system reveals why adaptogenic herbs prove so valuable for modern health challenges. Research documenting effects adaptogens on central nervous system shows these botanical medicines normalize stress response pathways, reduce sympathetic overactivation, and protect neurons from cortisol-induced damage. The adaptogenic mechanism of increasing non-specific resistance to stressors addresses the root cause of nervous system depletion rather than merely masking symptoms.
The parasympathetic nervous system provides the essential counterbalance, often called “rest and digest” mode. This branch slows heart rate, promotes digestion, stimulates healing processes, and allows the body to rebuild depleted resources. Optimal health requires flexible switching between these states based on actual needs, spending most time in parasympathetic dominance while maintaining the ability to activate sympathetic responses when genuine threats appear. Unfortunately, chronic stress locks many people into sustained sympathetic activation, exhausting the nervous system and creating cascading health problems throughout the body.
The nervous system communicates through both electrical signals traveling along nerve fibers and chemical messengers called neurotransmitters crossing synapses between neurons. These neurotransmitters include familiar names like serotonin, dopamine, GABA, glutamate, and norepinephrine, each playing specific roles in mood regulation, motivation, relaxation, excitation, and numerous other functions. The delicate balance between excitatory and inhibitory neurotransmitters determines whether you feel calm or anxious, focused or scattered, energized or depleted. Many herbs influence nervous system function precisely by modulating neurotransmitter production, receptor sensitivity, or degradation rates.
Government health agencies provide essential resources for understanding complementary approaches to nervous system health. The National Center for Complementary and Integrative Health offers evidence-based information traditional Chinese medicine practices including herbal interventions for neurological support, safety considerations, and research findings. These official resources help individuals make informed decisions about incorporating traditional medicine approaches into comprehensive wellness strategies under appropriate professional guidance.
Protecting nervous system health requires understanding its vulnerabilities. Neurons represent some of the longest-lived cells in your body, many lasting your entire lifetime since adult brains generate relatively few new neurons compared to other tissues. This longevity makes neurons particularly vulnerable to cumulative damage from oxidative stress, inflammation, toxin exposure, and nutrient deficiencies. Unlike skin cells that regenerate rapidly after injury, damaged neurons may never fully recover, making prevention through neuroprotection absolutely critical for maintaining cognitive function throughout the lifespan.
The blood-brain barrier adds another layer of complexity to nervous system support. This selective membrane protects the brain from potentially harmful substances circulating in the bloodstream while allowing essential nutrients to pass through. However, this protection also prevents many beneficial compounds from reaching brain tissue, limiting which supplements and herbs can directly influence central nervous system function. Effective nervous system herbs must contain compounds that either cross the blood-brain barrier or influence nervous function through peripheral mechanisms that ultimately affect central processing.
Modern neuroscience reveals that nervous system health extends far beyond preventing diseases like Alzheimer’s or Parkinson’s. The quality of nervous system function determines resilience to stress, emotional regulation capacity, cognitive performance, sleep quality, pain perception, and even immune system effectiveness. The gut-brain axis demonstrates how nervous system health interconnects with digestive function through the enteric nervous system, often called the “second brain.” This bidirectional communication explains why stress causes digestive problems and why gut inflammation contributes to anxiety and depression.
The Science Behind Herbs and Neurological Health
The intersection of traditional herbal medicine and modern neuroscience research has produced fascinating insights into how botanical compounds influence nervous system function at molecular levels. These discoveries validate centuries of traditional use while revealing mechanisms that earlier practitioners could only infer from observation. Understanding these scientific foundations helps explain why certain herbs consistently demonstrate effectiveness across diverse populations and conditions, while also highlighting important considerations for safe and effective use.
Herbal compounds influence nervous system health through multiple simultaneous mechanisms, distinguishing them from pharmaceutical drugs that typically target single pathways. This polypharmacy approach means herbs often produce broader benefits with fewer side effects than isolated synthetic molecules, though it also complicates research trying to identify “active ingredients.” Traditional herbalists understood this synergy intuitively, using whole plant preparations rather than extracting individual compounds. Modern research increasingly validates this approach, discovering that compounds within herbs work together in ways that enhance therapeutic effects beyond what isolated molecules achieve alone.
One primary mechanism involves direct influence on neurotransmitter systems. Herbs contain compounds that can increase neurotransmitter synthesis, prevent premature breakdown, modulate receptor sensitivity, or influence reuptake mechanisms. For example, compounds in St. John’s wort inhibit reuptake of serotonin, dopamine, and norepinephrine simultaneously, explaining its antidepressant effects. Herbs containing GABA precursors or compounds that enhance GABAergic activity produce calming effects by strengthening the nervous system’s primary inhibitory neurotransmitter. Other herbs influence acetylcholine metabolism, critical for memory formation and cognitive function.
Neuroprotection represents another crucial mechanism by which herbs support nervous system health. The brain consumes approximately twenty percent of the body’s oxygen despite representing only two percent of body weight, making it particularly vulnerable to oxidative stress as oxygen metabolism generates reactive free radicals. Herbs rich in antioxidant compounds like flavonoids, polyphenols, and terpenoids neutralize these free radicals before they damage delicate neuronal membranes and DNA. Studies published in neuroscience journals document how specific herbal antioxidants reduce markers of oxidative stress in brain tissue while improving cognitive performance measures.
Anti-inflammatory effects provide yet another pathway for herbal nervous system support. Chronic neuroinflammation, involving activation of brain immune cells called microglia and astrocytes, plays central roles in neurodegenerative diseases, depression, anxiety, and cognitive decline. Herbs containing compounds that inhibit inflammatory signaling molecules like NF-κB, TNF-α, and various interleukins reduce this damaging inflammation. Research shows these anti-inflammatory herbs not only protect existing neurons but may also create environments more favorable for neurogenesis, the birth of new neurons in specific brain regions.
The concept of adaptogenic action, while challenging for Western scientific frameworks to fully embrace, represents one of the most important ways certain herbs strengthen nervous systems. Adaptogens work by normalizing the hypothalamic-pituitary-adrenal axis, the complex hormonal system governing stress responses. Rather than simply suppressing or stimulating activity, adaptogens help this system respond appropriately to actual stressors while maintaining baseline function during rest periods. This bidirectional regulation explains why the same adaptogenic herb can calm an overstimulated nervous system while energizing a depleted one, adjusting effects based on individual needs.
Modern research has identified specific molecular targets for many traditional nervous system herbs. Ashwagandha contains withanolides that modulate cortisol receptor sensitivity and influence heat shock protein expression, protecting cells from stress damage. Bacopa monnieri’s bacosides enhance synaptic communication by upregulating proteins involved in neurotransmitter release while promoting dendrite branching that increases neuronal connectivity. Rhodiola rosea influences monoamine neurotransmitter levels through effects on enzyme activity while also protecting mitochondrial function in neurons, preserving cellular energy production under stress.
The bioavailability question remains central to understanding how herbs influence nervous system function. Not all beneficial compounds in herbs reach target tissues in concentrations sufficient to produce effects. Some herbal compounds require specific preparation methods like alcohol extraction or cooking to release active constituents from plant matrices. Others need cofactors present in whole food diets to enhance absorption. Fat-soluble compounds require dietary fats for optimal uptake. Traditional preparation methods often incorporated these considerations instinctively, while modern supplementation sometimes overlooks factors affecting absorption and biological activity.
Dosage and duration of use significantly impact herbal effectiveness for nervous system support. Unlike pharmaceutical drugs designed for immediate effects, many nervine and adaptogenic herbs require consistent use over weeks or months to produce optimal benefits. This delayed onset reflects their mechanism of gradually restoring balance rather than forcing immediate changes. Acute-acting nervines like valerian or passionflower provide relatively rapid effects within an hour or two, while adaptogens like ashwagandha typically require six to twelve weeks of daily use before full benefits manifest. Understanding these timelines helps set appropriate expectations and maintain consistency.
Adaptogenic Herbs: Building Long-Term Resilience
Adaptogenic herbs represent a special category of botanical medicines characterized by their ability to increase resistance to stress while normalizing physiological functions disrupted by chronic stressor exposure. The term “adaptogen” emerged from mid-twentieth-century Soviet research on substances that could enhance soldier performance under extreme conditions, though the herbs themselves had been used in traditional medicine systems for millennia. To qualify as true adaptogens, herbs must meet specific criteria including being non-toxic at normal doses, producing non-specific resistance to various stressors, and having normalizing effects regardless of initial dysfunction direction.
Ashwagandha stands as perhaps the most thoroughly researched adaptogenic herb for nervous system support, with over four thousand years of traditional use in Ayurvedic medicine backing modern clinical validation. Known botanically as Withania somnifera, this hardy shrub produces roots and berries containing powerful compounds called withanolides that exert multiple beneficial effects on stressed nervous systems. Clinical trials published in prestigious medical journals demonstrate that ashwagandha supplementation significantly reduces cortisol levels in chronically stressed individuals, sometimes by thirty percent or more, while simultaneously improving markers of anxiety and perceived stress.
The mechanisms by which ashwagandha strengthens nervous systems extend beyond simple cortisol reduction. Research reveals this herb influences GABA receptors, enhancing the calming effects of this primary inhibitory neurotransmitter. Withanolides also demonstrate neuroprotective properties, shielding neurons from oxidative damage and even promoting regeneration of nerve endings in animal studies. Human trials show improvements in memory, reaction time, and cognitive performance after several weeks of consistent use. The herb appears particularly beneficial for nervous exhaustion characterized by feeling “tired but wired,” where the sympathetic nervous system remains overactive despite physical exhaustion.
Shop on AliExpress via link: wholesale-ashwagandha-supplement
Rhodiola rosea, a flowering plant thriving in cold mountainous regions across Europe and Asia, represents another premier adaptogenic herb for nervous system resilience. Traditional use in Scandinavian and Russian folk medicine focused on enhancing physical endurance and mental clarity during harsh winters and demanding work. Modern research confirms rhodiola’s ability to combat mental and physical fatigue while improving cognitive function under stress. The herb contains active compounds including rosavins and salidrosides that influence serotonin, dopamine, and norepinephrine levels, supporting balanced mood and sustained energy without the jittery overstimulation that caffeine produces.
Rhodiola demonstrates particular effectiveness for individuals experiencing burnout, that state of profound exhaustion accompanying chronic stress exposure. Studies show significant improvements in symptoms including fatigue, difficulty concentrating, decreased motivation, and irritability after four to twelve weeks of rhodiola supplementation. The herb appears to work partly by protecting mitochondrial function in neurons and other cells, preserving the energy production capacity that stress and inflammation compromise. This mitochondrial support explains rhodiola’s ability to sustain energy levels without relying on artificial stimulation.
Holy basil, known as tulsi in Ayurvedic tradition, offers gentler adaptogenic support particularly suited for stress affecting digestion and creating scattered, anxious mental states. This aromatic plant belongs to the mint family and contains numerous volatile oils including eugenol, along with other compounds that demonstrate anti-anxiety, anti-inflammatory, and immune-modulating properties. Holy basil works especially well for individuals whose stress manifests through digestive complaints, headaches, and difficulty focusing. Traditional use involved drinking holy basil tea daily as a general health tonic, an approach modern research supports for maintaining stress resilience.
Asian ginseng, specifically Panax ginseng, has been revered in Traditional Chinese Medicine for over two thousand years as a premier tonic for vitality and longevity. The root contains ginsenosides, unique compounds that influence the hypothalamic-pituitary-adrenal axis governing stress responses while also affecting glucose metabolism, immune function, and cognitive performance. Ginseng demonstrates particularly interesting effects on mental performance, with studies showing improvements in attention, memory, and reaction time alongside reduced mental fatigue. The herb appears most beneficial for individuals experiencing depletion after prolonged stress rather than those in acute high-stress phases.
Eleuthero, sometimes called Siberian ginseng though not botanically related to true ginseng, provides adaptogenic support with less stimulating effects than Asian ginseng. This woody shrub native to northeastern Asia contains eleutherosides that help normalize stress responses while supporting immune function. Research conducted initially in Soviet laboratories demonstrated eleuthero’s ability to enhance physical endurance and mental performance in athletes and workers performing demanding tasks. For nervous system support, eleuthero shows particular benefit for individuals needing to maintain high performance levels during demanding periods while preventing the burnout that often follows such intensity.
The optimal use of adaptogenic herbs involves consistent daily administration for extended periods rather than sporadic dosing during acute stress episodes. Most adaptogens require four to twelve weeks of regular use before full benefits manifest, as they work by gradually retraining stress response systems rather than forcing immediate changes. This timeline demands patience but produces lasting results that persist even after discontinuing the herbs, unlike medications requiring continued use to maintain effects. Many practitioners recommend cycling adaptogens, using them for several months then taking breaks, to prevent the body from adapting to their presence and diminishing responses.
Combining multiple adaptogens often produces synergistic effects superior to using single herbs, though formulation requires knowledge to avoid excessive stimulation or excessive sedation. Traditional medicine systems typically used complex formulas containing multiple herbs rather than relying on isolated botanicals, a practice modern herbalists increasingly embrace. However, beginners should start with single adaptogens to assess individual responses before combining multiple herbs. Working with qualified herbalists or integrative practitioners helps create personalized formulas matching specific nervous system needs and avoiding potential interactions with medications or health conditions.
Nervine Herbs: Immediate Calming and Support
While adaptogenic herbs build long-term resilience through gradual system rebalancing, nervine herbs provide more immediate relief from acute nervous tension, anxiety, insomnia, and stress-related symptoms. The category of nervine herbs encompasses botanicals that directly calm nervous system activity through various mechanisms including neurotransmitter modulation, muscle relaxation, and mild sedation. These herbs serve important roles in managing acute symptoms while the slower-acting adaptogens rebuild depleted reserves and restore healthy stress response patterns over months of use.
Valerian root ranks among the most renowned nervine herbs in Western herbalism, with documentation of medicinal use extending back to ancient Greece and Rome. The distinctive-smelling root of Valeriana officinalis contains numerous compounds including valerenic acid that influence GABA receptors in the brain, enhancing the calming effects of this inhibitory neurotransmitter. Unlike pharmaceutical sedatives that can produce morning grogginess or dependence, valerian provides gentle sleep support without hangover effects when used appropriately. Research shows valerian most effective for individuals experiencing difficulty falling asleep due to racing thoughts or general nervous tension rather than those with severe insomnia or sleep disorders requiring medical intervention.
Passionflower, derived from the climbing vine Passiflora incarnata, offers another powerful nervine option for calming overstimulated nervous systems. Traditional Native American use preceded European adoption, with colonial herbalists quickly recognizing passionflower’s effectiveness for anxiety, insomnia, and nervous restlessness. Modern research confirms the herb’s anxiolytic properties, with clinical trials showing effectiveness comparable to benzodiazepine medications but with fewer side effects and no addiction potential. Passionflower appears to work through multiple mechanisms including GABA receptor modulation and influences on neurotransmitters like serotonin. The herb suits individuals experiencing the exhausted but unable to relax phenomenon, where nervous system overstimulation prevents rest despite genuine fatigue.
Chamomile represents perhaps the most accessible nervine herb, available in virtually every grocery store as a popular tea. Both German chamomile and Roman chamomile contain beneficial compounds including apigenin that binds to benzodiazepine receptors in the brain, producing mild anxiolytic and sedative effects. Beyond direct nervous system calming, chamomile demonstrates particular affinity for the enteric nervous system in the gut, soothing digestive upset related to stress and anxiety. This dual action makes chamomile especially appropriate for individuals whose nervous tension manifests through stomach complaints. The herb’s safety profile allows use even in children and during pregnancy under appropriate guidance.
Lemon balm, scientifically known as Melissa officinalis, provides gentle nervine support with particular effectiveness for agitated mental states characterized by scattered thinking and difficulty concentrating. The aromatic leaves contain volatile oils and other compounds that influence GABA receptors while also demonstrating antioxidant and antiviral properties. Research shows lemon balm’s ability to reduce anxiety and agitation while simultaneously supporting cognitive function, an unusual combination since many calming herbs impair mental clarity. The herb suits daytime use when nervous tension needs relief but mental sharpness must remain intact. Lemon balm also demonstrates benefits for sleep quality when taken before bed, reducing nighttime awakenings.
The relationship between nervous system health and cognitive clarity becomes particularly evident when examining targeted herbal interventions. While comprehensive nervous system support addresses overall function, specific formulations targeting best herbs for mental clarity deliver enhanced information processing, reduced brain fog, and sharper concentration through mechanisms including improved cerebral circulation and neurotransmitter optimization. Understanding these specialized applications helps individuals select appropriate herbs matching their specific cognitive support needs beyond general nervous system wellness.
California poppy, despite its name suggesting relation to opium poppies, contains entirely different and non-addictive compounds that provide gentle sedative and anxiolytic effects. Native Americans used this herb for various purposes including sleep support and pain relief long before European settlement. Modern research validates California poppy’s effectiveness for mild to moderate anxiety and sleep difficulties, with mechanisms involving both GABA and serotonin systems. The herb demonstrates particular benefit for children experiencing anxiety-related sleep difficulties, though appropriate professional guidance remains essential for pediatric use of any herbal remedy.
Skullcap, particularly American skullcap (Scutellaria lateriflora), has long been valued in herbal medicine for nervous system tension and anxiety characterized by muscle tightness and restlessness. The herb contains numerous flavonoids including baicalin that demonstrate neuroprotective properties alongside the calming effects. Skullcap proves particularly useful for individuals who hold stress physically, developing tight shoulders, jaw clenching, or tension headaches. The herb helps break the cycle where mental stress creates physical tension that further exacerbates mental stress. Traditional use often combined skullcap with other nervines for comprehensive nervous system support.
Lavender extends beyond aromatherapy applications to offer genuine nervous system benefits when taken internally as tea or tincture. The aromatic compounds in lavender, particularly linalool and linalyl acetate, cross the blood-brain barrier to influence GABA receptors and neurotransmitter systems. Research shows lavender supplementation reduces anxiety symptoms while improving sleep quality and emotional wellbeing. The herb suits individuals experiencing generalized anxiety without specific panic attacks, providing gentle ongoing support rather than acute intervention. Lavender’s pleasant flavor and aroma make it easily incorporated into daily routines as tea or culinary herb.
The effective use of nervine herbs requires matching specific botanicals to individual presentations rather than assuming all nervines work identically. Some people respond excellently to valerian while others find it ineffective or even paradoxically stimulating. Personal experimentation under appropriate guidance helps identify which nervines provide optimal benefits. Starting with lower doses and gradually increasing allows assessment of individual sensitivity while minimizing risks of excessive sedation. Timing matters significantly, with some nervines working best taken thirty to sixty minutes before desired effects while others require several days of consistent use before benefits appear.
Neuroprotective Herbs: Guarding Your Brain’s Future
Beyond immediate stress relief and resilience building, certain herbs demonstrate remarkable abilities to protect nervous system structures from degenerative damage, preserve cognitive function against aging-related decline, and even promote regeneration of damaged neural tissue. These neuroprotective herbs work through mechanisms including antioxidant activity, anti-inflammatory effects, improved cerebral circulation, and direct influences on nerve growth factors. Incorporating neuroprotective botanicals into long-term wellness strategies may significantly reduce risks of neurodegenerative diseases while maintaining sharper cognitive function throughout the lifespan.
Bacopa monnieri, known as brahmi in Ayurvedic medicine, stands among the most extensively researched herbs for cognitive enhancement and neuroprotection. This creeping perennial thrives in wetland environments across Asia, with traditional use dating back over three thousand years for memory enhancement and mental clarity. The herb contains unique compounds called bacosides that demonstrate multiple neuroprotective mechanisms including antioxidant activity, enhanced neurotransmitter synthesis, and promotion of synaptic communication. Clinical trials consistently show bacopa supplementation improves memory formation, information processing speed, and attention after twelve weeks of daily use.
The mechanisms underlying bacopa’s cognitive benefits involve both immediate and long-term effects on brain structure and function. Research reveals bacopa increases dendritic branching and synaptic density in neurons, literally expanding the brain’s communication network. The herb also influences acetylcholine systems critical for memory formation while protecting cholinergic neurons from degradation. Animal studies demonstrate bacopa’s ability to reduce beta-amyloid plaque formation, the pathological hallmark of Alzheimer’s disease. These neuroprotective effects suggest potential preventive benefits for age-related cognitive decline, though human studies of sufficient duration to confirm prevention remain ongoing.
Gotu kola, another Ayurvedic herb called Centella asiatica botanically, provides neuroprotection through entirely different mechanisms than bacopa despite both being revered for cognitive support. This herb contains triterpenoid compounds including asiaticoside that stimulate nerve growth factor production and enhance neuronal regeneration after injury. Research shows gotu kola’s ability to accelerate wound healing extends to nervous tissue, with studies demonstrating improved peripheral nerve regeneration in animal models. The herb also demonstrates anxiolytic properties and cognitive enhancement, though its primary value lies in neuroprotection and support for nervous system repair processes.
Ginkgo biloba represents one of the oldest living tree species, surviving over two hundred million years with remarkable resilience. The fan-shaped leaves contain unique compounds including ginkgolides and bilobalide that improve cerebral circulation while demonstrating potent antioxidant and anti-inflammatory properties. Extensive research on ginkgo shows consistent improvements in memory, attention, and cognitive processing speed, particularly in elderly individuals experiencing mild cognitive impairment. The herb’s ability to enhance blood flow throughout the brain helps deliver oxygen and nutrients while removing metabolic wastes, supporting optimal neuronal function. Ginkgo also protects blood-brain barrier integrity, maintaining this critical defensive structure.
Lion’s mane mushroom, though technically a fungus rather than herb, deserves mention for extraordinary neuroprotective properties increasingly validated by scientific research. This distinctive mushroom contains compounds called hericenones and erinacines that cross the blood-brain barrier to stimulate nerve growth factor synthesis directly in brain tissue. Animal studies show lion’s mane promotes neurogenesis in the hippocampus, a brain region critical for memory formation and particularly vulnerable to age-related decline. Human studies demonstrate improvements in cognitive function and reduced anxiety and depression symptoms after several weeks of lion’s mane supplementation.
Turmeric, specifically its active compound curcumin, has gained substantial attention for neuroprotective properties extending far beyond its traditional use as culinary spice and anti-inflammatory agent. Curcumin demonstrates remarkable antioxidant potency while also influencing numerous cellular signaling pathways involved in neurodegeneration. Research shows curcumin’s ability to reduce inflammatory markers in brain tissue, prevent beta-amyloid plaque formation, and even clear existing plaques in animal models of Alzheimer’s disease. The compound also protects neurons from oxidative damage and supports mitochondrial function essential for cellular energy production. However, curcumin suffers from poor bioavailability, requiring strategic formulation with piperine or lipids to enhance absorption.
Rosemary, the aromatic culinary herb, contains carnosic acid and other compounds with potent neuroprotective properties. Research reveals rosemary’s ability to prevent oxidative damage in brain tissue while also improving cerebral circulation. The herb demonstrates particular protective effects against age-related cognitive decline and may reduce risks of neurodegenerative diseases. Interestingly, even aromatherapy exposure to rosemary essential oil shows cognitive benefits, with studies documenting improved memory performance and alertness in individuals exposed to rosemary aroma. The dual benefits from culinary use and aromatherapy make rosemary an easily accessible neuroprotective herb for daily incorporation.
Green tea, consumed for millennia across Asia, provides neuroprotection through polyphenol compounds particularly epigallocatechin gallate. These antioxidants cross the blood-brain barrier to protect neurons from oxidative stress while also demonstrating anti-inflammatory and anti-cancer properties. Research shows regular green tea consumption associates with reduced risks of cognitive decline, Parkinson’s disease, and Alzheimer’s disease. The modest caffeine content in green tea provides mental alertness without the jittery overstimulation that excessive coffee produces, while L-theanine amino acids promote relaxed focus. This combination makes green tea particularly valuable for supporting both immediate cognitive function and long-term brain health.
Leading medical institutions continue validating the connection between nutrition and neurological health through rigorous research. Mayo Clinic investigators have documented how nutrient rich diets maximize memory function by providing essential compounds that support neurotransmitter synthesis, reduce oxidative stress, and maintain optimal cerebral blood flow. These findings reinforce the importance of combining herbal supplementation with comprehensive dietary strategies for supporting long-term brain health and cognitive performance.
The interconnection between peripheral circulation and nervous system function deserves greater attention than it typically receives. Research demonstrates that simple interventions treating cold feet through bath temperature optimization improve blood flow not only to extremities but enhance overall nervous system performance by ensuring adequate oxygen and nutrient delivery to nerve tissues throughout the body. This holistic understanding recognizes that supporting peripheral circulation provides foundational benefits for central nervous system health and cognitive function.
The strategic use of neuroprotective herbs ideally begins well before obvious cognitive decline appears, as prevention proves far more effective than attempting to reverse established damage. Starting neuroprotective supplementation in middle age provides decades of protective benefits accumulating to significantly reduce neurodegenerative disease risks. However, research shows benefits even when starting neuroprotective herbs after mild cognitive impairment develops, suggesting it’s never too late to begin supporting brain health. Combining multiple neuroprotective herbs with complementary mechanisms often produces superior results compared to relying on single botanicals, though formulation requires knowledge to avoid potential interactions.
Traditional Medicine Systems and Nervous System Support
Understanding how traditional medicine systems approach nervous system health provides valuable context for using herbs effectively while honoring the wisdom accumulated over millennia. Unlike Western medicine’s tendency to isolate symptoms and target specific pathologies, traditional systems view nervous system health within broader frameworks encompassing constitutional types, energetic qualities, and interconnected organ systems. This holistic perspective offers insights that purely biochemical approaches sometimes miss, leading to more nuanced and individualized herbal protocols.
Traditional Chinese Medicine regards the nervous system through concepts of Shen, often translated as “spirit” or “mind,” housed in the Heart organ system. Disturbances in Shen manifest as anxiety, insomnia, poor memory, or emotional instability, requiring interventions that calm and nourish the Heart while addressing underlying patterns of excess or deficiency. TCM practitioners assess individual constitutions, identifying patterns like Heart Yin deficiency or Heart Fire that guide specific herbal formulas. This personalized approach explains why different people with similar symptoms might receive entirely different herbs based on their unique constitutional presentations.
Ayurvedic medicine, India’s ancient healing system, categorizes individuals into three doshas or constitutional types: Vata, Pitta, and Kapha. Each dosha relates to specific nervous system tendencies and vulnerabilities. Vata types, governed by air and space elements, tend toward anxiety, scattered thinking, and nervous exhaustion when imbalanced. Pitta types, representing fire and water, may experience intense mental focus that becomes rigid or inflammatory when excessive. Kapha types, embodying earth and water, generally maintain emotional stability but can become mentally dull or depressed when imbalanced. Ayurvedic practitioners select herbs specifically to balance the individual’s doshic constitution rather than simply treating symptoms.
The Ayurvedic concept of Rasayana, or rejuvenation therapy, specifically addresses nervous system vitality and longevity. Rasayana herbs like ashwagandha, bacopa, and gotu kola aim not merely to treat disease but to enhance overall vitality, extend lifespan, and improve quality of life through supporting fundamental physiological processes. This preventive focus contrasts with Western medicine’s disease-centered approach, offering valuable perspectives on maintaining nervous system health throughout the lifespan rather than waiting for problems to emerge before intervening.
Native American herbal traditions, while diverse across hundreds of distinct tribal cultures, generally emphasize spiritual and emotional dimensions of healing alongside physical interventions. Herbs for nervous system support often involved ceremonial contexts, prayers, and relationship-building with plant spirits. This integration of psychological, spiritual, and physical healing reflects sophisticated understanding of how these dimensions interconnect to influence overall wellbeing. While modern use typically omits ceremonial elements, recognizing the original context adds depth to understanding these herbs’ traditional applications.
Shop on AliExpress via link: wholesale-herbal-supplement-organizer
European folk medicine traditions contributed significantly to modern Western herbalism, with documentation of medicinal plant use extending back through medieval monastery gardens to ancient Greek and Roman physicians. Herbs like valerian, St. John’s wort, and lemon balm figured prominently in European traditions for treating “nervous complaints,” melancholy, and insomnia. The doctrine of signatures, suggesting plants’ appearance indicated their medicinal uses, influenced herb selection though modern science validates many traditional choices through mechanisms unrelated to visual resemblance. European traditions also emphasized constitutional types, though conceptualized differently than Ayurvedic doshas or Chinese organ systems.
African traditional medicine encompasses enormous diversity across the continent’s many cultures and ecosystems, with numerous herbs used for nervous system support varying by region. While less documentation exists compared to Asian and European traditions, African herbs demonstrate powerful effects validating their traditional use. Plants like African ginger, kanna, and various regional species show promise for anxiety, depression, and cognitive support. The holistic orientation of African healing traditions, often involving divination, community ritual, and spiritual healing alongside herbal remedies, parallels indigenous approaches worldwide in recognizing multidimensional aspects of nervous system health.
Modern herbalism increasingly draws from multiple traditional systems, creating integrative approaches that combine insights from diverse healing lineages. This synthesis honors traditional wisdom while allowing flexibility to address contemporary health challenges that ancient practitioners never encountered. However, respectful integration requires understanding herbs within their original contexts rather than simply extracting botanical “ingredients” divorced from traditional frameworks. Working with practitioners trained in specific traditions ensures more authentic applications while avoiding cultural appropriation or misuse of sacred medicines.
How to Choose and Use Nervous System Herbs Safely
Translating knowledge about nervous system herbs into safe and effective personal use requires understanding quality considerations, appropriate dosing, potential interactions, and important contraindications. While herbs generally demonstrate superior safety profiles compared to pharmaceutical medications, they remain biologically active substances capable of producing unwanted effects when used inappropriately. Informed decision-making protects health while maximizing therapeutic benefits from these powerful botanical medicines.
Quality represents the single most critical factor determining both safety and effectiveness of herbal supplements. The herbal supplement industry remains poorly regulated compared to pharmaceuticals, with concerning variability in product quality, accurate labeling, and contamination risks. Independent testing by organizations like ConsumerLab, NSF International, and USP reveals that many supplements contain less than stated amounts of active compounds, while others harbor concerning levels of heavy metals, pesticides, or microbial contamination. Choosing products from reputable manufacturers who provide third-party testing certificates and follow Good Manufacturing Practices significantly reduces these risks.
Understanding regulatory frameworks governing herbal supplements helps consumers navigate quality concerns effectively. The Food and Drug Administration maintains comprehensive databases on dietary supplement ingredients documenting their actions, safety evaluations, and regulatory status for various botanical products. While dietary supplements receive less stringent oversight than pharmaceutical drugs, consulting official regulatory resources provides valuable context for making informed choices about nervous system herbs.
Source matters tremendously for herb quality and sustainability. Organically grown herbs avoid pesticide residues that can accumulate in nervous tissue, while wildcrafted herbs should come from companies committed to sustainable harvesting practices preventing species depletion. Some traditional medicine plants face extinction pressures from overharvesting, making careful sourcing ethically imperative. Companies transparent about sourcing, willing to provide certificates of analysis, and committed to fair trade practices deserve preference over cheaper products with unknown origins and questionable quality control.
Form of preparation influences both effectiveness and ease of use for nervous system herbs. Traditional teas or decoctions provide time-honored methods offering ritual benefits alongside medicinal effects, though preparation requires effort and active compounds may not extract completely in water alone. Tinctures, made by extracting herbs in alcohol, concentrate active constituents while preserving them for years, providing convenient dosing and good bioavailability for many herbs. Capsules and tablets offer maximum convenience but may have lower bioavailability unless properly formulated. Some herbs require specific preparation methods to optimize therapeutic compounds while minimizing potentially problematic constituents.
Dosing nervous system herbs appropriately balances effectiveness with safety while accounting for individual variation in sensitivity and response. General dosing guidelines exist for most herbs based on traditional use and clinical research, typically expressed as ranges rather than single values. Starting at lower ends of recommended ranges allows assessment of individual tolerance before increasing doses. Some individuals prove remarkably sensitive to herbs requiring only fractions of standard doses, while others need higher amounts for noticeable effects. Body weight, age, health status, and concurrent medications all influence appropriate dosing.
Systematic reviews of clinical research provide essential guidance for safe herbal use. Comprehensive analyses examining nutritional herbal supplements for anxiety disorders document both efficacy and safety profiles for commonly used nervine herbs including passionflower, kava, and magnesium-containing formulations. These evidence-based reviews help practitioners and patients make informed decisions about which botanicals offer the strongest support for specific nervous system concerns while minimizing potential adverse effects.
Timing of herb administration significantly impacts effectiveness, with different herbs requiring different scheduling for optimal benefits. Adaptogenic herbs typically work best when taken consistently at the same time daily, often in morning to align with natural cortisol rhythms. Nervine herbs for sleep support should be taken thirty to ninety minutes before bedtime, allowing time for absorption and onset of effects. Some herbs perform better with food to reduce stomach upset or enhance absorption, while others require empty stomach dosing for optimal bioavailability. Following traditional usage patterns and modern research recommendations guides appropriate timing.
Major academic medical centers provide valuable patient education about botanical medicine safety and applications. Johns Hopkins Medicine experts emphasize that herbal medicine wellness approaches require understanding both traditional uses and modern safety considerations including potential drug interactions and quality control issues. Their comprehensive resources help patients work effectively with healthcare providers to integrate herbal interventions into evidence-based treatment plans for nervous system support.
Duration of use varies dramatically between herb categories and individual needs. Acute-acting nervines for occasional sleep difficulties or anxiety might be used intermittently as needed without building tolerance or dependence. Adaptogenic herbs require consistent daily use for weeks or months to produce optimal benefits, with many practitioners recommending periodic breaks after several months to prevent adaptation. Neuroprotective herbs aimed at preventing cognitive decline may be used indefinitely as long-term preventive strategies. Understanding appropriate duration prevents both premature discontinuation before benefits manifest and unnecessarily prolonged use when shorter courses suffice.
Potential interactions between herbs and medications represent serious safety concerns requiring careful attention. Many herbs significantly influence drug metabolism through effects on cytochrome P450 enzymes in the liver, potentially altering blood levels of numerous medications. St. John’s wort famously interacts with dozens of drugs including birth control pills, antidepressants, and blood thinners. Sedative herbs may dangerously enhance effects of sleep medications, anti-anxiety drugs, or other central nervous system depressants. Always disclose all supplements to physicians and pharmacists, allowing assessment of interaction risks before combining herbs with prescription medications.
Contraindications, conditions where specific herbs should be avoided entirely, must be carefully respected to prevent serious adverse effects. Pregnancy and breastfeeding represent absolute contraindications for many herbs due to risks of premature labor, fetal effects, or transfer through breast milk. Upcoming surgeries require discontinuing herbs that affect bleeding or interact with anesthesia, typically stopping two weeks before procedures. Active psychotic disorders may worsen with certain herbs affecting neurotransmitters. Liver or kidney disease demands caution with herbs metabolized or eliminated through these organs. Medical guidance becomes essential when contraindications exist.
Working with qualified healthcare practitioners, particularly those trained in herbal medicine like naturopathic doctors, herbalists, or integrative physicians, provides personalized guidance impossible from general information. These practitioners can assess individual health status, consider existing medications and conditions, and create tailored herbal protocols matching specific needs. They also provide ongoing monitoring to assess effectiveness and watch for potential problems. While self-care with herbs offers valuable empowerment, complex situations involving serious health conditions, multiple medications, or persistent symptoms warrant professional consultation.
Conclusion: Integrating Herbal Wisdom into Modern Life
The journey through nervous system herbs reveals a wealth of botanical wisdom accumulated across millennia of human experience, increasingly validated by modern scientific investigation. These remarkable plants offer sophisticated tools for supporting nervous system health through multiple complementary mechanisms, from immediate symptomatic relief to long-term neuroprotection and resilience building. Yet the true power of herbal medicine emerges not from viewing herbs as green pharmaceuticals to be prescribed for specific symptoms, but from integrating them within comprehensive approaches to nervous system wellness that honor the interconnected nature of physical, mental, emotional, and spiritual health.
Modern life places unprecedented demands on nervous systems never designed for constant digital stimulation, relentless work pressures, social media comparison, and separation from natural rhythms. The epidemic of anxiety, depression, cognitive decline, and stress-related diseases reflects nervous systems overwhelmed by chronic activation without adequate recovery periods. While herbs provide valuable support for managing these challenges, they work most effectively within broader lifestyle frameworks addressing root causes rather than simply masking symptoms. Sleep hygiene, stress management practices, regular physical activity, meaningful social connections, time in nature, and nutrient-dense diets create foundations upon which herbal interventions build enhanced benefits.
The democratization of herbal knowledge through increased access to information empowers individuals to take active roles in their health, reclaiming agency often surrendered to medical authorities. However, this empowerment carries responsibilities including educating oneself about safe usage, respecting the power of botanical medicines, and recognizing when professional guidance becomes necessary. Herbs represent sophisticated pharmacological interventions capable of producing significant physiological effects, deserving the same respect and careful use as any medicine. The casualness with which some approach herbal supplements, assuming “natural equals safe,” can lead to adverse effects, interactions, or inappropriate self-treatment of serious conditions requiring medical care.
Looking forward, the convergence of traditional herbal wisdom and modern neuroscience research promises exciting developments in nervous system support. Emerging technologies allow unprecedented investigation of herbal mechanisms at molecular levels, validating traditional use while revealing new applications. Personalized medicine approaches incorporating genetic testing may eventually allow precise matching of specific herbs to individual genetic profiles, optimizing effectiveness while minimizing risks. Growing acceptance of integrative approaches within conventional medicine creates opportunities for collaboration between herbalists and physicians, providing patients with comprehensive care drawing from multiple healing traditions.
The sustainability challenges facing medicinal plant populations demand urgent attention as demand for herbal supplements grows globally. Overharvesting threatens numerous species with extinction while destroying ecosystems and displacing indigenous communities depending on these plants. Conscious consumers must prioritize products from companies committed to sustainable sourcing, fair trade practices, and habitat preservation. Supporting efforts to cultivate traditionally wildcrafted herbs reduces pressure on wild populations while ensuring future availability. The relationship with medicinal plants extends beyond extraction of therapeutic compounds to encompass stewardship responsibilities ensuring these botanical allies remain available for future generations.
Perhaps most profoundly, working with herbs for nervous system support invites reconnection with the natural world and recognition of interdependence between human health and ecological health. The plants offering nervous system support do so through billions of years of co-evolution, developing chemical compounds serving their own survival that happen to interact beneficially with human biochemistry. This ancient relationship between plants and humans deserves respect, gratitude, and reciprocity rather than simple extraction and exploitation. Traditional indigenous relationships with plant medicines, involving prayer, ceremony, and giving back, model approaches that modern herbalism increasingly embraces.
The path forward involves integrating the best of multiple healing traditions while remaining grounded in scientific rigor and appropriate skepticism. Not every traditional use withstands scientific scrutiny, while laboratory investigations sometimes miss subtle effects traditional observation captured. Holding both traditional wisdom and modern science in creative tension allows for sophisticated understanding respecting the complexity of both herbs and human physiology. This integration serves nervous systems struggling under modern pressures, providing tools for not merely surviving but thriving in challenging times.
For individuals suffering with compromised nervous system health, whether from chronic stress, anxiety, cognitive difficulties, or simple desire to optimize function and prevent future decline, herbs offer hope grounded in thousands of years of human experience. These botanical allies provide support through the hardest times while helping build resilience for challenges ahead. They remind us that solutions to modern problems sometimes lie not in ever more sophisticated technological interventions but in ancient wisdom passed down through generations who understood the profound connections between plants, people, and health. In returning to these green allies, we reclaim power over our wellbeing while honoring the natural world sustaining all life.
Frequently Asked Questions
Question 1: What are the best herbs for strengthening the nervous system?
Answer 1: The most effective herbs for nervous system support include ashwagandha, which reduces cortisol and protects neurons while rebuilding stress resilience over time. Bacopa monnieri enhances memory formation and cognitive function through promoting synaptic communication and neuronal branching. Gotu kola stimulates nerve growth factor production supporting nervous tissue repair and regeneration. Rhodiola rosea combats mental and physical fatigue while protecting mitochondrial function in neurons. Holy basil provides gentle adaptogenic support particularly beneficial when stress affects digestion and creates scattered thinking. These herbs work through complementary mechanisms addressing different aspects of nervous system health, with research validating traditional uses through thousands of years. Individual responses vary significantly, making personal experimentation under appropriate guidance essential for identifying optimal herbs. Most adaptogenic herbs require consistent daily use for three to six months before producing full benefits as they gradually restore system balance rather than forcing immediate changes.
Question 2: How long does it take for nervous system herbs to work?
Answer 2: Timeline for herbal effects varies dramatically based on herb category and intended outcomes. Nervine herbs like chamomile, lemon balm, and passionflower provide immediate calming effects within thirty to ninety minutes of administration, making them suitable for acute anxiety or occasional sleep difficulties. These rapid-acting herbs influence neurotransmitter receptors directly, producing noticeable relaxation relatively quickly. However, adaptogenic herbs that rebuild stress resilience and strengthen depleted nervous systems require substantially longer commitment. Ashwagandha, rhodiola, holy basil, and similar adaptogens typically need six to twelve weeks of daily consistent use before optimal benefits manifest. This delayed onset reflects their mechanisms of gradually normalizing hypothalamic-pituitary-adrenal axis function and restoring neurotransmitter balance rather than producing forced immediate changes. Neuroprotective herbs aimed at preserving cognitive function and preventing neurodegeneration work even more slowly, with benefits accumulating over years of consistent use. Clinical research consistently demonstrates that premature discontinuation before adequate trial periods prevents experiencing the significant improvements these herbs provide with patience.
Question 3: Can herbs really repair nerve damage?
Answer 3: The relationship between herbs and nerve repair requires nuanced understanding distinguishing between dramatic claims and scientifically supported possibilities. Herbs cannot reverse severe traumatic nerve damage or cure degenerative neurological diseases when used alone. However, substantial research demonstrates that specific botanical compounds do promote neurogenesis, the birth of new neurons in certain brain regions, and stimulate production of nerve growth factors supporting axonal regeneration. Lion’s mane mushroom contains hericenones and erinacines that cross the blood-brain barrier to directly enhance nerve growth factor synthesis in neural tissue. Gotu kola’s triterpenoid compounds accelerate peripheral nerve regeneration after injury in animal models. Bacopa monnieri promotes dendrite branching and synaptic formation, literally expanding neuronal communication networks. These herbs work by supporting the nervous system’s inherent capacity for repair and regeneration rather than magically reversing established damage. The effects accumulate gradually over months of consistent use, proving most beneficial when started early in disease processes or used preventively before significant damage occurs. Realistic expectations recognize herbs as valuable supportive tools within comprehensive treatment approaches rather than miraculous cures.
Question 4: Are nervous system herbs safe to take daily?
Answer 4: Most traditional nervine and adaptogenic herbs demonstrate excellent safety profiles when used appropriately at recommended doses over extended periods. Thousands of years of human use across multiple cultures provides substantial safety data that modern clinical trials continue confirming. However, several critical factors influence safety requiring careful attention. Quality matters enormously, as contamination with heavy metals, pesticides, or misidentified plant species creates risks that pure, properly identified herbs do not carry. Some herbs require caution in specific populations including pregnant or breastfeeding women, children, elderly individuals, or those with particular health conditions. Certain herbs affect liver function, with kava representing the most concerning example requiring monitoring in susceptible individuals. Drug interactions pose significant risks, as many herbs influence medication metabolism potentially altering blood levels dangerously. Starting with lower doses and gradually increasing while monitoring for side effects provides conservative approach minimizing risks. Working with qualified practitioners trained in herbal medicine ensures personalized guidance accounting for individual circumstances, medications, and health conditions that might contraindicate specific herbs.
Question 5: What’s the difference between nervines and adaptogens?
Answer 5: Nervine and adaptogenic herbs represent distinct categories with fundamentally different mechanisms and applications for nervous system support. Nervine herbs provide direct effects on nervous tissue and neurotransmitter systems, producing relatively immediate calming, sedation, or muscle relaxation. Examples include valerian, passionflower, chamomile, and lemon balm which influence GABA receptors and other neurotransmitter systems to reduce nervous tension and promote rest. These herbs suit acute situations requiring prompt symptom relief like occasional anxiety or difficulty sleeping. Effects typically manifest within minutes to hours and dissipate relatively quickly after discontinuation. Conversely, adaptogenic herbs work through entirely different mechanisms by normalizing hypothalamic-pituitary-adrenal axis function and improving stress response capacity over time. Adaptogens like ashwagandha, rhodiola, and holy basil don’t force immediate changes but gradually retrain how the body responds to stressors while building resilience. The same adaptogen can calm overactive systems while energizing depleted ones, adjusting effects based on individual needs rather than producing uniform responses. This bidirectional normalization distinguishes adaptogens from nervines providing consistent effects regardless of initial state.
Question 6: Which herbs help with nerve pain?
Answer 6: Several herbs demonstrate potential for managing neuropathic pain, though effectiveness varies considerably between individuals and conditions. St. John’s wort contains hyperforin and hypericin that influence nerve signal transmission while providing anti-inflammatory effects, showing benefits for some types of nerve pain in clinical studies. California poppy offers gentle analgesic properties through alkaloid compounds affecting pain perception without addiction risks associated with pharmaceutical opioids. Corydalis, used traditionally in Chinese medicine, contains dehydrocorybulbine that influences dopamine receptors involved in pain processing. Turmeric’s curcumin reduces inflammatory cytokines that sensitize nerve endings while protecting neurons from oxidative damage. However, nerve pain represents a complex symptom requiring comprehensive medical evaluation to identify underlying causes. Conditions like diabetic neuropathy, postherpetic neuralgia, or nerve compression each require specific approaches beyond symptom management. While herbs provide valuable supportive tools potentially reducing pain intensity and improving quality of life, they should complement rather than replace proper medical diagnosis and treatment. Persistent or severe nerve pain always warrants professional evaluation to rule out serious underlying conditions requiring medical intervention.
Question 7: Can I take multiple nervous system herbs together?
Answer 7: Combining compatible herbs often produces synergistic effects superior to using isolated botanicals, reflecting traditional medicine practices worldwide that typically employed complex formulas rather than single herbs. However, successful combination requires understanding herb properties, mechanisms, and potential interactions to avoid excessive effects in any single direction. Pairing calming nervines like chamomile with adaptogenic herbs like ashwagandha provides both immediate symptom relief and long-term resilience building through complementary actions. Combining herbs with different mechanisms, such as GABA-enhancing valerian with circulation-improving ginkgo, targets multiple aspects of nervous system health simultaneously. Traditional formulas often include small amounts of numerous herbs rather than large doses of few botanicals, distributing therapeutic effects across various pathways. However, beginners should start with single herbs to assess individual responses before combining multiple botanicals. Some combinations may produce excessive sedation, overstimulation, or interactions requiring reduction of individual doses. Working with qualified herbalists or integrative practitioners helps create personalized formulas matching specific nervous system needs while avoiding potential problems from inappropriate combinations or excessive total herb load.
Question 8: Do nervous system herbs interact with medications?
Answer 8: Herb-drug interactions represent serious concerns requiring careful attention, as numerous herbs significantly influence pharmaceutical medication metabolism, effectiveness, and side effect profiles. St. John’s wort strongly induces cytochrome P450 enzymes in liver that metabolize over fifty percent of prescription medications, potentially reducing drug blood levels dangerously including birth control pills, antidepressants, blood thinners, and immunosuppressants. Sedative herbs may additively enhance effects of sleep medications, anti-anxiety drugs, or other central nervous system depressants, producing excessive sedation or respiratory depression. Adaptogens affecting cortisol might interact with hormone replacement therapy or medications for thyroid or adrenal conditions. Herbs influencing neurotransmitters can interact with psychiatric medications targeting the same systems. Some herbs affect blood clotting requiring discontinuation before surgeries to prevent bleeding complications. Individual genetic variations in drug metabolism enzymes create additional unpredictability in interaction severity between people. These risks necessitate full disclosure of all supplements to prescribing physicians and pharmacists before starting herbs or medications. Healthcare providers can assess specific interaction risks based on exact medications and herbs involved, providing personalized guidance for safe concurrent use.
Question 9: What herbs help with anxiety and nervous tension?
Answer 9: Several herbs demonstrate particular effectiveness for anxiety and nervous tension through various complementary mechanisms. Passionflower provides rapid anxiolytic effects through GABA receptor modulation, reducing symptoms within hours of administration while maintaining mental clarity unlike pharmaceutical sedatives. Lemon balm offers gentle anxiety relief particularly effective for agitated states with scattered thinking, working through GABA and other neurotransmitter systems. Lavender demonstrates anxiety reduction in clinical trials when taken internally as supplement or used aromatically, with calming compounds crossing blood-brain barrier to influence nervous system function. Chamomile provides time-honored anxiety support with excellent safety profile suitable even for children under appropriate guidance. For chronic anxiety with underlying stress exhaustion, adaptogenic herbs prove more appropriate than immediate-acting nervines. Ashwagandha significantly reduces anxiety scores in clinical trials while addressing root cause of HPA axis dysfunction causing heightened anxiety responses. Holy basil offers gentle adaptogenic support particularly beneficial when anxiety manifests alongside digestive complaints. Rhodiola combats the mental and physical fatigue often accompanying chronic anxiety states. Combining immediate-acting nervines for acute symptom relief with longer-term adaptogens addressing underlying stress physiology provides comprehensive anxiety management.
Question 10: Are there herbs specifically for brain fog and mental fatigue?
Answer 10: Several herbs target cognitive clarity and mental energy through mechanisms improving cerebral blood flow, supporting neurotransmitter synthesis, and protecting brain cells from oxidative stress. Bacopa monnieri specifically enhances information processing speed, memory formation, and overall cognitive performance through promoting synaptic communication and neuronal branching, with benefits manifesting after twelve weeks of consistent daily use. Ginkgo biloba improves oxygen and nutrient delivery to brain tissue through vasodilation and blood flow enhancement while demonstrating antioxidant properties protecting neurons from free radical damage. The improvements in attention, memory, and processing speed prove particularly notable in individuals experiencing age-related cognitive decline or vascular contributions to mental fog. Rosemary increases cerebral circulation while providing neuroprotective antioxidants, with even aromatherapy exposure demonstrating memory and alertness improvements in research studies. Lion’s mane mushroom stimulates nerve growth factor production supporting neurogenesis and neural network expansion that underlies improved cognitive function over months of use. Rhodiola rosea combats mental and physical fatigue through protecting mitochondrial energy production in neurons and other cells. These cognitive-enhancing herbs work most effectively when addressing underlying causes of mental fatigue including poor sleep, chronic stress, nutritional deficiencies, and inadequate physical activity rather than simply forcing artificial stimulation.
Articles related:
Tags
📧 Get More Articles Like This
Subscribe to receive product reviews and buying guides in your inbox!
We respect your privacy. Unsubscribe at any time.