Strengthening the Heart Muscle and Circulatory System Through Nutrition and Exercise
Table of Contents
- Understanding the Heart Muscle and Circulatory System
- The Foundation: Nutrition for Cardiovascular Strength
- Essential Nutrients That Build Heart Muscle
- Exercise Strategies for Cardiovascular Enhancement
- Combining Nutrition and Exercise for Maximum Impact
- Lifestyle Factors That Support Heart Health
- Monitoring Progress and Measuring Success
- Frequently Asked Questions
Introduction
The morning Sarah collapsed during her usual jog through the park marked the beginning of her unexpected journey into understanding what it truly means to have a strong heart. At forty-two, she had considered herself relatively healthy, maintaining a regular exercise routine and watching her diet with casual attention. The diagnosis of early-stage cardiovascular dysfunction came as a shock, not just to her but to her entire family who had watched her seemingly healthy lifestyle unfold over the years. Her cardiologist’s words echoed in her mind during those first uncertain days after the incident: “Your heart muscle needs more than sporadic attention—it needs strategic, evidence-based support through both nutrition and exercise.” This revelation became the catalyst for Sarah’s transformation and mirrors a critical truth that millions around the world are discovering—cardiovascular health requires more than good intentions; it demands informed, consistent action.
The statistics surrounding cardiovascular disease paint a sobering picture of our current health landscape. According to recent data from the Centers for Disease Control and Prevention, cardiovascular disease remains the leading cause of death globally, accounting for nearly one in every three deaths in the United States alone. More alarming still is the fact that approximately eighty percent of cardiovascular disease cases are preventable through lifestyle modifications, primarily involving nutrition and exercise interventions. These numbers represent not just abstract statistics but real individuals—parents, partners, children, and friends—whose lives could be dramatically altered through informed choices about what they eat and how they move their bodies. The gap between knowing these facts and implementing effective change represents one of the most significant public health challenges of our time.
Public health institutions continue investigating the most effective interventions for translating cardiovascular disease knowledge into widespread behavior change at population levels. This research examines not only individual risk factors but also the social determinants, environmental influences, and systemic barriers that shape dietary and physical activity patterns across communities. Understanding these broader contexts helps inform both personal health decisions and policy initiatives aimed at creating environments that support rather than hinder cardiovascular wellness through preventing cardiovascular disease efforts for all populations.
efore delving into the details of the article, watch this video for the following anatomical explanation of the amazing transformations that occur in the heart and blood vessels during physical exertion :
Sarah’s story took a hopeful turn when she connected with a comprehensive cardiac rehabilitation program that emphasized the synergistic relationship between nutrition and exercise. Within the first month of following evidence-based protocols, her energy levels began to climb, her resting heart rate dropped from eighty-seven to seventy-two beats per minute, and her blood pressure measurements showed consistent improvements. The transformation wasn’t magical—it was methodical, grounded in scientific understanding of how specific nutrients fuel cardiac tissue and how targeted exercise strengthens the intricate network of cardiovascular structures. Her journey from that frightening morning in the park to regaining robust heart health illustrates a fundamental principle that research continues to validate: the heart muscle and circulatory system respond remarkably well to proper nutritional support and strategic physical conditioning when both elements work in concert.
Understanding the mechanics of how nutrition and exercise strengthen the cardiovascular system requires appreciating the heart’s unique position as both a muscle and a tireless pump. Unlike skeletal muscles that rest between contractions, the heart beats approximately one hundred thousand times each day, pumping roughly two thousand gallons of blood through an estimated sixty thousand miles of blood vessels. This extraordinary workload demands constant fuel, efficient waste removal, and structural integrity that can only be maintained through optimal nutrition and regular conditioning. The heart muscle cells, or cardiomyocytes, require specific nutrients to generate the enormous amounts of energy needed for continuous contraction, while the endothelial cells lining blood vessels depend on particular compounds to maintain flexibility and prevent dangerous plaque accumulation. When nutrition provides these essential building blocks and exercise creates the stimulus for adaptation, the cardiovascular system responds with enhanced strength, efficiency, and resilience.
The modern understanding of cardiovascular strengthening has evolved significantly from simple recommendations to “eat less fat and exercise more.” Contemporary research reveals that the quality of fats matters immensely, that certain carbohydrates can be protective while others are harmful, and that different types of exercise produce distinct cardiovascular benefits. The Mediterranean dietary pattern, for instance, has demonstrated remarkable cardiovascular protection in numerous studies, not through the elimination of fats but through the emphasis on healthy fats from sources like olive oil, nuts, and fatty fish. Similarly, exercise science has progressed beyond the notion that more is always better, recognizing that strategic combinations of aerobic training, resistance work, and high-intensity intervals create optimal cardiovascular adaptations. This nuanced approach to heart health acknowledges the complexity of human physiology while providing actionable strategies that individuals can implement regardless of their starting point.
Leading cardiology organizations have established comprehensive frameworks that outline optimal eating patterns for long-term heart protection. These diet and lifestyle recommendations emphasize whole food consumption while providing practical strategies for reducing processed food intake and managing portion sizes. The guidance reflects decades of nutritional research synthesized into actionable steps that individuals can implement regardless of their current dietary habits or cultural food preferences.
The compelling evidence for lifestyle-based cardiovascular strengthening extends well beyond individual success stories like Sarah’s. Large-scale longitudinal studies tracking tens of thousands of participants over decades have consistently demonstrated that individuals who maintain both healthy dietary patterns and regular physical activity experience dramatically lower rates of heart attacks, strokes, and cardiovascular mortality compared to their sedentary peers with poor nutritional habits. The Framingham Heart Study, which has followed multiple generations since 1948, provides some of the most robust data linking specific lifestyle factors to cardiovascular outcomes. More recent research utilizing advanced imaging techniques has shown that these benefits aren’t merely statistical—they manifest as measurable improvements in arterial flexibility, reduced atherosclerotic plaque burden, and enhanced cardiac contractility. The heart muscle literally becomes stronger and more efficient when supported by appropriate nutrition and regular exercise, demonstrating the remarkable plasticity of cardiovascular tissue even in individuals who begin making changes later in life.
Perhaps most encouraging for those beginning their cardiovascular strengthening journey is the rapidity with which positive changes can begin. While structural improvements to heart muscle and arterial health develop over months and years, beneficial metabolic shifts occur within weeks of implementing healthier nutrition and exercise patterns. Blood pressure often begins declining within two to three weeks of consistent lifestyle modifications, while improvements in cholesterol profiles typically appear within six to eight weeks. These early wins provide crucial motivation for continuing the journey toward comprehensive cardiovascular health, creating a positive feedback loop where initial successes fuel ongoing commitment. The key lies in understanding that cardiovascular strengthening isn’t a destination but rather an ongoing practice—one that becomes progressively easier and more rewarding as healthy habits become integrated into daily life and the body’s cardiovascular system responds with enhanced vitality and resilience.
Academic medical centers continue advancing our understanding of how specific food choices influence cardiac function at the cellular level. Recent research has clarified which dietary components provide the most substantial protection against arterial damage and cardiac dysfunction, moving beyond outdated nutritional paradigms toward more sophisticated appreciation of food quality. This evolving knowledge base helps individuals make informed decisions about heart healthy eating that support optimal cardiovascular outcomes throughout the lifespan.
Specific nutritional strategies designed for individuals engaged in regular physical training can accelerate cardiovascular adaptations while supporting recovery between exercise sessions. Understanding how to fuel activity optimally ensures that the body receives appropriate nutrients when they’re needed most, enhancing both performance during workouts and the beneficial remodeling that occurs afterward. This integration of exercise science with nutritional timing principles represents an important advancement beyond generic dietary advice toward more personalized approaches that recognize the unique demands of active lifestyles.
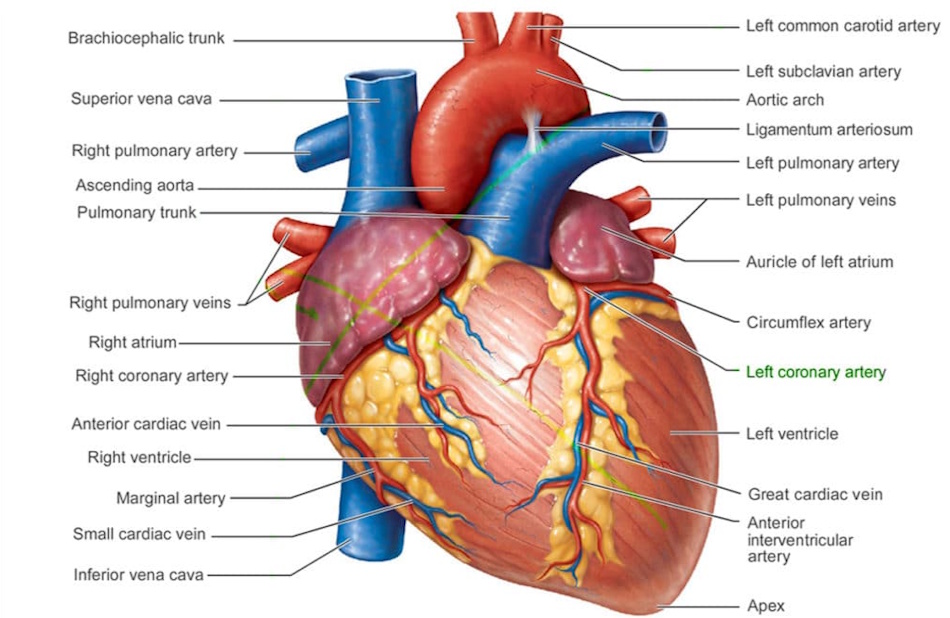
Understanding the Heart Muscle and Circulatory System
The human heart represents one of nature’s most remarkable engineering achievements, a fist-sized organ weighing approximately ten ounces that manages to pump blood continuously for decades without pause or rest. This extraordinary endurance stems from the heart’s unique muscular composition—cardiac muscle tissue that differs fundamentally from both skeletal muscle and smooth muscle found elsewhere in the body. Cardiac muscle cells contain exceptionally high concentrations of mitochondria, the cellular powerhouses that generate energy, reflecting the enormous metabolic demands of constant contraction. These cells are interconnected through specialized junctions called intercalated discs, allowing electrical signals to spread rapidly across the heart muscle and ensuring synchronized contractions that efficiently pump blood with each beat. Understanding this structural sophistication helps explain why the heart responds so profoundly to both nutritional support and exercise conditioning—it’s an organ built for performance but dependent on optimal fuel and regular challenge to maintain peak function.
The circulatory system extends far beyond the heart itself, comprising an intricate network of arteries, veins, and capillaries that collectively form a closed loop distributing oxygen and nutrients while removing metabolic waste products. Arteries carry oxygen-rich blood away from the heart under high pressure, their walls constructed with thick layers of smooth muscle and elastic tissue that allow them to expand with each heartbeat and maintain steady blood flow. These arterial walls are lined with a thin layer of endothelial cells that play crucial roles in regulating blood vessel diameter, preventing clot formation, and managing inflammation—functions that depend heavily on proper nutrition and are enhanced by regular exercise. As arteries branch into progressively smaller vessels, they eventually become capillaries so narrow that red blood cells must pass through single file, facilitating the exchange of oxygen and nutrients with surrounding tissues. The blood then collects in veins equipped with one-way valves that prevent backflow as it returns to the heart, completing the circuit and beginning the journey anew.
Shop on AliExpress via link: wholesale-sports-water-bottles
The physiological demands placed on the cardiovascular system vary dramatically based on activity level, creating windows of adaptation that can be harnessed through strategic exercise programming. At rest, the average adult heart pumps approximately five liters of blood per minute, a rate that can increase five-fold or more during intense physical activity. This dramatic scaling of cardiac output requires the heart muscle to adapt its contractile force, developing greater strength and efficiency through repeated exposure to increased demands. Similarly, blood vessels must learn to dilate more effectively during exercise, delivering increased blood flow to working muscles while maintaining adequate perfusion to vital organs. These adaptations don’t occur spontaneously—they require the combination of appropriate nutritional building blocks and the stimulus of regular physical challenge. The remarkable capacity for cardiovascular improvement, even in individuals starting from a deconditioned state, demonstrates the system’s inherent plasticity when provided with proper support.
The relationship between heart muscle strength and overall cardiovascular health extends beyond simple pumping capacity to encompass factors like electrical conduction stability, metabolic efficiency, and structural resilience. A well-conditioned heart develops a lower resting heart rate not through weakness but through improved stroke volume—the amount of blood ejected with each beat increases, allowing the same cardiac output to be achieved with fewer contractions. This enhanced efficiency reduces the total workload on the heart over time.
The electrical system coordinating heart contractions also benefits from proper conditioning, becoming more stable and less prone to dangerous arrhythmias that can trigger sudden cardiac events. Additionally, exercise-induced adaptations include the development of new capillaries within the heart muscle itself, improving oxygen delivery to cardiac tissue and enhancing its resilience against ischemic injury. These multifaceted improvements highlight why cardiovascular strengthening through nutrition and exercise represents such a powerful strategy for both disease prevention and health optimization.
The Foundation: Nutrition for Cardiovascular Strength
Nutrition serves as the cornerstone of cardiovascular health, providing not only the energy substrates that fuel each heartbeat but also the structural components necessary for maintaining and repairing cardiac tissue and blood vessels. The concept of “eating for heart health” has evolved considerably from the overly simplistic fat-restriction paradigms of previous decades to a more nuanced understanding that emphasizes food quality, dietary patterns, and the synergistic effects of whole foods rather than isolated nutrients. Contemporary nutritional science recognizes that the Mediterranean dietary pattern, characterized by abundant vegetables, fruits, whole grains, legumes, nuts, olive oil, and moderate amounts of fish and poultry, provides superior cardiovascular protection compared to low-fat approaches that often replace healthy fats with refined carbohydrates. This shift in understanding reflects growing appreciation for how different macronutrients and phytochemicals interact within the body to influence inflammation, oxidative stress, lipid metabolism, and vascular function—all critical determinants of cardiovascular health.
The macronutrient composition of one’s diet exerts profound effects on cardiovascular risk factors, though the relationships are more complex than traditional dietary guidance sometimes suggests. Regarding fats, mounting evidence indicates that replacing saturated fats with polyunsaturated fats reduces cardiovascular disease risk, while the wholesale elimination of dietary fats can prove counterproductive by reducing beneficial HDL cholesterol and increasing triglycerides. Omega-3 fatty acids, particularly the long-chain varieties found in fatty fish like salmon, mackerel, and sardines, demonstrate remarkable cardiovascular benefits including reduced inflammation, improved arterial flexibility, decreased blood clotting tendency, and stabilized heart rhythm. Carbohydrate quality matters enormously—whole grains, legumes, and intact fruits provide fiber and phytochemicals that support cardiovascular health, while refined grains and added sugars promote metabolic dysfunction and increase cardiovascular disease risk. Protein sources also carry significance, with plant-based proteins and fish generally offering superior cardiovascular profiles compared to processed meats, which have been consistently linked to elevated heart disease risk in epidemiological studies.
The role of specific nutrients in supporting cardiovascular function extends well beyond macronutrient ratios to encompass a range of vitamins, minerals, and phytochemicals that directly influence heart muscle and vascular health. Potassium and magnesium work synergistically to regulate blood pressure, maintain proper heart rhythm, and support healthy blood vessel function—deficiencies in either mineral can compromise cardiovascular health even in the presence of an otherwise adequate diet. The B-vitamin complex, particularly folate, B6, and B12, helps regulate homocysteine levels, an amino acid that when elevated promotes arterial damage and increases cardiovascular disease risk. Antioxidants including vitamins C and E, along with numerous polyphenolic compounds found in colorful fruits and vegetables, protect cardiovascular tissues from oxidative damage that accumulates with aging and metabolic stress. Notably, these protective compounds appear most effective when consumed as part of whole foods rather than isolated supplements, suggesting that the matrix of nutrients and phytochemicals found in natural foods creates synergistic benefits that cannot be fully replicated through supplementation alone.
Dietary patterns that have demonstrated consistent cardiovascular benefits in research studies share common characteristics that extend beyond any single nutrient or food group. The Mediterranean diet emphasizes plant-based foods, healthy fats from olive oil and nuts, moderate fish consumption, and limited red meat, creating a nutritional profile rich in fiber, antioxidants, omega-3 fatty acids, and anti-inflammatory compounds. The DASH (Dietary Approaches to Stop Hypertension) eating plan, originally designed to lower blood pressure, similarly emphasizes fruits, vegetables, whole grains, lean proteins, and low-fat dairy while limiting sodium, saturated fat, and added sugars. Both approaches have been extensively studied and consistently demonstrate reductions in cardiovascular disease risk, improvements in blood pressure and cholesterol profiles, and decreased inflammation markers. Importantly, these dietary patterns prove sustainable for many individuals precisely because they don’t rely on extreme restriction or elimination of entire food categories but rather emphasize shifting proportions toward more nutrient-dense, minimally processed options while allowing flexibility and cultural adaptation.
The timing and frequency of eating may influence cardiovascular health beyond the simple composition of meals, though research in this area continues to evolve. Some evidence suggests that eating patterns characterized by regular meal times and avoidance of late-night eating may support better cardiovascular outcomes, potentially through effects on circadian rhythm alignment and metabolic regulation. The practice of intermittent fasting has gained attention for potential cardiovascular benefits, though current evidence remains insufficient to recommend specific fasting protocols for heart health promotion. What appears clear is that erratic eating patterns, particularly those involving frequent consumption of energy-dense, nutrient-poor foods throughout the day, promote metabolic dysfunction and increase cardiovascular disease risk. Establishing regular eating routines that emphasize nutrient-dense whole foods during active hours and allow extended overnight fasting periods aligns with natural metabolic rhythms and may optimize cardiovascular function, though individual responses vary considerably based on genetics, activity patterns, and overall health status.
Essential Nutrients That Build Heart Muscle
Omega-3 fatty acids stand among the most extensively researched nutrients for cardiovascular health, with decades of scientific investigation revealing their multifaceted benefits for both heart muscle and the broader circulatory system. The two primary omega-3s of interest—EPA (eicosapentaenoic acid) and DHA (docosahexaenoic acid)—are found predominantly in fatty fish and exert powerful anti-inflammatory effects by competing with omega-6 fatty acids in cellular membrane composition and subsequent eicosanoid synthesis. These long-chain omega-3s become incorporated into cardiac cell membranes, where they influence electrical signaling and help stabilize heart rhythm, potentially reducing the risk of dangerous arrhythmias that can trigger sudden cardiac death. Additionally, omega-3 fatty acids reduce triglyceride levels, decrease blood clot formation tendency, improve arterial flexibility, and may modestly reduce blood pressure—collectively creating a cardiovascular risk profile that numerous studies have associated with reduced heart attack and stroke incidence. While omega-3 supplementation through fish oil capsules has produced mixed results in clinical trials, regular consumption of fatty fish appears consistently protective, suggesting that whole food sources may provide additional beneficial compounds or that omega-3s work synergistically with other nutrients present in fish.
Antioxidant nutrients and phytochemicals form a critical line of defense against oxidative stress, a pathological process that damages cardiovascular tissues and accelerates atherosclerosis development. Free radicals generated through normal metabolism, environmental exposures, and inflammation attack cellular structures including lipids, proteins, and DNA, with particularly harmful effects in the cardiovascular system where oxidized LDL cholesterol becomes a key driver of arterial plaque formation. Vitamins C and E function as direct antioxidants, neutralizing free radicals before they can cause damage, while countless polyphenolic compounds found in colorful plant foods provide complementary antioxidant protection through various mechanisms. Berries, particularly blueberries, contain anthocyanins that protect endothelial cells lining blood vessels and improve vascular function. Dark leafy greens provide lutein and other carotenoids that accumulate in arterial walls and reduce atherosclerotic plaque progression. The flavonoids in cocoa, tea, and certain fruits demonstrate impressive abilities to enhance nitric oxide production, a critical molecule that promotes blood vessel dilation and prevents platelet aggregation. The consistent finding that diets rich in colorful plant foods protect against cardiovascular disease likely reflects the combined actions of hundreds of these protective compounds working synergistically rather than any single antioxidant nutrient.
The mineral duo of potassium and magnesium deserves special attention for their critical roles in maintaining cardiovascular health, yet both remain significantly under-consumed in typical Western diets. Potassium functions as nature’s blood pressure regulator, promoting sodium excretion through the kidneys and directly relaxing blood vessel walls—effects that explain why potassium-rich diets consistently demonstrate lower cardiovascular disease rates in population studies. The modern diet’s heavy reliance on processed foods, which are typically low in potassium but high in sodium, creates an imbalanced ratio that promotes hypertension and cardiovascular strain. Magnesium participates in over three hundred enzymatic reactions throughout the body, including those governing heart muscle contraction, blood vessel tone, and electrical conduction in cardiac tissue. Magnesium deficiency, which may affect a substantial portion of the population despite not always manifesting in standard blood tests, can contribute to hypertension, arrhythmias, and vascular dysfunction. Excellent food sources of both minerals include leafy greens, legumes, nuts, seeds, whole grains, and various fruits and vegetables—precisely the foods emphasized in heart-healthy dietary patterns and notably absent from highly processed food products that dominate many modern diets.
Dietary fiber represents another crucial nutrient for cardiovascular health, though it often receives less attention than more glamorous compounds like omega-3s or antioxidants. Soluble fiber, found abundantly in oats, barley, legumes, and many fruits, binds to cholesterol-containing bile acids in the digestive tract and promotes their excretion, thereby lowering blood cholesterol levels. This mechanism explains why foods like oatmeal have earned reputation as heart-healthy options—regular consumption demonstrably reduces LDL cholesterol and cardiovascular disease risk. Insoluble fiber, while not directly affecting cholesterol, supports cardiovascular health through effects on weight management, blood sugar control, and gut microbiome composition. Recent research has revealed that gut bacteria ferment fiber into short-chain fatty acids that exert anti-inflammatory effects and may influence blood pressure regulation through complex mechanisms involving the nervous system and kidney function. The average adult consumes only about half the recommended daily fiber intake, representing a significant missed opportunity for cardiovascular disease prevention. Increasing fiber consumption through whole plant foods rather than processed products fortified with isolated fiber provides not only the fiber itself but also the full complement of nutrients and phytochemicals that make these foods protective.
Healthcare professionals emphasize that comprehensive approaches combining dietary fiber with other heart-protective nutrients create the most substantial cardiovascular benefits. Educational resources provide detailed guidance on implementing these evidence-based strategies into daily routines, helping individuals understand not just what changes to make but how to sustain them over time. The integration of professional medical advice with lifestyle modifications ensures that cardiovascular disease prevention efforts align with individual health needs and medical considerations.
Specific amino acids and their dietary sources have emerged as important considerations for cardiovascular health, particularly regarding the amino acid homocysteine and the nutrients required for its metabolism. Elevated homocysteine levels damage arterial walls and increase cardiovascular disease risk, yet can often be normalized through adequate intake of folate, vitamin B6, and vitamin B12—nutrients that facilitate homocysteine conversion to less harmful compounds. Dietary sources of these B-vitamins include leafy greens, legumes, whole grains, lean meats, fish, and fortified foods, though supplementation may be necessary for certain populations including older adults who absorb B12 less efficiently. Another amino acid derivative, L-arginine, serves as the precursor for nitric oxide synthesis in endothelial cells, making it crucial for healthy blood vessel function. While the body can synthesize arginine, dietary intake from sources like nuts, seeds, seafood, and legumes may support optimal nitric oxide production and vascular health. The amino acid taurine, found primarily in seafood and available through supplements, demonstrates cardiovascular benefits including blood pressure reduction and improved heart muscle function, though more research is needed to establish optimal intake levels. These examples illustrate how even specific amino acids, often overshadowed by discussions of protein quantity, can significantly influence cardiovascular health when consumed as part of a varied, nutrient-dense diet.
Exercise Strategies for Cardiovascular Enhancement
Aerobic exercise forms the foundation of any cardiovascular strengthening program, utilizing rhythmic, repetitive movements of large muscle groups to elevate heart rate and increase oxygen consumption over sustained periods. Activities like brisk walking, jogging, cycling, swimming, and dancing create training stimuli that prompt the cardiovascular system to adapt through multiple mechanisms. During aerobic exercise, the heart must pump faster and more forcefully to deliver oxygen-rich blood to working muscles, creating a training effect that over time increases the heart’s stroke volume—the amount of blood ejected with each contraction. This adaptation allows a trained heart to deliver the same cardiac output at lower heart rates, reducing the total number of beats over a lifetime and decreasing cardiovascular stress. Simultaneously, blood vessels adapt by improving their ability to dilate in response to increased blood flow demands, a process mediated by enhanced nitric oxide production in endothelial cells. The muscle tissue itself develops increased capillary density, allowing more efficient oxygen extraction from blood and reducing the cardiovascular system’s workload during both exercise and daily activities. These adaptations accumulate progressively with consistent training, explaining why individuals who maintain regular aerobic activity for years demonstrate markedly superior cardiovascular function compared to sedentary peers.
Laboratory investigations have meticulously documented the molecular mechanisms through which physical training remodels cardiovascular tissues at the cellular level. These studies reveal that exercise triggers specific genetic expression patterns that enhance mitochondrial function, improve calcium handling within cardiac cells, and stimulate beneficial adaptations in blood vessel responsiveness. The translation of this basic science into practical exercise recommendations continues to refine our understanding of optimal cardiovascular effects of exercise across different age groups and fitness levels.
Building healthy muscle mass requires strategic nutrition that provides sufficient calories and protein to support tissue growth while maintaining cardiovascular wellness. Individuals starting from lower body weights face unique challenges in achieving muscle development without compromising metabolic health or cardiovascular function. Balanced approaches that emphasize nutrient-dense foods and progressive resistance training can help build lean tissue while supporting overall health markers including those related to heart function and circulatory efficiency.
The intensity at which aerobic exercise is performed significantly influences the specific adaptations that occur, with both moderate-intensity continuous training and high-intensity interval training offering distinct cardiovascular benefits. Moderate-intensity aerobic exercise, typically defined as activity that elevates heart rate to sixty to seventy percent of maximum while still allowing conversation, provides the most accessible entry point for most individuals and produces robust cardiovascular improvements when performed regularly. This intensity range promotes sustainable adaptations in mitochondrial density, capillary growth, and cardiac output capacity without excessive stress that might discourage continued participation. High-intensity interval training, alternating short bursts of near-maximal effort with recovery periods, has gained attention for producing substantial cardiovascular improvements in less total training time compared to continuous moderate-intensity work. These intense intervals push the cardiovascular system to its limits, triggering adaptations in cardiac contractility, maximal oxygen uptake, and metabolic efficiency that complement those achieved through longer, steadier efforts. Research suggests that incorporating both training approaches—moderate-intensity sessions for building aerobic capacity and high-intensity intervals for pushing cardiovascular limits—creates optimal improvements in heart muscle strength and overall cardiovascular fitness.
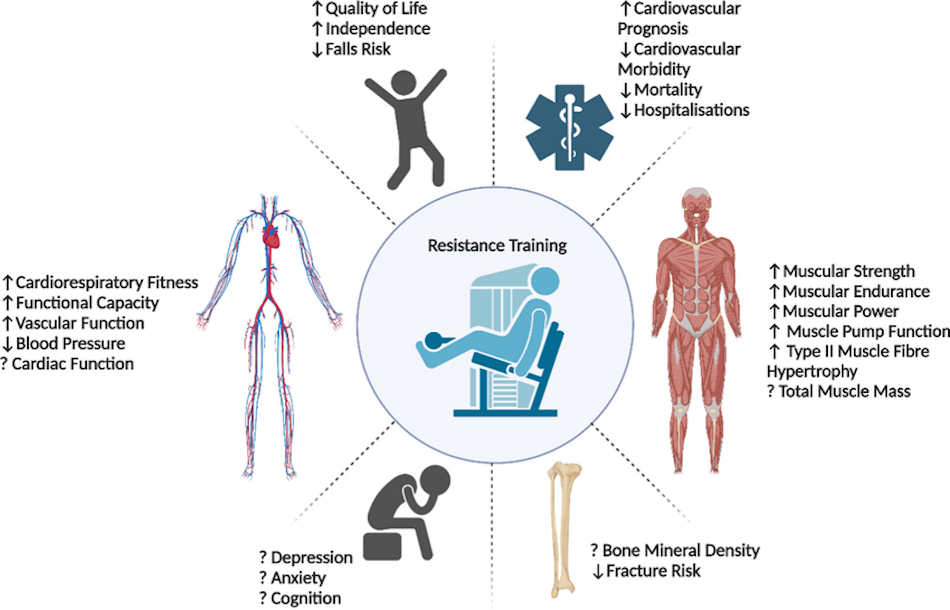
Resistance training, once considered primarily a tool for building muscular strength and size, has gained recognition for its significant cardiovascular benefits that complement those achieved through aerobic exercise. While resistance exercise doesn’t typically elevate heart rate as dramatically or sustainably as aerobic work during the training session itself, it produces important adaptations including improved insulin sensitivity, enhanced lipid profiles, reduced blood pressure, and favorable changes in body composition that collectively support cardiovascular health. The mechanism behind these benefits appears multifaceted—increased muscle mass raises resting metabolic rate, improving the body’s ability to manage glucose and lipids, while the acute metabolic demands of resistance training create beneficial stress responses in cardiovascular tissues. Recent research has revealed that resistance training promotes beneficial cardiac remodeling, increasing left ventricular wall thickness in a physiological pattern associated with improved cardiac function rather than the pathological thickening seen in certain disease states. Additionally, the blood pressure reductions observed with regular resistance training rival those achieved through aerobic exercise, particularly when training incorporates higher repetitions with moderate loads rather than exclusively heavy lifting with low repetitions. Contemporary exercise guidelines recognize these cardiovascular benefits by recommending that adults engage in muscle-strengthening activities at least twice weekly in addition to regular aerobic exercise.
Medical research facilities have examined precisely how different training modalities affect cardiac structure and function, revealing that strategic combination of movement types produces superior outcomes compared to single-approach programs. The cardiovascular system responds to varied physical demands by developing multiple adaptive capabilities that collectively enhance both performance capacity and disease resistance. Understanding exercise and heart principles allows individuals to design training routines that maximize heart-strengthening benefits while minimizing unnecessary strain or injury risk.
The emerging understanding of how different exercise modalities complement each other has led to integrated training approaches that combine aerobic work, resistance training, and flexibility exercises into comprehensive programs optimized for cardiovascular health. Concurrent training, which systematically incorporates both aerobic and resistance sessions throughout the week, appears to produce superior overall cardiovascular outcomes compared to either approach alone. The aerobic component primarily drives improvements in cardiac output, oxygen transport capacity, and endurance performance, while resistance work enhances metabolic health, body composition, and muscular fitness—factors that indirectly but substantially influence cardiovascular disease risk. Flexibility and mobility work, though not directly cardiovascular in nature, support injury prevention and movement quality that facilitates consistent participation in more intense training modalities. A well-designed weekly program might include three to four days of aerobic training varying in intensity and duration, two to three days of resistance training targeting all major muscle groups, and daily mobility work to maintain joint health and movement efficiency. The specific distribution depends on individual goals, fitness levels, and recovery capacity, but the principle remains constant: comprehensive cardiovascular strengthening requires diverse training stimuli that challenge the system through multiple mechanisms.
Recovery periods between exercise sessions represent critical windows for adaptation, during which the cardiovascular system rebuilds and strengthens in response to the training stimulus. The common misconception that more exercise always equals better results overlooks the fundamental principle that adaptation occurs during recovery, not during the training itself. Exercise creates a controlled stress that disrupts cardiovascular homeostasis, triggering molecular signals that prompt tissue remodeling and functional improvements. However, these beneficial changes only manifest if adequate recovery time, nutrition, and sleep allow the reconstruction processes to occur. Insufficient recovery between intense training sessions can lead to overtraining syndrome, characterized by elevated resting heart rate, decreased performance, increased susceptibility to illness, and paradoxically, reduced cardiovascular fitness despite continued training. The optimal balance between training stress and recovery varies considerably between individuals based on factors including age, fitness level, genetics, nutrition status, and life stress, but general principles apply: beginners require more recovery time between sessions compared to experienced exercisers, higher-intensity workouts demand longer recovery periods than moderate efforts, and signs of incomplete recovery—persistently elevated morning heart rate, unusual fatigue, or performance decrements—should prompt additional rest before resuming intense training.
Combining Nutrition and Exercise for Maximum Impact
The synergistic relationship between nutrition and exercise creates cardiovascular benefits that exceed the sum of their individual effects, a phenomenon extensively documented in research comparing different lifestyle intervention approaches. Studies examining diet-only, exercise-only, and combined diet-plus-exercise interventions consistently demonstrate that the integrated approach produces superior improvements in cardiovascular risk factors including blood pressure, cholesterol profiles, insulin sensitivity, and inflammatory markers. This synergy operates through multiple mechanisms—exercise increases muscle glucose uptake and improves the body’s ability to utilize dietary nutrients effectively, while proper nutrition provides the substrates necessary for exercise adaptations and recovery. The Mediterranean dietary pattern combined with regular physical activity, for instance, has demonstrated remarkable cardiovascular disease prevention in numerous large-scale studies, reducing heart attack and stroke incidence by forty to fifty percent compared to sedentary individuals following typical Western dietary patterns. This multiplicative effect explains why comprehensive lifestyle interventions prove so powerful for both primary prevention of cardiovascular disease and secondary prevention in those who have already experienced cardiac events.
Nutrient timing relative to exercise sessions can influence both performance during training and recovery adaptations afterward, though the practical significance varies based on training intensity, duration, and individual metabolic characteristics. Pre-exercise nutrition serves primarily to ensure adequate energy availability, preventing hypoglycemia during prolonged or intense training sessions and optimizing performance. For moderate-intensity aerobic exercise lasting less than sixty minutes, most individuals perform well relying on their normal meal patterns without specific pre-exercise fueling strategies. Longer or more intense sessions benefit from consuming easily digestible carbohydrates one to three hours before exercise, providing readily available glucose without causing digestive discomfort. Post-exercise nutrition assumes particular importance for recovery and adaptation, with the hours immediately following exercise representing a window of enhanced nutrient uptake and utilization. Consuming a combination of carbohydrates and protein within two hours after training supports glycogen replenishment, reduces muscle protein breakdown, and provides amino acids for tissue repair—factors that collectively enhance recovery and facilitate the adaptations that strengthen cardiovascular function. While competitive athletes may need to optimize these timing strategies precisely, most individuals pursuing cardiovascular health will realize the majority of benefits simply by maintaining overall diet quality and ensuring adequate nutrition throughout the day surrounding their training sessions.
Hydration status profoundly affects cardiovascular function during exercise and recovery, yet many individuals chronically consume insufficient fluids to support optimal performance and adaptation. Even mild dehydration decreases blood volume, forcing the heart to work harder to maintain cardiac output and deliver oxygen to tissues. During exercise, fluid losses through sweat can substantially reduce blood volume, elevating heart rate and cardiovascular strain while impairing temperature regulation and exercise performance. The cardiovascular system’s efficiency depends on adequate blood volume to maintain venous return to the heart, fill the cardiac chambers adequately, and eject blood forcefully with each contraction—processes all compromised by dehydration. Beyond exercise sessions, chronic mild dehydration may contribute to elevated blood pressure and increased cardiovascular disease risk through effects on kidney function and blood viscosity. Individual fluid needs vary widely based on factors including body size, sweat rate, environmental conditions, and exercise intensity, but general guidelines suggest consuming enough fluid to maintain pale yellow urine color and replacing fluid losses during prolonged exercise by drinking regularly throughout the session. For cardiovascular health purposes, water remains the optimal beverage choice for most situations, providing hydration without added sugars, caffeine, or other compounds that may compromise health when consumed in excess.
The role of body composition in cardiovascular health extends beyond simple weight management to encompass the distribution and metabolic activity of different tissue types. Visceral adipose tissue—fat stored around internal organs rather than beneath the skin—produces inflammatory molecules and hormones that directly damage cardiovascular tissues and promote metabolic dysfunction. The combination of nutrition and exercise proves particularly effective for reducing visceral fat accumulation, with exercise demonstrating a preferential effect on this dangerous fat depot compared to subcutaneous fat. Lean muscle mass, conversely, supports cardiovascular health through its metabolic activity—muscle tissue consumes glucose and fatty acids, helping regulate blood sugar and lipids while producing beneficial molecules called myokines that reduce inflammation and support vascular function. The synergistic effects of resistance training and protein-adequate nutrition on muscle mass maintenance or development, combined with aerobic exercise and overall caloric balance for fat loss, create favorable body composition changes that substantially reduce cardiovascular disease risk independent of total body weight changes. This finding explains why fitness level and metabolic health predict cardiovascular outcomes better than body mass index alone—two individuals at the same weight may have vastly different cardiovascular risk profiles based on their muscle mass, visceral fat accumulation, and physical fitness.
Lifestyle Factors That Support Heart Health
Sleep quality and duration exert profound influences on cardiovascular health through mechanisms affecting inflammation, metabolic regulation, blood pressure, and autonomic nervous system balance. Chronic sleep deprivation, defined as regularly obtaining less than seven hours per night, has been consistently associated with elevated cardiovascular disease risk in population studies, with some research suggesting that both short and excessively long sleep durations correlate with increased heart disease incidence. During sleep, blood pressure normally decreases by ten to twenty percent compared to waking levels, a phenomenon called “nocturnal dipping” that appears essential for cardiovascular health—individuals who fail to exhibit this nighttime blood pressure reduction demonstrate higher rates of cardiovascular events. Sleep also regulates hormones affecting appetite and metabolism, with insufficient sleep promoting increased food intake, particularly of energy-dense foods, and impairing glucose regulation in ways that increase diabetes and cardiovascular disease risk. The relationship between sleep and cardiovascular health operates bidirectionally—sleep disorders like obstructive sleep apnea directly damage the cardiovascular system through repeated episodes of oxygen deprivation and blood pressure surges during the night, while cardiovascular disease can disrupt sleep through discomfort, anxiety, or medication side effects. Prioritizing consistent sleep schedules, creating conducive sleep environments, and addressing sleep disorders when present represent important components of comprehensive cardiovascular disease prevention that complement nutrition and exercise interventions.
Stress management emerges as a critical but often overlooked factor in maintaining cardiovascular health, as chronic psychological stress triggers a cascade of physiological responses that directly damage the heart and blood vessels. The stress response evolved to mobilize resources for immediate physical threats, increasing heart rate and blood pressure, releasing glucose into the bloodstream, and promoting blood clotting—responses that proved adaptive for our ancestors facing predators but become maladaptive when triggered constantly by modern psychological stressors. Chronic activation of these stress pathways elevates blood pressure, promotes inflammation, encourages atherosclerotic plaque development, and increases the risk of cardiac arrhythmias and acute cardiovascular events. Additionally, stress often drives unhealthy coping behaviors including poor dietary choices, physical inactivity, smoking, and excessive alcohol consumption that compound cardiovascular risk. Exercise itself functions as a powerful stress management tool, reducing stress hormone levels, improving mood through endorphin release, and providing psychological benefits through enhanced self-efficacy and social connection when performed in group settings. Other evidence-based stress reduction approaches including meditation, yoga, deep breathing exercises, and cognitive behavioral therapy demonstrate cardiovascular benefits both through direct physiological effects on blood pressure and heart rate variability and through improvements in health behaviors. Incorporating regular stress management practices alongside nutrition and exercise interventions creates a more comprehensive approach to cardiovascular strengthening and disease prevention.
Social connections and community engagement contribute to cardiovascular health through both psychological and behavioral pathways that research is only beginning to fully elucidate. Large population studies have consistently found that individuals with strong social ties demonstrate lower cardiovascular disease mortality rates compared to socially isolated peers, even after accounting for traditional risk factors like smoking, blood pressure, and cholesterol levels. The mechanisms underlying this protective effect appear multifaceted—social support reduces psychological stress and its harmful cardiovascular consequences, while social connections may promote healthier behaviors through modeling and accountability. Group exercise classes, walking groups, or recreational sports leagues combine the cardiovascular benefits of physical activity with social connection, potentially amplifying the protective effects of each. Additionally, having a sense of purpose and engagement in meaningful activities appears protective against cardiovascular disease, possibly through effects on stress physiology and health-promoting behaviors. These findings highlight the importance of viewing cardiovascular health holistically, recognizing that even the most optimized nutrition and exercise programs operate within broader contexts of psychological wellbeing, social connection, and life satisfaction that influence health outcomes through complex pathways.
Environmental factors including air quality, noise pollution, and access to green spaces influence cardiovascular health in ways that often go unrecognized but can substantially affect disease risk, particularly for individuals living in urban environments. Air pollution exposure, even at levels commonly experienced in many cities, accelerates atherosclerosis development, increases blood pressure, promotes arrhythmias, and elevates heart attack and stroke risk through inflammatory and oxidative stress mechanisms. Chronic noise exposure, particularly from traffic, similarly increases cardiovascular disease risk through stress pathway activation and sleep disruption. Conversely, access to green spaces and natural environments appears protective, associated with lower blood pressure, reduced stress, and increased physical activity levels. These environmental influences interact with individual nutrition and exercise behaviors—air pollution may reduce the cardiovascular benefits of outdoor exercise during high-pollution periods, while access to safe, pleasant outdoor spaces facilitates physical activity and stress reduction. Awareness of these environmental factors allows individuals to make informed choices about when and where to exercise, potentially choosing indoor activities during air quality alerts while maximizing outdoor exercise during favorable conditions. For broader cardiovascular disease prevention at the population level, these findings support urban planning approaches that prioritize air quality, reduce noise pollution, and ensure equitable access to green spaces and safe environments for physical activity.
Monitoring Progress and Measuring Success
Tracking cardiovascular fitness improvements requires monitoring multiple parameters that collectively reflect the heart muscle’s strength and the circulatory system’s efficiency. Resting heart rate serves as one of the most accessible indicators of cardiovascular adaptation, with regular aerobic training typically producing gradual reductions as the heart develops increased stroke volume and requires fewer beats per minute to maintain adequate circulation at rest. Well-trained endurance athletes may exhibit resting heart rates in the low forties or fifties, compared to the average untrained adult range of seventy to eighty beats per minute, though genetic factors influence individual baselines considerably. Heart rate recovery—the speed at which heart rate decreases following exercise cessation—provides another valuable fitness marker, with faster recovery indicating better cardiovascular conditioning and autonomic nervous system function. Blood pressure responses to exercise and during recovery similarly reflect cardiovascular health, with well-conditioned individuals demonstrating more appropriate blood pressure increases during activity and quicker returns to baseline afterward. More sophisticated assessments including maximal oxygen consumption testing, which measures the body’s peak ability to transport and utilize oxygen during exercise, offer precise quantification of cardiovascular fitness but require specialized equipment and expertise typically available only in research or clinical settings.
Biomarkers measured through blood tests provide objective data regarding cardiovascular health status and responses to lifestyle interventions. Standard lipid panels assessing total cholesterol, LDL cholesterol, HDL cholesterol, and triglycerides offer crucial information about cardiovascular disease risk, with favorable changes in these markers typically appearing within six to twelve weeks of implementing comprehensive nutrition and exercise programs. More advanced lipid testing can evaluate LDL particle size and number, providing additional insight into cardiovascular risk beyond standard cholesterol measurements. Hemoglobin A1C testing reveals average blood sugar control over the preceding three months, detecting prediabetes or diabetes that substantially elevate cardiovascular disease risk. Inflammatory markers including high-sensitivity C-reactive protein correlate with cardiovascular disease risk and may improve with lifestyle interventions, though their utility for monitoring individual progress remains debated. Measuring these biomarkers at baseline and periodically during lifestyle modification programs provides tangible evidence of progress that can motivate continued adherence, while also identifying individuals who may benefit from additional interventions beyond lifestyle approaches to achieve optimal cardiovascular risk profiles.
Subjective measures of exercise capacity and daily function often demonstrate improvements before objective cardiovascular parameters show significant changes, providing early feedback that encourages continued program adherence. Many individuals report increased energy levels, reduced fatigue during daily activities, and improved sleep quality within the first few weeks of starting regular exercise programs, even before measurable changes appear in cardiovascular markers. Exercise performance itself improves noticeably—distances that initially required significant effort become manageable, recovery between exercise intervals shortens, and the subjective perception of exertion decreases for any given workload. These functional improvements reflect genuine cardiovascular adaptations including enhanced oxygen delivery, improved metabolic efficiency, and better neuromuscular coordination, even when not yet captured by formal fitness testing. Documenting these subjective improvements through training logs or simple performance benchmarks—time required to walk a standard distance, number of stairs climbed without breathlessness, or perceived recovery after routine activities—provides valuable feedback that complements objective health measurements and reinforces the connection between lifestyle behaviors and meaningful health outcomes.
Technology has expanded options for cardiovascular health monitoring, with wearable devices offering continuous tracking of heart rate, activity levels, sleep patterns, and other metrics relevant to cardiovascular fitness. Heart rate monitors integrated into fitness watches or chest straps allow real-time exercise intensity management, ensuring training sessions target appropriate zones for desired adaptations. Activity trackers encourage movement throughout the day, addressing the growing recognition that prolonged sedentary behavior increases cardiovascular disease risk independent of structured exercise participation. Sleep tracking features, while not always perfectly accurate, can identify patterns and potential sleep disturbances that may warrant further evaluation. However, the proliferation of tracking technology also carries risks of excessive focus on metrics at the expense of listening to body signals, potential anxiety from minor fluctuations in tracked parameters, and overreliance on devices rather than developing internal awareness of effort levels and recovery status. Used judiciously, these technologies can enhance cardiovascular strengthening programs by providing objective feedback and identifying trends over time, but they function best as tools supporting rather than replacing thoughtful attention to overall health and wellbeing.
The ultimate measure of successful cardiovascular strengthening extends beyond any single metric to encompass improved quality of life, enhanced functional capacity, and reduced risk of cardiovascular events and mortality. While biomarkers and fitness tests provide valuable feedback, the practical benefits of cardiovascular health manifest in daily life through increased vitality, greater resilience to physical and psychological stressors, reduced medication requirements for those managing cardiovascular risk factors, and enhanced ability to engage in meaningful activities without physical limitations. Long-term studies tracking individuals who maintain healthy nutrition and exercise patterns demonstrate not only reduced cardiovascular disease incidence but also compression of morbidity—the period of life affected by disability and disease becomes shorter, allowing more years of active, healthy living. These broad health outcomes, while harder to quantify in the short term compared to changes in cholesterol or exercise performance, represent the true goal of cardiovascular strengthening efforts and justify the sustained commitment required to maintain healthy lifestyle patterns across decades of life.
Frequently Asked Questions
Question 1: How does nutrition strengthen the heart muscle?
Answer 1: Nutrition strengthens the heart muscle through multiple interconnected mechanisms that support cellular function, reduce inflammation, and optimize metabolic processes. Specific nutrients provide the raw materials necessary for cardiac tissue maintenance and repair, with protein supplying amino acids for contractile protein synthesis, while omega-3 fatty acids become incorporated into cell membranes where they influence electrical signaling and reduce arrhythmia risk. Antioxidants protect cardiac cells from oxidative damage that accumulates through normal metabolism and environmental stressors, helping preserve cellular integrity and function over time. Minerals like potassium and magnesium regulate heart rhythm and contractile force, with deficiencies in either potentially compromising cardiac performance. Beyond these direct effects on heart muscle cells, nutrition influences cardiovascular health through impacts on blood lipids, blood pressure, inflammation, and vascular function—factors that collectively determine the heart’s workload and long-term health. The synergistic effects of consuming whole foods rich in these protective nutrients explain why dietary patterns like the Mediterranean diet demonstrate such powerful cardiovascular benefits, creating an internal environment that supports optimal heart muscle function throughout life.
Question 2: What types of exercise are best for cardiovascular health?
Answer 2: Aerobic exercises that elevate heart rate and sustain increased oxygen consumption for extended periods provide the most direct cardiovascular strengthening benefits, with activities like brisk walking, running, swimming, cycling, and dancing all offering excellent options depending on individual preferences and physical capabilities. These rhythmic, large-muscle-group movements challenge the cardiovascular system to deliver increased blood flow and oxygen, prompting adaptations including enhanced cardiac output, improved blood vessel function, and increased metabolic efficiency. Research supports both moderate-intensity continuous training and high-intensity interval training as effective approaches, with the optimal choice depending on individual fitness levels, time availability, and specific health goals. Resistance training complements aerobic work by improving body composition, enhancing insulin sensitivity, and promoting favorable changes in cholesterol profiles, with contemporary guidelines recommending muscle-strengthening activities at least twice weekly in addition to regular aerobic exercise. The most effective cardiovascular strengthening programs incorporate variety across these training modalities while maintaining consistency over time, as the cumulative adaptations from sustained regular activity provide far greater benefits than sporadic intense efforts separated by long inactive periods.
Comprehensive fitness programs addressing multiple health domains simultaneously produce more substantial long-term benefits than narrowly focused interventions targeting single outcomes. Modern approaches integrate cardiovascular training with strength development, flexibility work, and recovery practices into cohesive programs that support overall wellness. These integrated strategies reflect current understanding that optimal health emerges from balanced attention to diverse fitness components rather than exclusive focus on any single training modality or health metric.
Question 3: Can diet alone improve heart health without exercise?
Answer 3: Dietary modifications alone can produce meaningful improvements in cardiovascular health markers including cholesterol levels, blood pressure, inflammatory indicators, and blood sugar control, with research demonstrating that adopting heart-healthy eating patterns reduces cardiovascular disease risk even in the absence of structured exercise programs. Nutritional interventions work primarily through metabolic pathways—improving lipid profiles, reducing oxidative stress, decreasing inflammation, and supporting healthy blood pressure—creating an internal environment more conducive to cardiovascular health. However, exercise provides unique cardiovascular benefits that nutrition alone cannot replicate, including direct strengthening of the heart muscle through increased contractile demands, enhanced blood vessel flexibility through improved endothelial function, and development of increased capillary density that improves oxygen delivery to tissues. The combination of nutrition and exercise produces synergistic effects that exceed the sum of their individual contributions, with studies consistently showing that integrated lifestyle interventions yield superior cardiovascular outcomes compared to either approach in isolation. For individuals unable to engage in formal exercise due to physical limitations or medical conditions, dietary optimization remains highly valuable and can substantially improve cardiovascular health, though the addition of even modest physical activity when possible provides additional protective benefits that enhance overall health trajectories.
Question 4: How long does it take to see improvements in heart health?
Answer 4: The timeline for cardiovascular improvements varies considerably depending on which specific parameters are measured, with some beneficial changes occurring within days while others develop gradually over months or years of sustained healthy behaviors. Blood pressure often begins declining within two to three weeks of implementing lifestyle modifications including dietary changes and regular exercise, providing relatively rapid feedback that interventions are working. Improvements in cholesterol profiles typically become apparent within six to eight weeks for those relying on lifestyle approaches alone, though individuals taking cholesterol-lowering medications may see changes more quickly. Measurable increases in cardiovascular fitness, reflected in parameters like exercise capacity and resting heart rate reductions, generally require eight to twelve weeks of consistent training to become noticeable, though subjective improvements in energy and exercise tolerance often appear within the first month. More substantial structural changes to heart muscle and blood vessels, including increased cardiac stroke volume, enhanced arterial flexibility, and reduced atherosclerotic plaque burden, develop progressively over many months to years of sustained healthy lifestyle patterns. These longer-term adaptations accumulate gradually but ultimately produce the most significant health benefits, reducing cardiovascular disease risk and improving overall vitality in ways that become increasingly apparent as healthy habits become integrated into daily life over extended periods.
Question 5: What foods should I avoid for better heart health?
Answer 5: Foods requiring limitation or avoidance for optimal cardiovascular health primarily include those high in saturated fats, trans fats, added sugars, and excessive sodium—compounds that promote inflammation, arterial damage, elevated cholesterol, and increased blood pressure. Processed meats including bacon, sausages, hot dogs, and deli meats consistently demonstrate associations with elevated cardiovascular disease risk in research studies, likely due to their high saturated fat and sodium content along with preservatives and other additives. Trans fats, while largely removed from the food supply in many countries through regulatory action, may still appear in some commercially baked goods and should be avoided entirely due to their particularly harmful effects on cholesterol profiles. Sugar-sweetened beverages provide concentrated calories without nutritional value while promoting insulin resistance and weight gain, making them prime candidates for elimination from heart-healthy diets. Highly processed snack foods, fried items, and baked goods made with refined grains and unhealthy fats contribute to cardiovascular risk through multiple mechanisms including promotion of weight gain, adverse effects on cholesterol, and increased inflammation. Rather than viewing heart-healthy eating primarily through a restrictive lens of foods to avoid, emphasizing positive dietary changes—increasing consumption of vegetables, fruits, whole grains, legumes, nuts, and fish while naturally displacing less healthy options—creates sustainable eating patterns that support long-term cardiovascular health without requiring rigid avoidance of all less-optimal foods.
Clinical nutrition experts have developed practical frameworks for implementing dietary modifications that reduce cardiovascular risk factors without requiring extreme restriction or complicated meal planning. These approaches recognize that sustainable change occurs through gradual shifts toward healthier options rather than abrupt elimination of familiar foods. The strategies emphasize enhancing diet quality through addition of protective foods, naturally displacing less beneficial choices while maintaining eating patterns that fit individual lifestyles and preferences through heart disease diet guidance.
Question 6: Is it safe to exercise with existing heart problems?
Answer 6: Exercise can be not only safe but highly beneficial for many individuals with diagnosed cardiovascular conditions when appropriately prescribed and monitored, with cardiac rehabilitation programs demonstrating remarkable success in improving outcomes for heart disease patients through supervised exercise training combined with risk factor management. However, the specific safety considerations and exercise recommendations vary substantially based on the type and severity of cardiac condition, making medical consultation essential before beginning any exercise program for those with known heart disease. Conditions including stable coronary artery disease, controlled heart failure, and recovered myocardial infarction typically benefit from carefully progressed exercise programs that improve cardiovascular fitness and quality of life while potentially reducing future event risk. Certain situations require more cautious approaches or temporary exercise restriction, including unstable angina, severe valvular disease, uncontrolled arrhythmias, and acute cardiac events, with medical evaluation determining when exercise can safely resume and at what intensity. Cardiac rehabilitation programs provide ideal environments for individuals with heart disease to begin exercise under professional supervision, with continuous monitoring during initial sessions and gradual progression based on individual responses and capabilities. For those with cardiac conditions exercising independently after medical clearance, awareness of warning symptoms requiring immediate medical attention—including chest pain, severe breathlessness, dizziness, or palpitations—remains crucial, along with adherence to prescribed intensity limits and medication regimens that support safe exercise participation.
Question 7: What role do omega-3 fatty acids play in heart health?
Answer 7: Omega-3 fatty acids, particularly the long-chain varieties EPA and DHA found predominantly in fatty fish, exert multiple beneficial effects on cardiovascular health through their incorporation into cell membranes and subsequent influences on inflammation, blood clotting, heart rhythm, and vascular function. These essential fats compete with omega-6 fatty acids in producing signaling molecules called eicosanoids, with omega-3-derived eicosanoids generally promoting less inflammation and reduced blood clotting compared to those derived from omega-6 sources, creating a cellular environment more favorable for cardiovascular health. Omega-3 fatty acids stabilize cardiac electrical activity by influencing ion channel function in heart muscle cells, potentially reducing the risk of dangerous arrhythmias that can trigger sudden cardiac death in susceptible individuals. Additionally, these fats lower triglyceride levels, modestly reduce blood pressure, improve arterial flexibility, and may slow the progression of atherosclerotic plaque development. Population studies consistently show that individuals consuming fatty fish regularly demonstrate lower cardiovascular disease mortality rates compared to those rarely eating fish, with some research suggesting particular benefits for preventing sudden cardiac death and reducing heart failure risk. While omega-3 supplementation through fish oil capsules has produced inconsistent results in clinical trials examining cardiovascular outcomes, the evidence supporting regular consumption of omega-3-rich foods like salmon, mackerel, sardines, and herring remains robust, suggesting these whole food sources provide the most reliable cardiovascular benefits possibly through synergistic effects with other nutrients present in fish.
Question 8: How does stress affect heart health and circulation?
Answer 8: Chronic psychological stress triggers a complex cascade of physiological responses that directly damage cardiovascular tissues while promoting behaviors that compound cardiovascular disease risk, making stress management an essential component of comprehensive heart health strategies. When the brain perceives stress, it activates the sympathetic nervous system and hypothalamic-pituitary-adrenal axis, releasing stress hormones including adrenaline and cortisol that increase heart rate, elevate blood pressure, promote glucose release into the bloodstream, and enhance blood clotting—responses that evolved to mobilize resources for immediate physical threats but become maladaptive when chronically activated by modern psychological stressors. Prolonged elevation of these stress responses damages arterial walls, promotes atherosclerotic plaque development, increases inflammation throughout the body, and elevates the risk of dangerous cardiac arrhythmias and acute cardiovascular events including heart attacks and strokes. Stress also influences cardiovascular health indirectly through its effects on health behaviors, with stressed individuals more likely to engage in emotional eating, choose nutrient-poor comfort foods, reduce physical activity, smoke cigarettes, consume excessive alcohol, and experience sleep disturbances—all factors that independently increase cardiovascular disease risk. The relationship between stress and heart health operates bidirectionally, as individuals with cardiovascular disease often experience increased stress and anxiety related to their condition, potentially creating a vicious cycle where stress worsens heart health which in turn increases stress levels. Effective stress management approaches including regular exercise, meditation, yoga, deep breathing practices, adequate sleep, social connection, and professional counseling when needed demonstrate measurable cardiovascular benefits including reduced blood pressure, improved heart rate variability, decreased inflammation, and better overall cardiovascular disease outcomes.
Question 9: Can heart damage be reversed through lifestyle changes?
Answer 9: While the extent to which cardiac damage can be reversed depends heavily on the type, severity, and duration of existing injury, research increasingly demonstrates that comprehensive lifestyle modifications can produce substantial improvements in cardiovascular structure and function even in individuals with established heart disease. Studies utilizing advanced imaging techniques have documented regression of atherosclerotic plaques in coronary arteries following intensive lifestyle interventions combining very low-fat or Mediterranean-style diets with regular exercise, stress management, and smoking cessation, particularly when individuals achieve significant improvements in cholesterol levels and blood pressure. The heart muscle itself demonstrates remarkable plasticity in response to appropriate lifestyle changes—individuals with heart failure who participate in supervised exercise rehabilitation programs often show improvements in cardiac contractile function, exercise capacity, and quality of life, though complete normalization of severely damaged hearts rarely occurs. Blood vessel function responds particularly well to lifestyle interventions, with improvements in endothelial-dependent vasodilation—a critical marker of vascular health—appearing within weeks to months of adopting healthier eating patterns and regular physical activity. Areas of prior damage from myocardial infarction leave permanent scars, but the remaining viable heart muscle can strengthen and compensate, partially offsetting functional limitations when supported by optimal nutrition, appropriate exercise conditioning, and medical management. The critical importance of early intervention cannot be overstated—lifestyle changes implemented before significant irreversible damage occurs offer the greatest potential for complete recovery, while those with advanced disease may achieve stabilization and functional improvements but face permanent limitations. These realities emphasize the value of prevention through lifelong healthy habits while also providing hope that meaningful improvements remain possible even for those beginning lifestyle modifications with existing cardiovascular damage.
Question 10: What nutrients are most important for circulatory system health?
Answer 10: The circulatory system’s health depends on a constellation of nutrients that collectively support blood vessel structure, regulate vascular tone, prevent pathological clot formation, protect against oxidative damage, and maintain healthy blood composition. Nitric oxide precursors including dietary nitrates found abundantly in leafy green vegetables and beetroot support blood vessel dilation and healthy blood flow, with the body converting these compounds into nitric oxide that relaxes vascular smooth muscle and prevents platelet aggregation. Vitamin K2, distinct from vitamin K1 involved in blood clotting, plays crucial roles in directing calcium away from arterial walls and into bones, potentially preventing the vascular calcification that stiffens arteries and increases cardiovascular risk. Antioxidant vitamins C and E along with polyphenolic compounds from colorful plant foods protect endothelial cells lining blood vessels from oxidative damage that promotes atherosclerosis and vascular dysfunction. B-vitamins including folate, B6, and B12 regulate homocysteine metabolism, preventing accumulation of this amino acid that damages arterial walls when present in excess. Minerals including magnesium and potassium influence vascular smooth muscle tone and blood pressure regulation, with adequate intake supporting healthy blood vessel relaxation and optimal circulation. Essential fatty acids, particularly omega-3s, become incorporated into endothelial cell membranes where they influence inflammation, blood clotting tendency, and overall vascular function. The interconnected nature of these nutrients highlights why whole food dietary patterns rich in vegetables, fruits, whole grains, nuts, fish, and healthy oils provide superior circulatory system support compared to isolated nutrient supplementation, as these foods deliver complementary compounds that work synergistically to maintain the complex network of vessels comprising the circulatory system.
Conclusion
The journey toward strengthening the heart muscle and optimizing circulatory system function represents one of the most impactful investments an individual can make in their long-term health and quality of life. The evidence accumulated over decades of cardiovascular research paints a clear and compelling picture—the combination of strategic nutrition and regular exercise produces profound beneficial changes in cardiac structure and function that dramatically reduce disease risk while enhancing vitality across the lifespan. These interventions work through multiple complementary mechanisms, with nutrition providing the molecular building blocks necessary for tissue maintenance and repair while exercise creates the physiological stimuli that drive adaptive strengthening. The synergistic effects of these approaches exceed what either can achieve independently, creating cardiovascular improvements that manifest in measurable biomarker changes, enhanced functional capacity, and ultimately, reduced rates of heart attacks, strokes, and cardiovascular mortality.
Research institutions have extensively documented how regular movement strengthens cardiac tissue through multiple biological pathways. When moderate and vigorous activities become consistent habits rather than occasional efforts, the heart muscle develops enhanced pumping efficiency that reduces long-term cardiovascular strain. These physical activity benefits extend beyond exercise sessions to influence how the entire circulatory network responds to daily demands, creating resilience that protects against future cardiac events.
Sarah’s story, which opened this exploration, illustrates both the challenges and possibilities inherent in cardiovascular strengthening through lifestyle modification. Her initial cardiac event, while frightening, became the catalyst for transformative changes that not only restored her health but optimized it beyond her previous baseline. The comprehensive approach she embraced—combining evidence-based nutrition emphasizing whole foods and healthy fats with a varied exercise program incorporating both aerobic and resistance training—produced improvements that extended well beyond simple risk factor reduction. Her experience reflects a fundamental truth validated by countless research studies and clinical observations: the cardiovascular system possesses remarkable capacity for positive adaptation when supported by appropriate nutrition and regular physical challenge, regardless of an individual’s starting point or previous health history.
The practical implementation of cardiovascular strengthening principles requires neither perfection nor extreme measures but rather sustained commitment to progressively healthier choices across multiple domains of daily life. Beginning with manageable modifications—perhaps adding one additional serving of vegetables daily or incorporating a fifteen-minute walk into the daily routine—creates momentum that facilitates subsequent changes as improved energy and wellbeing provide tangible reinforcement of healthy behaviors. The key lies in viewing cardiovascular health not as a destination reached through temporary dietary restriction or exercise bursts but as an ongoing practice woven into the fabric of daily living, where healthy choices become increasingly automatic and enjoyable through repetition and positive feedback. This sustainable approach, supported by regular monitoring of progress and periodic consultation with healthcare providers, creates the foundation for lifelong cardiovascular wellness that adapts and evolves alongside changing life circumstances and physical capabilities.
Looking forward, the integration of emerging research and technologies promises to enhance our ability to strengthen cardiovascular systems with ever-greater precision and effectiveness. Advances in nutrigenomics may eventually enable personalized dietary recommendations based on individual genetic profiles, optimizing nutrition strategies for cardiovascular protection. Wearable technologies continue evolving to provide more sophisticated monitoring of cardiovascular responses to exercise and daily activities, potentially allowing real-time adjustments that maximize training effectiveness while minimizing injury risk. Growing understanding of the gut microbiome’s influence on cardiovascular health may reveal new dietary approaches that leverage beneficial bacterial metabolism to enhance heart protection. Despite these exciting developments, the fundamental principles remain constant—cardiovascular health flourishes when supported by nutrient-dense whole foods, regular physical activity that appropriately challenges the system, adequate recovery including sufficient sleep, effective stress management, and supportive social connections. These timeless elements of healthy living, validated repeatedly by scientific investigation and clinical experience, provide the foundation upon which emerging innovations will build, creating ever more powerful and personalized approaches to cardiovascular disease prevention and heart muscle strengthening.
Articles related:
Tags
📧 Get More Articles Like This
Subscribe to receive product reviews and buying guides in your inbox!
We respect your privacy. Unsubscribe at any time.